This QA testing property of the WellStar
ARTICLE CARDS
US4563
ENABLED PAGINATION vertical limit -5 TEXT ALIGN-CENTER Test FOR PROD 7/15/25 48301
.jpg?rev=0c641d247be3492db97099991e0fef7f)
To celebrate Women’s Health Month, more than 150 executives gathered Thursday at The Studio Theatre in Sandy Springs for insightful discussions on advancing women’s health in Atlanta and throughout Georgia.
The Women's Health Summit, presented by the Atlanta Business Chronicle and Wellstar Health System, featured two panels of experts and a keynote address by renowned health and wellness expert Emma Lovewell.
Cheryl Preheim, anchor at 11Alive (WXIA), welcomed attendees and served as a moderator.
;
For more than a year, our communities have done their part to fight COVID-19.
We have stayed home, worn masks when we’ve gone out, been extra careful with washing our hands and avoided large gatherings. That’s meant that holidays and birthdays have looked a little different, all so we can stay safe and healthy.
The separation and fear have been draining, and many of us have dealt with loneliness and stress as we worry about our health and our loved ones.
But now we have something to celebrate. Hope has arrived in the form of the COVID-19 vaccine. All Georgians age 12 or older are now eligible to get their shots.
At Wellstar, we've chosen to lead by example. Across our health system, frontline healthcare workers and leadership have "stuck it to COVID." Whether they want to gather with friends and family, travel to a new destination or help protect vulnerable members of the community, our Wellstar team members all have their #MyWhy — the reason they chose to get vaccinated.
For Dr. Jeffrey Hines, chief of gynecologic oncology for Wellstar, getting the shot was about a sense of responsibility. As medical director of the Wellstar Center for Health Equity, Dr. Hines works to ensure our underserved populations have access to the care they need to stay safe and healthy. He got the COVID-19 vaccine to protect those around him.
“I’m a father, I’m a husband, I’m a brother and I’m a grandfather, and it’s important for me to protect my family,” Dr. Hines said. “I understand the science, and the science is important, but equally important to me is I want to be a trusted voice to people in the community who are most at risk for this and perhaps may have the most questions.”
Dr. Sophia McIntyre, senior vice president of Wellstar Medical Group, also said she got her shot to stop the spread, noting that COVID-19 has disproportionately affected minority communities.
“The reason why I got the COVID-19 vaccine is to ensure that I’m doing my part to bend the curve,” Dr. McIntyre said. “We know that African Americans and Latino Americans are dying at a higher proportion.”
Dr. Danny Branstetter, Wellstar’s medical director for infection prevention, has been at the forefront of Wellstar’s work to fight COVID-19 and keep our communities safe. Now, he wants to see life return to normal, because health isn’t just about your body. It’s also about your personal connections and overall well-being.
“I’m tired of being separated from my friends and family. I’m tired of seeing small businesses fold,” Dr. Branstetter said. “I’m tired of seeing the increased burden this places on those without resources. I’m tired of the loneliness this puts on those who are isolated and the elderly. My question is, aren’t you tired, too?”
All of us play a part in ending this pandemic.
“We’re in this together, and we can end this together through vaccination,” Dr. Branstetter said.
To find a vaccination site near you, visit the Georgia Department of Public Health website or local retail pharmacy.
;

Christmas carols and telephones ringing filled the Wellstar Children’s Hospital of Georgia lobby December 7 through December 9, 2023 for the 23rd annual iHeartMedia Cares for Kids Radiothon.
Thanks to the generosity of supporters, a check for $262,693 was presented to Wellstar Children’s at the conclusion of Radiothon on Saturday, December 9.
Throughout the event, radio stations 104.3 WBBQ, 96.3 Kiss-FM and 105.7 The Bull broadcast live from the lobby while WRDW News 12/NBC 26 shared stories of hope. Families of pediatric patients who have successfully finished treatment or are undergoing treatment at Wellstar Children’s, which is a member of the Children’s Miracle Network, stopped by to share stories of the world-class care their children received from the caring staff and expert caregivers.
“Every dollar that’s raised this weekend with Radiothon stays right here at Wellstar Children’s Hospital of Georgia and directly benefits the care of the children,” said Pediatrician-in-Chief Dr. Valera Hudson. “We’re the second largest children’s hospital in Georgia and the only children’s hospital outside of Atlanta. We offer the highest level of care to the sickest and most complex children. We hope you never need us, but if you ever need us, we’re here.”
Donations to Radiothon are used to purchase much-needed items that are unique to a children’s hospital, such as a vein finder for the neonatal intensive care unit. This device shines a red light through an infant’s arm or leg and helps caregivers find their tiny veins without having to stick them with a needle multiple times to administer fluids and medications.
The funds are also used to provide additional supplies for patient care as needs arise.
Though Radiothon is over, pledges are accepted year-round by calling (706) 721-4004 or by visiting the Cares for Kids Radiothon website.
;
Christmas music and cheers filled the halls of Wellstar Children’s Hospital of Georgia Dec. 5 through 7 as listeners and viewers of local iHeartMedia radio stations and WRDW-TV generously supported patients and families for the 24th consecutive year.
In the end, the community pledged $255,612 to support Wellstar Children’s.
iHeartMedia generously donated the 72 hours of airtime to the cause while three of its popular radio stations—104.3 WBBQ, 96.3 Kiss FM and 105.7 The Bull—and WRDW News 12/NBC 26 broadcast live from the hospital.
“The children’s hospital could not survive without the support of the community. I’m just so grateful for everyone’s support,” said Dr. Valera Hudson, pediatrician-in-chief of Wellstar Children’s. “No children’s hospital thrives without philanthropy; 100% of the money that’s raised is used directly to help the children we take care of here. All of the funds stay right here at the Wellstar Children’s Hospital of Georgia.”
Wellstar Children’s is a not-for-profit hospital with specialists who care for pediatric patients with a range of conditions, including the most complex conditions.
Some of the patients who have been treated at Wellstar Children’s shared their stories with DJs and reporters throughout Radiothon. For example, 9-year-old Kensley Woodberry began developing spots on her hands and feet that became so painful, she could no longer walk. She stopped eating and refused to play. A team of specialists at Wellstar Children’s diagnosed her with juvenile dermatomyositis, a rare autoimmune disease that causes the body to attack its own muscles and leads to inflammation throughout the body.
This past summer, Kensley attended Camp Joint Venture, a summer camp for children with rheumatic conditions. It gives kids like Kensley the opportunity to enjoy the summer camp experience while a team of medical personnel is nearby in case they are needed. The camp is one of several summer camps funded through Radiothon.
Radiothon also allows for purchases of comfort items like Zaky Hugs, which mimic the warmth and security of a parent’s touch for babies in the NICU; red wagons for transporting young patients around the hospital; and sensory toys for children with autism. These are only a few of the items that bring joy, comfort or care to young patients that the hospital could not purchase without community support.
Though Radiothon has concluded, donations can be made throughout the year by calling (706) 721-4004, by emailing Wellstar Children’s Director of Philanthropy Catherine Stewart or through the Cares for Kids Radiothon website.
;
The iHeartMedia Cares for Kids Radiothon filled the lobby of Wellstar Children’s Hospital of Georgia Dec. 4 through 6 for its 25th year of fundraising. Surrounded by a winter wonderland of Christmas trees and red, white and silver balloon arches, volunteers took donations from generous supporters while iHeartMedia radio stations and WRDW-TV broadcast stories of the miracles that happen every day at Wellstar Children’s Hospital of Georgia.
The event raised $291,617 to support the children’s hospital, which is a part of the Children’s Miracle Network.
“Thank you, thank you, thank you! This is life-changing,” said Ralph Turner, president of Wellstar MCG Health Medical Center. “This can support many of our young patients. They come to us and we take care of them. We don’t turn them away, and this really helps support our mission.”
Dr. Valera Hudson, pediatrician-in-chief, echoed Turner’s gratitude.
“We couldn’t do this without community support. We are so grateful for everyone who is here who helped pull this off,” she said.
Each year, iHeartMedia generously donates 72 hours of airtime as DJs from 96.3 Kiss FM, 104.3 WBBQ and 105.7 The Bull join WRDW-TV to broadcast live from the event, sharing success stories from patients and families grateful for the care they received.
“Thank you, CSRA, for making miracles happen. Exactly 291,617 miracles. Thank you!” said Ivy Elam, market president of iHeartMedia in Augusta.
Donations from the iHeartMedia Cares for Kids Radiothon are used throughout the year to purchase pediatric equipment such as vein finders for babies in the neonatal intensive care unit and a gaming system for patients in the pediatric operating room.
They also support programs that are unique to a children’s hospital. These include the facility dog program, featuring three hospital-owned dogs who provide comfort and help Child Life Specialists more easily communicate with young patients. Donations also help fund summer camps for children living with chronic conditions—such as Camp Rainbow for cancer patients—which allow kids to just be kids while remaining under medical supervision.
Radiothon has ended, but donations can be made throughout the year by calling (762) 375-4004, by emailing Wellstar Children’s Hospital of Georgia Director of Philanthropy Catherine Stewart or by visiting the Wellstar Foundation.
;
Hepatitis B vaccine
What it does: Protects your baby from Hepatitis B, a virus that attacks the liver and can cause lifelong infection Why it’s important: Hepatitis B isn’t just a risk for adults later in life. Most importantly for newborns, the virus can be passed from mother to baby during childbirth. Studies show that up to 75% of mothers with chronic Hepatitis B don’t know they’re infected—and 90% of infants who catch the virus during delivery will develop a chronic infection. Chronic Hepatitis B can lead to serious liver disease, cancer or even death. What to expect: The Hepatitis B vaccine is a series of three doses given at birth, 1 month and 6 months. Side effects are rare, other than mild soreness at the injection site.Beyfortus (RSV protection)
What it does: Shields your baby from RSV (respiratory syncytial virus), a common virus that can be much more serious in infants Why it’s important: For most adults, RSV feels like a mild cold. But for newborns—especially those born prematurely—RSV can sometimes lead to serious lung infections and hospitalization. In severe cases, babies may need breathing support in the hospital. Beyfortus provides antibodies that protect your baby through their first RSV season. What to expect: One injection lasts about five to six months. The most common side effects are pain, redness or swelling at the injection site. Studies show Beyfortus reduces the risk of severe RSV illness by about 85% to 90%. Extra protection tip: Moms can also receive an RSV vaccination late in pregnancy, which helps pass antibodies to their newborns. Keeping siblings and visitors with colds away from newborns—and encouraging good handwashing—are other ways to help protect your baby.Vitamin K shot
What it does: Gives your baby the vitamin needed to help blood clot and prevent dangerous bleeding Why it’s important: Babies are born with very little vitamin K, and breastmilk and formula don’t provide enough. Without the shot, newborns are at risk for vitamin K deficiency bleeding—a rare but serious condition that can cause internal bleeding in places like the brain and intestines. These bleeds can happen suddenly and may lead to life-altering complications. What to expect: The vitamin K shot has been safely given to newborns in the U.S. since the 1960s, with no significant side effects. If you have questions about newborn immunizations, speak with your baby’s pediatrician. At Wellstar Children’s of Georgia, we’re here to partner with you through every stage of your child’s life.;
The gynecologic oncologists at Wellstar care for women at all stages of life, treating a variety of conditions with compassion and offering advanced care options. Our team are experts in treating cancers such as uterine, ovarian, cervical, vaginal and vulvar cancers. Here, we answer common questions about gynecologic cancer care with the help of Dr. Rosa Miller Polan, a gynecologic oncologist at Wellstar Cobb Medical Center.
What is a gynecologic oncologist?
Gynecologic oncologists are specialists trained in the multidisciplinary management of patients with cancers of the female reproductive tract. Trained originally in obstetrics and gynecology, gynecologic oncologists treat patients with complex benign gynecologic issues, as well as gynecologic cancer patients who may need surgery, chemotherapy, immunotherapy or a combination of different treatments.
When should you seek care?
Gynecologic cancers have different warning signs. When a person experiences concerning symptoms, a physical exam, including a pelvic exam, should be performed. Cervical and vaginal cancer symptoms include abnormal vaginal discharge, vaginal bleeding and pain. The most common warning sign for uterine cancer is abnormal vaginal bleeding. In postmenopausal women, any bleeding or spotting is abnormal and should prompt an evaluation.
Ovarian or fallopian tube cancer symptoms include bloating, constipation, pelvic or abdominal pain and difficulty eating or feeling full quickly. Vulvar cancer symptoms include itching, burning, discoloration, and new bumps or lumps on the skin outside of the vagina.
Who is at risk for developing gynecologic cancer?
Women who smoke cigarettes are at elevated risk for cervical, vaginal and vulvar cancer development. People who are immunosuppressed and those who have tested positive for the human papillomavirus (HPV) are also at increased risk. Genetics can contribute to the development of uterine, ovarian or fallopian tube cancers and these types of cancers can run in families. Obesity and use of hormone replacement therapy can put women at risk for the development of uterine, ovarian and fallopian tube cancers. A history of infertility, endometriosis and pelvic radiation are also risk factors for developing gynecologic cancer.
What services are available at Wellstar?
At Wellstar, gynecologic oncologists provide comprehensive care for patients with gynecologic cancers, including administering chemotherapy and performing surgeries when needed. As high-volume pelvic surgeons, gynecologic oncologists also care for patients who need elective and emergent complex benign gynecologic surgery.
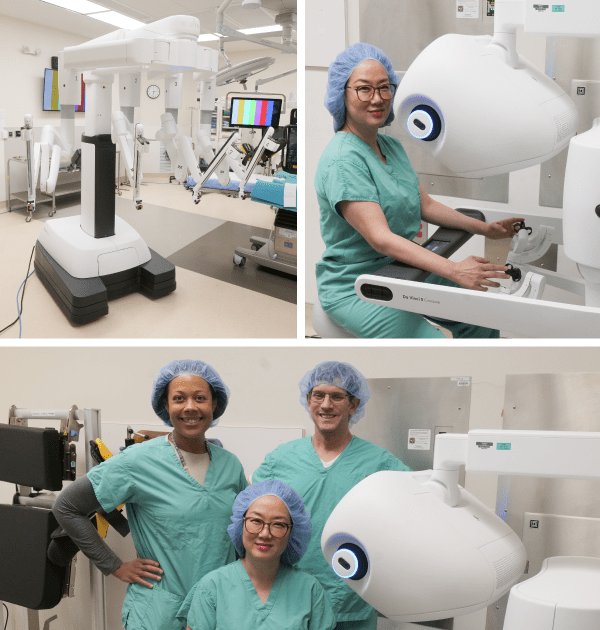
For many patients, robotic-assisted surgery offers a minimally invasive approach with less associated blood loss, shorter hospital stays and fewer post-operative complications. Gynecologic oncologists are some of the top users of the innovative DaVinci 5 robotic surgery platform. Performing complex gynecologic cancer surgeries, minimally invasive or otherwise, requires the type of highly specialized and multidisciplinary teams that work at Wellstar—and an infrastructure of resources to ensure patients have access to best-in-class care in their own backyard.
Learn more about gynecologic oncology at Wellstar at wellstar.org/gyncancer.

By Dr. Joanna Dolgoff, Wellstar pediatrician
When school is in session, finding the perfect after-school snack that balances nutrition and deliciousness can feel like quite a task. As a board-certified Wellstar pediatrician, I understand the importance of fueling growing bodies with the right nutrients. With that, I'm excited to share five wholesome after-school snack ideas that are easy to make and fun for kids to eat.
1. Celery Caterpillars
This creative snack recipe offers a good balance of protein from peanut butter, along with a variety of fruits and vegetables, providing essential vitamins and antioxidants for growing children.
What You’ll Need:
Peanut butter
Celery
Grapes
Blueberries
Grape tomatoes
Candy eyes
Directions:
- Fill stalks of celery with peanut butter.
- Place grapes, blueberries or grape tomatoes atop celery sticks. These will be the body and head of your caterpillars.
- Apply peanut butter to the backs of candy eyes, then place eyes on grape, tomato or blueberry to create face.
- Optional: Cut thin matchsticks from a celery stick and place behind candy eyes to create the antennae.
2. Apple Sailboats
This recipe is excellent for kids as it combines the crisp sweetness of apples, a good source of fiber and vitamins, with protein-rich peanut butter and the added crunch of Cheerios to create a tasty and nutritionally balanced snack. Toothpicks may be a choking hazard for children, so supervise as your family makes and enjoys this snack.
What You’ll Need:
One apple
Peanut butter
Cheerios
Low-fat cheese
Toothpicks
Directions:
- Cut apple in half and remove the apple’s core.
- Spread peanut butter across the flat side of your apple halves.
- Place Cheerios on top of peanut butter spread.
- Using a thick slice of cheese, cut triangular sails for your apple boats.
- Attach sail to boat using toothpick.
3. Krazy Kabobs
This krazy kabob recipe is a playful and nutritious way to encourage children to enjoy a variety of fruits. Filled with hydrating watermelon, sweet cantaloupe, refreshing honeydew, juicy pineapple, antioxidant-rich blueberries and grapes, these skewers provide a spectrum of vitamins and flavors, promoting a fun and healthy snacking experience for young taste buds.
What You’ll Need:
Watermelon
Cantaloupe
Honeydew
Pineapple
Blueberries
Grapes
Wood skewers
Fruit-shape cutters (stars, hearts, etc.)
Directions:
- Cut horizontal slices of your larger fruits (watermelon, cantaloupe and honeydew).
- Use your fruit cutters to cut shapes out of your fruit slices.
- Place any creative combination of fruits or fruit shapes onto your skewer to create the ultimate krazy kabob.
4. Veggie Cars
This wholesome veggie car recipe is a fun way to encourage children to enjoy their vegetables. With vibrant baby peppers and baby cucumbers, the snack not only provides essential vitamins, but also engages kids in a fun, hands-on experience of assembling their own veggie cars, promoting both healthy eating and interactive play. Toothpicks may be a choking hazard for children.
What You’ll Need:
10 baby peppers
Six baby cucumbers
Toothpicks
Directions:
- Slice cucumbers into half-inch rounds, discarding the ends. These will be your wheels.
- Place two toothpicks through each pepper. The toothpicks will serve as the axels to your cars.
- Push one cucumber round onto the ends of each toothpick to form the full car.
5. Banana Lollipops
These banana lollipops offer a delightful and healthier alternative to traditional sweets. With the natural sweetness of bananas and the richness of dark chocolate, the recipe makes for an enjoyable, nutritious after-school snack for kids of all ages.
What You’ll Need:
One banana
Chopped dark chocolate bar
Popsicle sticks
Wax paper and baking sheet
- Unpeel banana and slice into inch-thick rounds, discarding the ends.
- Insert one popsicle stick into each round.
- Place chopped dark chocolate into microwave-safe bowl and heat until melted.
- Dip each banana round into chocolate.
- Place popsicles onto wax paper-covered baking sheet and let freeze for 45 minutes.
As a pediatrician dedicated to the well-being of children, these snack ideas offer more than delicious bites—they pave the way for a lifetime of healthy habits. Incorporating a variety of fruits and vegetables, these recipes not only provide essential vitamins and minerals, but also engage young minds in the joy of preparing and enjoying wholesome foods. Learn more about how to keep your kids happy and healthy by scheduling an appointment with a world-class Wellstar pediatrician today.
A graduate of New York University Grossman School of Medicine, Dr. Joanna Dolgoff is a board-certified pediatrician with Wellstar.
Wellstar’s content, and all related media, are provided for educational and informational purposes only and does not constitute providing medical advice or professional services. Consult a pediatrician for the diet that’s best for your child.
;
Small changes add up to big results. By incorporating simple habits into your life, you can kickstart your wellness journey and stay on track for the long run.
Setting healthy, realistic goals
Use the SMART goal-setting system to help define your goal and develop attainable resolutions.
- Specific—Be clear about exactly what you want to accomplish. Include as many details as necessary, such as potential obstacles or extra requirements.
- Measurable—Measure your progress and determine how to meet the goal. If you have a big goal, you may need to set smaller milestones to stay on track.
- Achievable—Attainability is an important factor to consider when it comes to goal setting. “While behavior change comes with any resolution, it is unfair to yourself if you set a goal that is not feasible,” said Dr. Rebecca Gomez, Wellstar clinical health psychologist and Clinician Resiliency & Well-Being Program lead.
- Relevant—Align your resolutions with your overall life goals and think about what you hope to accomplish by reaching that goal.
- Time bound—Set a realistic, target deadline to reach your goal with checkpoints at intervals along the way. Markers provide an opportunity to measure progress and reassess any changes needed to stay on track.
Keep in mind, you may encounter some bumps in the road along the way. Recognizing all the small accomplishments can help you stay motivated and win in the long run.
“Focus on what small steps you’ve accomplished rather than how far you have to go,” Dr. Gomez shared. “Also, have a resiliency plan to help you bounce back after a more challenging day.”
Build new habits into your regular routine by beginning small and adding on over time. With this “habit stacking” technique, you pair your new habit with something you’re already doing. For example, if your goal is to drink more water, drink a glass of water while making your morning coffee or tea.
Schedule a wellness exam
Seeing your primary care clinician at least once a year is the single most important thing you can do for your health.
At your annual exam, your care team will help keep you healthy and reach your wellness goals. They screen for diseases to stay ahead of medical issues and check in on your overall well-being.
Set a reminder on your phone or calendar to prompt you to book an appointment. You can also use an important date, such as your birthday, anniversary or a holiday, as a marker to remind you to schedule a visit.
Get moving to stay well
If you’re focused on improving your fitness routine, put a plan in place to be more active.
“Begin to incorporate a little more exercise into your daily routine,” said Wellstar Primary Care Physician Dr. Jeremy Boyd. “The Centers for Disease Control and Prevention offers a suggestion of 150 minutes of aerobic activity a week. I like to break that down to a good 40 minutes four times a week.”
Set a sleep routine
Having a bedtime routine is essential to catch more Zs throughout the year. When you wake up feeling rested, you often feel more productive and energized throughout the day.
Get started by setting a specific time to go to sleep—and stick to it. Make sure you reserve at least seven to nine hours per night for sleep.
Limit your screen time before getting in bed. Bright screens from a phone, computer or TV can keep your brain awake and make it harder to fall asleep.
If you’re having trouble getting to sleep, have a decaffeinated cup of tea or take a warm bath to help you relax.
Eat a balanced diet
When it comes to losing weight, many people look for a quick fix, which can often create unhealthy ways of eating. Creating a healthy eating plan from the start can help avoid any fad diet pitfalls.
Nutrition plans that restrict or eliminate food groups and those with extreme calorie deficits are difficult to maintain and can often produce more weight gain or undesired results, according to Wellstar Registered Dietitian Kelly Prian.
Diet trends can also create a negative relationship with food, which can make it harder to achieve your goals. Prian shared that those with long-term success focus on maintaining a plan that enables steady weight loss over time.
A healthy nutrition plan is balanced and emphasizes whole foods, such as fruits and vegetables, lean proteins, low fat dairy, nuts and seeds, and whole grains.
Try not to overcomplicate healthy eating. You can start by filling half your plate with vegetables or having fun trying new recipes.
Take care of your mental health
Self-care is an important aspect of your mental well-being and should be made a consistent part of each day.
“Make self-care a priority and a non-negotiable,” Dr. Gomez said.
“Think of self-care as a form of personal healing and a way to strengthen resilience,” Dr. Gomez explained. “Much like the way exercise enhances physical health, self-care enhances mental health.”
According to Dr. Gomez, it can be helpful to turn tasks we do on “autopilot” into more meaningful experiences.
“When washing your hands, give yourself a hand massage,” Dr. Gomez shared. “When driving, use red lights to practice deep breathing. Listen to a book on tape or language lessons rather than the radio or call someone to reconnect.”
If you feel overwhelmed by stress or anxiety, Wellstar behavioral health specialists are here for you.
“Working with a mental health provider is different than speaking with a friend or even a life coach,” Dr. Gomez said. “Mental health professionals are trained and licensed to address psychological or emotional wellness.”
Need support? Connect with a Wellstar behavioral health specialist.
;
Pay attention to early signs of stress.
Recognizing stress early is key to managing it effectively. When stress becomes chronic, it can affect both your mental and physical health. Learning to identify warning signs can help you take action before it escalates. This is true across all areas of life, including the workplace, where job stress can quietly build over time and lead to more serious mental health concerns if left unaddressed. “Paying attention to feelings of emotional exhaustion and general cynicism is important,” said Dr. Ryan Breshears, a board-certified clinical health psychologist and chief behavioral health officer at Wellstar. “Those are the foundational signs of occupational burnout, which certainly affects our well-being in the workplace, but when unchecked, can also spill over into our personal lives.” That spillover can show up as irritability, mood changes, social withdrawal or insomnia. “Any of those could point to a problem that warrants intervention,” Dr. Breshears said.Treat your whole health to support your mental well-being.
Mental and physical health are deeply interconnected—and we shouldn’t treat them in silos. At Wellstar, integrated care is a key part of our approach. “I think the days of talking about problems that are physical problems versus mental problems are over,” said Dr. Breshears. “We have a body of research now and decades of science that show the interplay between the physical and the emotional.” He explained that changes in thinking patterns can trigger physiological shifts in heart rate, stress hormone levels and more. Recognizing these mind-body connections can help you take a more proactive approach to your mental health. “Wellstar is making a concerted effort to deconstruct old ideas about mental health and remove barriers to access,” Dr. Breshears added. “For example, we’re bringing behavioral health into primary care, cardiac care, pediatrics and women’s health. We want to strategically integrate behavioral health services wherever patients are receiving care.” By treating the whole person and bringing behavioral health into every corner of healthcare, Wellstar is helping people take charge of their well-being in a way that’s compassionate, connected and convenient.Prioritize recovery.
Stress is inevitable, and recovery is essential. Without it, your mind and body stay in overdrive, increasing your risk for burnout and long-term health issues. Taking time to recover is not a sign of weakness—it’s a strategy for resilience. “Our bodies are designed to return to baseline, what we call homeostasis, after high-stress periods,” Dr. Breshears said. “Research suggests it's often the failure to prioritize recovery, not the stress itself, that actually contributes to the most lasting problems.” Dr. Breshears shared a study comparing elite marathon runners to non-elite runners. The surprising finding? Elite runners were better at identifying stress early and adjusting their pace to recover, ultimately helping them perform better. That same principle can apply to your mental health. If you notice signs of stress—like fatigue, irritability or changes in focus—take time to reset. That might mean getting more sleep, going for a walk, reaching out to a friend or seeking professional support. Being intentional about recovery helps you maintain balance, build resilience and continue showing up for what matters most.Nurture relationships and workplace well-being.
Meaningful relationships are a powerful buffer against stress. For many people, the workplace is a central source of community—and a critical place to nurture mental health. “We’re social creatures,” said Dr. Breshears. "Having environments where people come in and feel good about their day-to-day interactions is really important.” Dr. Breshears said it starts with employers being committed to understanding the inadvertent threats to their team’s well-being and removing barriers to care. “First, I think we have to pay attention to the occupational drivers of stress on our employees and commit to resolving those issues,” he explained. “All of the human resources and benefits in the world will fail if we’re not also working upstream to eliminate the root causes. Secondly, we need to establish clear pathways so people can easily access support without all the stumbling blocks and delays they often run into.” Employers who lead with empathy—and prioritize flexibility, compassion and connection alongside performance—help create cultures where people feel empowered to seek help when needed. “We have to ensure that we have accessible resources,” Dr. Breshears said. “People bring their personal struggles into the workplace, and take their struggles in the workplace home. The lines have certainly blurred.”Know when to seek help.
While self-care and support systems can go a long way, there are times when professional help is essential. Mental health conditions are common—and treatable. The sooner you seek help, the better. This is especially true for men, who often face cultural and emotional barriers when it comes to seeking support. “Men on average tend to delay help-seeking more than women,” Dr. Breshears said. “And this is especially true when men are suffering. Frankly, it's a mortality issue.” He noted that men are more likely to die by suicide and experience substance abuse disorders, which makes early intervention even more critical. Dr. Breshears also emphasized the need to remove barriers and promote action: “We have to create environments in which people feel safe to talk about the struggles that they’re having.” If you’re struggling, don’t wait. Explore Wellstar Behavioral Health services and find the support you need today. If you or someone you know is in crisis, call or text 988 for the Suicide and Crisis Lifeline, or contact the Crisis Text Line by texting TALK to 741741.;
Let’s cut to the chase: What is the best way to lose weight?
Dr. Rubin: There is no magic fix that works for everyone. Many people have tried every fad diet out there. They’ve tried being more active. Maybe they’ve even had bariatric surgery or used injectable weight loss drugs—but nothing works. If this sounds like you, schedule an appointment at a comprehensive weight loss center. Find one that offers medical and surgical treatment options and personalized recommendations. And make sure they provide ongoing support to help you meet and maintain your weight loss goals. Dr. Hilton: Both of our centers take this comprehensive approach. We use every tool available to treat obesity. You may be successful with lifestyle changes alone, or perhaps you need to meet with a behavioral therapist or consider surgery, medicine or a combination of therapies. Everyone is unique, and their treatment plan has to be unique too.What’s your take on weight loss injectables—are you a fan?
Dr. Rubin: I’m excited about drugs like Wegovy and Ozempic, which people sometimes refer to as GLP-1s. They work because they control your appetite and reduce ‘food noise,’ a persistent, unwanted focus on food. However, not everyone can tolerate the side effects, which include nausea, constipation and diarrhea. If you want to lose more than 20% of your body weight, using one of those drugs alone probably won’t get you there. Another consideration is that many people need to continue taking these drugs for life—even after they reach their weight loss goals.What are some misconceptions about bariatric surgery?
Dr. Hilton: Two big misconceptions are that bariatric surgery is dangerous and it doesn’t work. Here’s what I’d say: First, bariatric surgery is as safe as a routine procedure like gallbladder removal. Second, bariatric surgery is the most long-lasting and effective treatment for obesity available. Most people who have bariatric surgery maintain their weight loss at the 10-year mark.With weight loss drugs dominating the headlines, have you noticed a shift away from surgery?
Dr. Hilton: Yes, but I think that’s temporary. The drugs are sparking conversations about obesity and weight loss, which is a good thing. Patients who have never considered bringing up obesity to their primary care provider are asking about the injectables. They’re making appointments at a comprehensive weight loss center, and they are discovering they have a lot of choices. It isn’t ‘medicine or surgery’ or ‘medicine versus surgery.’ Sometimes the best answer is both.Can you share a weight loss success story with us?
Dr. Rubin: We’ve had so many success stories. One of our rock star patients has lost 250 pounds under our care. Now, she’s living her life again. Her diabetes is in remission, and her cholesterol has improved. She’s no longer depressed and isolated. My whole team is so proud of her—she has completely changed her lifestyle, sees our dietitian regularly and attends our support group. Another patient has lost 135 pounds. He and his wife are losing weight together, and it’s fantastic. Dr. Hilton: We ask our patients at their first visit, ‘What does success look like to you?’ Most have a number in mind, but non-scale victories are important too. Some want to get off their diabetes medicine or shop in a regular store instead of a big and tall store. Others want to take their kids to Disney World or a water park and have fun on the rides—not just watch.What is the No. 1 key to weight loss success?
Dr. Rubin: The key is to make lasting lifestyle changes. Medication and bariatric surgery can only get you so far. If you are ready to make these changes, consider finding a team who offers personalized, long-term support. Dr. Hilton, myself and others at Wellstar are here to help! Ready to take your first step? If you’re considering lifestyle changes, medication or surgery for weight loss, it all starts with a conversation. Schedule a visit with your primary care clinician to discuss your goals, health history and next steps.;
1. High blood pressure can be silent—and dangerous.
Some women develop high blood pressure during pregnancy, even if they’ve never had it before. High blood pressure can lead to preeclampsia. It’s a condition that can cause organ damage and, in severe cases, seizures. When high blood pressure isn’t treated, it can increase the risk of stroke or heart failure. Checking your blood pressure regularly can help catch problems early.What to do about high blood pressure
If you have a history of high blood pressure, heart disease or a family history of cardiovascular issues, tell your care team. Preconception counseling is essential if you have a known heart condition. Your physician may recommend that you monitor your blood pressure at home and report any sudden swelling, headaches or vision changes immediately.2. Heart failure can happen—even in healthy moms.
A rare but serious condition called peripartum cardiomyopathy (PPCM) weakens the heart, usually in the last month of pregnancy or the months following delivery. If you have shortness of breath, swelling or often feel extremely tired, don’t ignore those signs.What to do if you have shortness of breath or a racing heart
Talk to your provider immediately if everyday activities leave you exhausted or struggling to breathe. Other concerning symptoms include persistent coughing, swelling in your legs or feet and dizziness. Don’t ignore symptoms like chest pain, shortness of breath, severe fatigue or a racing heartbeat. These could signal a serious heart problem—seek help right away.3. Pre-existing heart conditions and hypertensive disorders require extra care.
If you’ve ever had heart disease, a heart defect or high blood pressure—including hypertension or hypertensive disorders—pregnancy can increase your risks. Even women without symptoms before pregnancy may need extra monitoring.What to do if you have a pre-existing heart condition
Talk with your provider early about a care plan. High-risk pregnancies may require specialist support, like a maternal-fetal medicine physician or cardiologist. If you’ve been diagnosed with a heart condition before pregnancy, ask your provider how it may affect labor and delivery. If something doesn’t feel right, speak up. You know your body best, and your concerns deserve attention.4. Blood clots are more common during pregnancy.
Pregnancy increases the risk of thromboembolism, a serious condition where blood clots can travel to the lungs and cause a pulmonary embolism. The risk is even higher for women with a history of clotting disorders, obesity or limited mobility.What to do to prevent blood clots
To reduce your risk of blood clots, stay active, stay hydrated and watch for warning signs like leg swelling, redness or pain. If you notice these, call your provider right away. If you’re on bed rest, ask your provider about ways to improve circulation. Learn the signs of deep vein thrombosis and pulmonary embolism.5. A racing heartbeat may be abnormal.
You can expect some changes in heart rhythm during pregnancy, but arrhythmias (irregular heartbeats) can be a sign of something more serious. Hormone changes, increased blood volume and underlying conditions like thyroid disorders can all contribute to an irregular heartbeat.What to do about a racing heart
If your heart races often, feels like it’s skipping beats or you feel dizzy or faint, let your provider know immediately. Keep track of when these symptoms happen and whether they occur at specific times, such as during physical activities or when your stress levels are high.6. Postpartum recovery still puts stress on the heart.
The risk of heart complications doesn’t end at delivery. Many serious conditions, including heart failure or high blood pressure, can develop in the weeks or months after childbirth. Postpartum heart issues can be life-threatening if you don’t address them.What to do during the postpartum period
Keep all postpartum checkups, even if you feel fine. Watch for new symptoms like chest pain, shortness of breath or extreme fatigue. If you had high blood pressure during pregnancy, continue monitoring it after delivery. Be aware that cardiovascular complications can develop up to a year postpartum, and follow-up care is so important for your long-term health.7. Your hospital choice matters
For women at high risk, delivering in a hospital with access to specialized prenatal tests, genetic testing like amniocentesis, fetal evaluations and emergency cardiac care can make all the difference. Not all hospitals have the same level of maternal heart care, so it’s important to plan ahead. Choose a hospital that is equipped to handle pregnancy-related cardiac emergencies. Wellstar provides specialized care for mothers and babies close to home, including:- Wellstar Acworth Health Park: Perinatal cardiology
- Wellstar Avalon Health Park: Perinatal cardiology
- Wellstar Cherokee Health Park: Perinatal cardiology
- Wellstar Children’s Hospital of Georgia: Level IV NICU
- Wellstar Cobb Medical Center: Emergency cardiac care, level III NICU, maternal-fetal medicine, medical genetics, perinatal cardiology
- Wellstar Douglas Medical Center: Emergency cardiac care, maternal-fetal medicine
- Wellstar East Cobb Health Park: Perinatal cardiology
- Wellstar Kennestone Regional Medical Center: Emergency cardiac care, Level III NICU, maternal-fetal medicine, medical genetics, perinatal cardiology
- Wellstar MCG Health Medical Center: Cardio-obstetrics, emergency cardiac care, maternal-fetal medicine, medical genetics
- Wellstar North Fulton Medical Center: Emergency cardiac care, medical genetics
- Wellstar Paulding Medical Center: Emergency cardiac care, medical genetics, perinatal cardiology
- Wellstar Spalding Medical Center: Maternal-fetal medicine
- Wellstar Vinings Health Park: Perinatal cardiology
- Wellstar West Georgia Medical Center: Emergency cardiac care
What to do about your hospital choice
If you are high-risk, consider hospitals with advanced cardiac care and those that have expertise in pregnancy-related heart conditions. Talk to your care team well in advance about your birth plan, especially if you have a heart condition. If possible, tour the hospital beforehand and ask about its capabilities in managing pregnancy-related heart complications.8. Mental health and stress impact heart health.
Anxiety and stress can affect your heart. If you’re feeling overwhelmed, talk to someone. Your mental health is just as important as your physical health. Depression, anxiety and even post-traumatic stress disorder are common in pregnancy and postpartum, and they can impact heart health.What to do to keep your mental health in check
Access mental health resources and practice stress management techniques to help you manage your mental health. Simple practices like deep breathing, mindfulness and connecting with loved ones can help lower stress levels. Remember, you are empowered to take control of your health—talk with your provider or a support person and get the help you need.Take Action for a Healthier Pregnancy.
Eat well, stay active and avoid smoking or alcohol. These efforts can protect your heart and your baby’s health. Small, consistent changes—like reducing salt intake or walking daily—can make a difference. Regular prenatal visits are just as important. Remember, knowledge is power. Stay informed, speak up when something feels off and choose a hospital that meets your needs. These simple steps can help you take control of your heart health and reduce the risk for you and your baby. Find an OB/GYN or perinatal cardiologist and learn about labor and delivery at Wellstar.;
According to the Centers for Disease Control and Prevention (CDC), about 1 in 10 Americans have diabetes. Of that group, 90 to 95% have type 2 diabetes. Because this condition often develops in people over 45, getting screened and getting the best treatment to live your healthiest life is essential.
"Diabetes is a chronic and complex condition, and treatments are continuously changing," said Dr. Georgia Forrest, Wellstar primary care physician. "Teaming up with a primary care provider who personalizes your care plan to you and everything that makes you unique should be a top priority."
Whether you currently have type 2 diabetes, a family history of the disease or feel concerned about your overall well-being, you can take proactive steps to manage your health. Here are some key facts to help you better understand the relationship between diabetes and good health.
1. Undiagnosed diabetes costs you money & health
Not knowing you have diabetes carries high medical costs. Undiagnosed diabetes can increase your risk for death and other medical issues.
Diabetes was the eighth leading cause of death in 2021, the most recent data reported by the U.S. Preventive Services Task Force. And according to the American Diabetes Association, having diabetes doubles your risk for heart disease and stroke—heart disease is the number one killer in the U.S.
2. A diagnosis and personalized treatment can save your life
Knowing you have diabetes and then working to manage your blood sugar, blood pressure and cholesterol effectively can lower your risk of death and help you live a better quality of life.
3. Getting screened for diabetes is easy
The U.S. Preventive Services Task Force now recommends getting screened with a simple blood test at the age of 35 for people with no symptoms but who are overweight or obese. Even if you have no signs or family history of diabetes, it can lurk in your numbers. Getting screened can help you catch it early and even prevent it altogether.
Consider getting screened for diabetes if you:
- Are obese or overweight
- Are physically inactive
- Have a parent or full sibling with diabetes
- Are an African American, Latino, Native American, Asian American or Pacific Islander
- Have a history of cardiovascular disease
- Have hypertension
- Have blood work that shows an HDL of less than 35 mg/dl or triglycerides greater than 250 mg/dl
- Have a diagnosis of polycystic ovarian syndrome
- Have other medical conditions that lead to insulin resistance
4. Some people have pre-diabetes
If your screening shows that you have pre-diabetes, your blood sugar levels run higher than average but aren't within the range of type 2 diabetes. However, you have an increased risk of getting type 2 diabetes.
Identifying that diabetes is around the corner can help you stop it before it starts.
5. Diabetes treatment plans should be unique
When crafting a plan to address diabetes, the conversation must be about more than the numbers.
"Additional diseases or conditions you may be experiencing in conjunction with your diabetes should also become part of your individualized health plan," Dr. Forrest said.
A complete medical history helps your healthcare provider understand how other medications and treatments may interact with your symptoms and treatments related to type 2 diabetes.
6. Lifestyle modifications can make a big impact on diabetes
Lifestyle modifications may involve slight changes to your weight, the amount of exercise you get, your diet and even your sleeping patterns.
Changes don't have to be major. For instance, your doctor may suggest you lose around 10 pounds and exercise for 30 minutes five days a week.
Our primary care providers work with patients one-on-one but can also refer patients with pre-diabetes and diabetes to Wellstar Diabetes Services to help prevent the onset or manage the effects of diabetes.
7. S.M.A.R.T. diabetes treatment plans
According to Dr. Forrest, your overall plan should include "specific, measurable, achievable, relevant and timely (S.M.A.R.T.) goals and involve shared decision-making between you and your care provider. There should be plenty of follow-ups to keep the conversation fluid and open to modification."
8. Know your numbers — and acronyms (A1C, CGM, TIR)
Should your screening lead to a type 2 diabetes diagnosis, conversations with your health providers will focus on several acronyms and numbers.
"Know your ABCD’s of diabetes," said Dr. Forrest. "Your A1C, blood pressure, cholesterol and the medications you are taking. Knowing these facts about your health will be key to your success."
• A = Hemoglobin A1C goal is <7
• B = Blood pressure goal is <130/80
• C = Cholesterol goal is to keep bad cholesterol <100
• D = Drugs
Keeping the A1C low and within an optimal range will help prevent complications like eye damage, blindness, kidney failure and nerve damage.
A mainstay for type 2 diabetes management centers around constant glucose level monitoring. Continuous glucose monitoring (CGM) provides readings every few minutes via a sensor inserted just below your skin. Monitoring glucose is a common way to help regulate insulin in your body, giving you the readings you need to self-adjust with insulin when appropriate. Average glucose levels should be 100 mg/dl or lower though they can increase if you've just eaten.
New developments introduced the importance of tracking Time in Range (TIR). Along with monitoring your glucose levels, TIR may impact your customized plan for maintenance. According to Dr. Forrest, the goal for TIR is 70% or more.
9. Receive individualized diabetes care at Wellstar
For diabetes management, a personalized, proactive approach can make all the difference. Wellstar primary care providers are here to partner with you to help prevent or manage diabetes, heart disease and many other conditions.
"A true patient-centered approach for managing diabetes is the key to the future of this disease," Dr. Forrest said. "Get screened and speak up when it comes to your care. Opportunities for personalized and individualized medicine should be a part of your treatment plan as you move forward."
Find a primary care provider near you.

Over the years, advice about breast self-exams and breast cancer screenings has changed. So what exactly should you be doing to make sure you’re staying your healthiest? We brought together a panel of women’s health experts to discuss the best strategies to keep tabs on your breast health—and who to talk to if you’re diagnosed with breast cancer.
I do breast self-checks every month. Why do I need a mammogram too?
Dr. Paula Greaves, MD, OBGYN, Wellstar chief Women's Health officer: Unfortunately, 1 in 8 women will develop breast cancer in their lifetime, so early detection is key. We have shown over the years that the sooner we detect breast cancer, the more successfully it can be treated. Survival has increased significantly since we started finding breast cancer earlier—before there are symptoms, such as feeling a lump during a self-exam.
Mammograms are essential for early detection. It’s recommended that women start getting mammograms at age 40. However, if you have a family history of breast cancer or other risk factors, your gynecologist or primary care provider may recommend starting earlier and will help you create a personalized screening plan. There are some risk factors that women cannot change, such as genetics, but there are some ways women can lower their risk, like quitting smoking, eating a healthy diet and exercising regularly. Wellstar offers 16 mammography locations, and our patients have state-of-the-art technology on their side. We offer high-resolution breast screening, including 3D mammograms.
Women should continue not only getting annual mammograms, but also seeing their gynecologist or primary care provider for regular breast exams. Women should also be aware of physical changes within their bodies, including breast changes. Changes in the texture of the skin or a lump or pain in the breast should always be checked out by their healthcare provider.
Margie Apacible-Mancao, MSN, RN, CBCN, nurse navigator: I am so passionate about breast cancer screening—every opportunity I have I tell patients to get a screening mammogram when they’re of age. Tell someone in your circle that you’re going, then they’ll tell someone in their circle and the circle gets wider so more people will get screened.
Does it mean I have cancer if the doctor recommends a biopsy?
Dr. Sujatha Hariharan, MD, medical oncologist: When a mammogram detects an abnormality, a biopsy might be indicated. Many breast biopsies will be non-cancerous such as fibroadenomas.
If cancer is found on a breast biopsy, there are several parts of the pathology result that the care team will utilize to make a treatment plan. For example, the presence of estrogen and progesterone receptor positivity allows the potential for hormone therapy as part of the treatment plan. The HER-2 gene is also tested for and if that is present and positive, it allows for medication directed at the HER-2 gene to be given along with chemotherapy.
Sequencing of the various treatments for breast cancer—surgery, chemotherapy, radiation and hormone therapy—will be determined as a collaborative effort between the breast surgeon and medical oncologist.
If I’m diagnosed, who should I talk to next?
Margie: The anxiety of not knowing their diagnosis or what’s next is one of the hardest parts. At Wellstar, patients have access to a nurse navigator on the day they are recommended to have a biopsy. We make an appointment with the specialists as quickly as possible because just knowing that someone is helping them get to the next step and get that appointment fast dials down their stress level.
Dr. Karen Xu, MD, radiation oncologist: If you are diagnosed with breast cancer, you will need to see a breast surgeon first to discuss your surgery options—lumpectomy or mastectomy; a radiation oncologist to discuss the duration of radiation treatment and whether lymph nodes should be included in the target; and a medical oncologist about whether endocrine therapy or chemotherapy is indicated and the timing of systemic therapy. Patients who desire reconstruction after mastectomy will discuss with a plastic surgeon the type and timing of reconstruction they want.
Schedule a mammogram
Find a breast imaging location near you online or call (678) 581-5900.

Heart attack is the leading cause of death in Georgia, according to the American Heart Association. To save more lives, Wellstar provides advanced heart care services, ranging from minimally invasive procedures to open heart surgery. The health system recently expanded its offerings to bring an advanced technology called rotational atherectomy to more people in our community. The tool our physicians use for this procedure is called a Rotablator, which has a small but mighty diamond tip.
Who rotational atherectomy helps
Wellstar has offered percutaneous coronary intervention (PCI), formerly known as angioplasty, for a number of years. This procedure helps treat the main cause of heart attacks—the build-up of cholesterol filled plaque within a coronary artery. The build-up decreases blood flow and oxygen to the heart. By opening the artery, blood and oxygen can move freely once again.
The benefits of having a PCI typically include fewer complications, faster recovery time and shorter hospital stays.
Not everyone is a candidate for PCI, especially when the blockage is heavily calcified. But rotational atherectomy changes that.
“For heavily calcified coronary blockages, rotational atherectomy works as a drill to decrease the bulk of calcium,” said Wellstar interventional cardiologist Dr. Omer Mirza.
This technology makes non-surgical heart attack treatment available to people with more complex blockages that could not typically be cleared with balloon angioplasty.
Rotational atherectomy has been available at Wellstar Kennestone Regional Medical Center, and now we have expanded availability recently to Wellstar Cobb Medical Center.
“By expanding Wellstar Cobb’s technology, we can offer more comprehensive care for the patient and prevent transfers and subsequent delays to patient care,” Dr. Mirza said.
How rotational atherectomy works
At Wellstar, a rotational atherectomy is performed using a Rotablator, a small, diamond-tipped tool. This revolving instrument is inserted into the blocked artery using a catheter while a patient is under local anesthesia.
When the interventional cardiologist guides the Rotablator to the blockage, it begins to rotate, going as fast as 190,000 rpm. It gently breaks apart the blockage, making the plaque particles small enough to pass safely through the bloodstream.
Stents are then placed in the artery to widen it so blood can flow through. This procedure can improve blood flow and heart function within minutes.
Effective treatment with advanced technology
Studies indicate that rotational atherectomy results in high procedural success rates.
Giving patients the ability to resume normal activities within a few days, the recovery time for this procedure is significantly less than open heart surgery. Patients undergoing a rotational atherectomy typically spend one night in the hospital.
Learn more about interventional cardiology at Wellstar or find a specialist near you.

It all started with a gift and a special note.
April Sather had just undergone surgery for her breast cancer and was struggling to sleep at night. She would spend the night tossing and turning, trying to get comfortable. “I’m a side sleeper, so that is kind of an issue,” she said when describing her sleeping troubles.
One day she received a gift from a friend: a heart-shaped pillow made with soft flannel that was light pink with beautiful clouds across it. Sather was able to tuck it under her arm and sleep comfortably throughout the night. This gift, combined with a lovely note from one of her nurses after surgery, inspired Sather to want to do the same for others.
“I thought, ‘Wouldn’t it be cool if we could make heart-shaped pillows for other breast cancer patients so that after they get out of surgery, they could feel that same love that I received?’” Sather said. “I shared the idea with a few ladies at church, and the rest is history.”
Healing Hearts Ministry at Warren Belvedere Church now meets once a month to sew, stuff, pray, write notes and package up the hearts to be delivered to patients with breast cancer across the CSRA. There is no commitment, and volunteers are welcome to take the materials with them if they prefer to work in the comfort of their own homes.
“It makes me feel like I’ve done something that’s worthy of helping someone else go through a hard time in their life,” volunteer Susan Elliot shared about each time the group finishes a pillow to be delivered to a patient.
Elliot is one of the women who answered Sather’s call for help with her idea. While she has no personal experience with breast cancer, she is a seamstress and was more than happy to use her knowledge and experience with sewing for the program.
Healing Hearts provides the sewing pattern, fabric and fluff needed to create the pillows, so all that volunteers have to bring are their hands and good spirits. Sometimes the group welcomes speakers during the meetings; in fact, they celebrated their first anniversary by inviting a Wellstar Georgia Cancer Center patient and breast team nurse navigator to come and share their story.
If you would like more information or to make a donation to assist the program, visit the church’s website, select the Belvedere campus, then make the message out to April Sather or Susan Elliot. You can also get in touch through the church’s Facebook page.
;


Dr. Joanna Dolgoff, Wellstar Children’s of Georgia pediatrician and author of the bestselling book “Red Light, Green Light, Eat Right,” uses her “no time, some time, never all the time” philosophy to provide families with guidance around screen time. At nearly every wellness visit, Dr. Dolgoff talks with parents about how to set healthy limits with screen time. “We’re seeing language delays in children from too much screen time,” she explained. Some signs that children may be spending too much time on social media, gaming or watching videos can include:
- Aggression
- Difficulty handling boredom without a screen
- Trouble connecting with peers
- Sleep disruption
- Poor focus in school
- Withdrawing from hobbies or activities they once enjoyed
Troubling trends in children’s media habits
Common Sense Media is a nonprofit organization that advocates for children’s health in the digital age. Its most recent survey of the digital habits of children 8 and younger showed that by age 2, 40% of children have their own tablet. By age 4, that number climbs to 58%. The survey also found that 1 in 5 children use mobile devices during meals, at bedtime or to cope with emotions. Dr. Dolgoff stresses that parents must monitor and regulate their children’s digital use across all platforms. Yet the same survey shows gaps in how families co-view content: 62% of parents occasionally watched YouTube with their children, compared to only 17% on TikTok. The survey also found that screen use varies by income. Children in lower-income households spend twice as much time on screens (3 hours, 48 minutes) as those in higher-income households (1 hour, 52 minutes).Guidelines for screen time by age
As a spokesperson for the American Academy of Pediatrics, Dr. Dolgoff suggests that parents know and follow the organization’s screen time guidelines for children:- Under 18 months: No screen time
- 18 to 24 months: Only educational content with parents
- 2 to 5 years: No more than one hour per day
- 6 years and older: Balanced screen time that doesn’t interfere with family, friends and schoolwork
What do screen time limits look like?
According to Dr. Dolgoff, parents don’t need to worry if little ones under 18 months use screens for video chats with loved ones like grandparents. But she adds an important distinction: “Content matters. Mindlessly scrolling through TikTok videos is not what we want children doing for hours each day.” Fortunately, children’s programming has expanded considerably since the parents of today were kids. YouTube Kids, PBS Kids, Netflix, Apple TV and other streaming services serve a variety of programs. Here are some healthy screen time choices, along with suggested time limits:- Toddler (2 to 3 years): Video call with grandparents and 30 minutes of educational programming such as Daniel Tiger’s Neighborhood or Sesame Street with parents watching
- Elementary school (6 to 10 years): Homework on Chromebook or other platform and 30 minutes of YouTube Kids, unstructured outside play and bedtime stories
- Teens (13 years and older): Homework time and no more than two hours of other screen use for gaming or socializing with friends
- “What do you think will happen next?”
- “How would you feel if that happened to you?”
- “Could this happen in real life?”
- “How would you have made this better?”
Sound screen habits begin with parents
Young children develop social and communication skills by observing, listening, talking (babbling counts!), reading, singing and playing with parents, siblings and others. The American Academy of Pediatrics advocates that parents put down their phones so they can focus on those activities and interactions. For help, parents can turn to apps designed to monitor their smartphone and tablet use. They can also examine their habits by asking themselves questions such as:- “Am I scrolling at the dinner table?”
- “Am I texting while driving?”
- “How much are my children watching me use my phone for entertainment?”
- “Am I setting a good example by having hobbies and interests that don’t involve screens?”
Experts advise ways to set and enforce limits
The American Academy of Child & Adolescent Psychiatry and the American Academy of Pediatrics understand the temptations of screens and parents’ difficulty setting limits. Some of their advice for parents:- Avoid using screens as pacifiers, babysitters or to stop tantrums.
- Create tech-free times, with extended breaks and tech-free zones, including the meal table.
- Learn about and use parental controls on devices, including phones, tablets, laptops and televisions.
- Make family outings technology-free—and that includes cameras.
- Remove screens from bedrooms 30 minutes to an hour before bedtime.
- Set a timer when using a device as a reminder to turn it off or put it away.
Tips for enforcing screen-time limits
It’s in children’s nature to resist when they don’t want to stop doing something pleasant or fun. It’s the parents’ job to stick to the limits they’ve set. Some more ideas for managing children’s reactions to screen-time limits include:- Have a designated “quiet spot” for younger children to calm down if they rage after time on a device is up.
- Offer alternatives after a device is turned off. Those could include playing a board game, reading a book together, playing with a favorite toy or creating an art project.
- Warn children before their time limit is up.
Resources for parents
- The American Academy of Child & Adolescent Psychiatry on screen time limits, music and music videos, video games, movie and video choice, and screen violence
- Common Sense Media
- Google and Apple content about online safety and parental controls
- Healthychildren.org, a website of the American Academy of Pediatrics
- know2protect, guidelines for protecting children online from the U.S. Department of Homeland Security

If you’ve had a stroke, you don’t have to replace flavorful cuisine with bland foods on your journey to recovery.
There are easy, delicious meal options that follow American Heart Association nutrition guidelines for lowering your risk of another stroke. More fiber, whole grains, fruit, vegetables and lean protein, with less trans fat, saturated fat, sodium and sugar are key to supporting your recovery efforts. Rehabilitation care teams and dietitians at Wellstar recommend keeping meals and snacks interesting with variety and new recipes like these.
Coconut Truffles satisfy your sweet tooth without any added sugar.
Ingredients:
12 medjool dates, pitted
2 tablespoons water
4 tablespoons unsweetened cocoa powder
½ cup puffed brown rice
½ cup shredded unsweetened dried coconut
Directions:
- Using a blender or food processor, puree dates and water until a sticky paste forms.
- Add cocoa powder and pulse until a solid dough forms.
- Stir in puffed brown rice.
- Using a small scoop, form mixture into 14 tablespoon size balls.
- Roll each ball in the shredded coconut for a light coating.
- Refrigerate for one hour.
- Enjoy!
Southwestern-Style Breakfast Casserole is a great way to start your morning.
Ingredients:
6 slices hearty whole-grain bread, cut into cubes
1 10-ounce package frozen chopped spinach, thawed and liquid squeezed out
1 7-ounce jar roasted red peppers, drained and chopped (or 1 red bell pepper, roasted and chopped)
1 ½ cups (6 ounces) Mexican-style cheese
3 cups non-fat milk
8 ounces egg substitute
1 teaspoon garlic powder
1 teaspoon cumin
½ teaspoon black pepper
½ teaspoon salt
Directions:
- Coat a 9 x 13 inch baking dish with non-stick cooking spray.
- Layer the bread in the bottom of the baking dish.
- Sprinkle evenly with the spinach, red peppers and cheese into baking dish.
- Combine the non-fat milk, egg substitute, garlic powder, cumin, black pepper and salt, then pour into baking dish.
- Cover and refrigerate at least four hours or overnight.
- Preheat oven to 350 degrees F.
- Bake, uncovered, for 45 minutes or until a knife inserted into the center comes out clean.
- Let stand 10 minutes before serving.
For more heart-healthy recipes, visit American Heart Association Recipes.
To learn more about how you can partner with Wellstar rehabilitation care teams to reduce your risk of another stroke, visit https://www.wellstar.org/medical-services/treatments-procedures/rehabilitation-services/neuro-rehabilitation..
;
Augusta University Health System (AUHS) has signed a letter of intent with Wellstar Health System to form an innovative new partnership that would expand Augusta University’s educational and research missions and allow Wellstar Health System to create a broader affiliation with the university’s Medical College of Georgia (MCG) as AUHS joins the Wellstar Health System.
The potential partnership is the culmination of a thoughtful and deliberate process begun in 2019 by AUHS, its governing board and Augusta University to strategically grow MCG while expanding and improving both patient care and Georgians’ access to health care services across the state.
The proposed partnership would innovate clinical care, training and research while adopting a successful model of bringing together community-based health systems and academic medical centers such as MCG and its teaching hospitals. MCG and Augusta University are part of the University System of Georgia (USG), and MCG serves as the only public medical school in the state.
“AUHS, Augusta University and the Wellstar Health System have a shared mission to solve Georgia’s health care challenges,” USG Chancellor Sonny Perdue said. “By joining forces and working together, we can leverage Wellstar’s clinical platform and leading-edge systems to support patients while providing more opportunities for students to learn, train and care for residents in local communities across Georgia.”
Pending a definitive agreement and regulatory approval, the partnership would focus on three strategic initiatives:
- Expanding digital health offerings to create more convenient access to care and provide more individualized care regardless of location.
- Growing the pipeline of physicians and other health care providers serving Georgia by increasing the number of students who train and conduct research through MCG.
- Developing new treatments, innovative care offerings and scalable care models to optimize the health and well-being of every patient.
“By bringing Augusta University Health System together with Wellstar Health System and leveraging our respective strengths, we would improve the health of the community, address social determinants of health and expand access to quality care for all Georgians,” said Candice L. Saunders, FACHE, president and chief executive officer of Wellstar Health System.
While there are aspects of the proposed partnership yet to be determined, the partnership would likely result in significant investments to improve existing healthcare facilities and to expand access to care across the state, including a new hospital and medical office buildings in Columbia County.
“Providing health care has never been as dynamic and complex as it is today, and this partnership with the Georgia-based, not-for-profit Wellstar Health System would enable us to extend our mission of improving health through excellence in patient care, education and research for the benefit of Georgians,” said Brooks A. Keel, PhD, acting chief executive officer of Augusta University Health System and president of Augusta University.
Through an expanded affiliation with the university’s Medical College of Georgia, the partnership would address the need to train more physicians and address a growing statewide shortage. With 60 percent of MCG graduates entering a primary care residency, training more physicians in these disciplines would support increased access to frontline care provided by specialists such as family medicine physicians and general pediatricians, especially in underserved areas of the state.
A new teaching campus in Atlanta at Wellstar Kennestone Hospital could also be established under the proposed partnership. As a result, MCG, which already has the ninth-largest freshman medical school class in the nation, would grow to become one of the largest public medical schools in the country.
“With our entire nation facing a physician shortage and our state typically ranking about 40th in the number of physicians per capita, educating the next generation of physicians is more critical than ever,” said David Hess, MD, dean of the Medical College of Georgia and executive vice president of medical affairs and integration at Augusta University. “I’m excited about the partnership with Wellstar, since it will enable our students and residents to continue to learn from some of the most highly qualified physicians and other health care professionals in the state while allowing MCG to expand its contributions to improving public health in Georgia especially in more rural regions.”

This article was originally published on Atlanta Business Chronicle on August 19, 2022.
Cancer is the second-leading cause of death in the United States, with more than 600,000 people dying of cancer in the country in 2021. While the U.S. death rate, or the percentage of people dying from cancer, is decreasing — partly due to fewer people smoking — the number of cancer deaths is going up due to our aging population. All these statistics are behind the call to decrease cancer deaths by 50% in the next 25 years. Atlanta Business Chronicle recently talked with a panel of experts from Wellstar Health System and the American Cancer Society, headquartered in Atlanta, about ways to accelerate cancer care progress through scientific research, patient care, partnerships, early detection, diversity and inclusion, and local care.* (Remarks edited for clarity and brevity.)
Panelists & moderator
Moderated by David Rubinger, market president and publisher, Atlanta Business Chronicle.
*Wellstar partners with Northwest Georgia Oncology Centers to provide world class cancer care close to home.
Research & treatment
David Rubinger: Where are we today in the world of scientific research? Are we in a good place in terms of research dollars?
Kimberly Jackson: I think we’re in a good place, but we can always be doing better and that’s a fact. There’s no other nongovernmental, nonprofit organization in the United States that’s focused on finding the cause and cures for cancer like the American Cancer Society. We’re committed to continuously funding the best new and ongoing projects at institutions across the country. For instance, right now in Georgia, we are currently funding eight research multi-year grants that are totaling more than $6.3 million. In addition to funding and conducting research, we are mobilizing our grassroot network advocates to increase the funding for cancer research. We’re primarily supporting those investigators that are early in their career, who are doing the most innovative cancer discovery research.
Rubinger: While the aging population is causing the cancer deaths to increase, the average death rate for the population has actually decreased. What do you attribute recent successes to and how will we continue to fight cancer deaths in the future?
Dr. Steve McCune: The mission of the Wellstar and Northwest Georgia Oncology Centers partnership is to help cancer patients live longer by providing innovative therapies in their local communities. What we have seen in the last 10 years has revolutionized the treatment of certain cancers, particularly lung cancer and melanoma, with immunotherapy and targeted therapies, oral drugs that address a gene mutation. What may be a good way to think of that is it’s the Achilles heel for certain cancers: they have one gene that drives their growth. And there are, because of the research that has occurred, typically one or more drugs that may specifically treat that mutation and block it so that it no longer encourages the growth of cancer cells.
Next-generation sequencing makes it very easy and fast to sequence 400 to 500 genes in a tumor from an individual patient, so that you know exactly any gene mutations in that particular tumor. It’s the most individualized medicine you could have. That’s the reality and that’s very accessible for many patients.
Rubinger: Nicole, from the nursing standpoint on the front line with patients, how has immunotherapy changed the relationship between the patient and the healthcare provider psychologically?
Nicole Centers: From the patient care perspective, it’s very clear that patients are more involved in their care. They want to have more say in their care. When we can educate patients appropriately up front about all of their different options and their care along with their providers, they feel like they have more control. We know when patients feel more in control of their care, they’re more compliant to the plan of care. When it comes to immunotherapy and monoclonal antibodies that are given, they’re generally tolerated far better than chemotherapies of the past. That doesn’t mean everything can be treated with an immunotherapy or monoclonal antibody. However, when we have more options to give patients that they can tolerate better, then it kind of alleviates all of those nightmares of, “This is a horrific journey,” and, “It’s not going to work for me.” Overall, we have medicines that work with your body to fight the cancer in ways that we just haven’t had before.
Patient care & partnerships
Rubinger: The cancer “moonshot" is a term that excited everyone. Have you seen the concept of patient care change from when you first got into the field to where it is today?
McCune: I think it’s dramatically different. In some ways the moon shot has already happened and I'll explain what I mean by that.
Immunotherapy revolutionized the treatment of cancer. If you have a chemotherapy that kills 99% of cancer cells, well that means eventually that 1% keeps coming back. Immunotherapy can work for years, even after the actual immunotherapy has stopped. It’s not a vaccine, but it works in much the same way that a person’s own immune system actually can control or eliminate the cancer. I think that, in a sense, was the biggest game changer for the way that people were treated.
I started doing this about 20 years ago. And so most things that we treated were chemotherapy, very few things that were actually what we would have called targeted therapy or intelligently designed targeted therapy. The first drug was really coming out at that time called Gleevec, which treated CML (chronic myeloid leukemia.) I treated patients before that era who had to have a bone marrow transplant or they were basically going to die of CML. And now we think of CML as a condition that’s almost 100% survivable. We have eight different medicines that are commercially available for treating CML. It’s totally changed the future for some patients who would have had very poor outcomes otherwise.
Melanoma used to be very difficult to treat. Chemotherapy didn't work well. A treatment called Interleukin-2 worked for about 8% of patients and no one really knew why. It basically is an early immunotherapy but with a lot of toxicity. Now you have drugs like Opdivo, Yervoy, Keytruda, which are really the standard of care. Chemotherapy is rarely, if ever, used for melanoma.
There are antibody drug conjugates — something that basically has a payload on the monoclonal antibody, so it homes in on certain proteins on the outside of different cancer cells. That’s a way of delivering a toxin directly to the cancer cells with less impact on normal tissues.
There are companies all over the United States, from large to small, that are really driving the innovation in targeted therapies, antibody drug conjugates, so it’s an exciting time in oncology.
Wellstar has participated in trials for 15 years. In just the last three years, we have participated in cancer trials resulting in over 20 FDA approvals for either new medicines or new combinations of medicines. Usually, it is four to five years before something is FDA-approved. Now not everything’s approved, not everything works better, but it gives people hope and it gives them the chance to have cutting-edge therapies in their local communities.
Rubinger: Nicole, how have advances like these changed the psychology of talking with a patient with a cancer diagnosis?
Centers: I think it has changed. When I started in this field 20 years ago, we would say “the breast cancer down the hall" or “this is the breast cancer treatment.” Now we say, “the patient with breast cancer,” “the patient with lung cancer,” and we treat it as an illness that is part of the whole person, versus the whole person being the illness. That’s a different way that we think about things and that’s how we approach our patients differently when it comes to nursing.
There’s a very unique field inside of nursing called navigation. And one of the things that moonshot really promoted was something that we've been out here doing for a pretty good while, but it brought it to the center stage for all Americans to hear this word called a navigator. It meant someone that was going to guide you on your cancer journey. Several years ago, there was just one kind of navigator and they tried to do the whole care path, but we at Wellstar recognize that there’s lots of pieces to people who could have cancer, people who are being tested for cancer, and those patients that actually have cancer. So we have screening navigators, we have diagnostic navigators, and we have actual care trajectory navigators, which are oncology nurse navigators. We have over 15 of those in our system and some of those specialize by tumor type and some of those are more generalized.
What they do is they actually bring the whole person into view during their care. It means if you have childcare or if you have your parents, that you're taking care of first, or that transportation is an issue, these navigators work with you and your provider as well as your payers, whether it’s insurance or if you don't have insurance, we try and get you on insurance — to be sure that those things that would affect your compliance to the plan of care, they're helping you resolve.
It’s great if you can come in for your treatment. But if your dog has to be walked at two o'clock every single day and your treatment starts at noon, then we need to help you get a dog walker. We need to help you link to resources. For years there have been resources out there that patients didn't even know to utilize. And so organizations have this money that’s sitting there trying to help patients, but no one to link them to it. Navigators link patients to community resources, to national resources. The American Cancer Society has this really great program that will offer patients free rides to go get their cancer care, and most patients don't even know about that. But you talk to the navigator and they're like, “Wait, I have them on speed dial” because they get to know what those resources are, and they can help patients keep their appointments and keep a total life balance.
When we look at that, what that does is it makes their care more effective because they're more compliant to the plan of care.
The other thing navigators do is to help timeliness of care. So if two providers talk and say “we're both going to go see Sally Sue,” or whoever your patient is, and they turn to the front desk and say, “be sure we get this patient on the schedule.” However, the front office staff may not be aware the appointment doesn't meet the latest benchmark for timely care. So what a nurse navigator does is say, “Wait, we have some timeliness to care parameters that we know are best practice.” And they work with that provider or that office to help expedite those appointments.
The best part of navigation is it really brought care back into the patient’s community. Patients didn't understand what was available to them in their community. They thought you had to go to an academic center in a large city that cost them lots of money because they had to stay in hotels or take a flight or go get a car, because there’s so many patients in the states that don't have valid transportation that can take them two hours away. Navigators help patients understand what’s available in their community and the care that they can receive. They can also link them to clinical trials, arrange for assisted lodging and help patients get the best care out there to survive their cancer.
We've also seen an uptick in clinical trials because the navigators say, “Do you remember when your doctor talked to you about clinical trials? Do we want to circle back on that? And do you want to go talk to your doctor again?" They're reinforcing that education.
Second opinions & local care
Rubinger: Let’s move to another topic: the second opinion. The second opinion might be local, but if you have the resources, it might be at Sloan Kettering, MD Anderson or Mayo. Is there less of that going on today because local providers are able to provide that level of confidence in what the care is going to be? Twenty years ago you would have maybe run to Houston.
McCune: I think people still do, but maybe for a different reason. I think they have more information and more knowledge and they're not just running to Houston, they're running to a specialist in Houston or New York or Atlanta. I say, “Hey, you're not stepping on my toes. I want you to get a second opinion. I can help you get that, more than just a cold phone call. Let me try to get you to the right person.”
At Wellstar, we do have Mayo Clinic Care Network e-consults available. That’s a pretty easy way to get a quick question answered if we need a specific answer or a second opinion without someone having to travel somewhere.
In addition to second opinions, we believe in collaborative care. We have groups of cancer experts who diagnose and plan treatments together in tumor boards so patients have the best outcomes. In Specialty Teams & Treatments (STAT) Clinics, multiple cancer specialists meet with the patients and their families in one place on one day to help them get questions answered. This helps them start treatment faster so they have better outcomes.
Centers: At Wellstar, 300 cancer specialists in our network can collaborate with each other. When they do request second opinion e-consults from the Mayo Clinic, it is free to patients which is a really nice thing because they usually have to pay for second opinions.
Rubinger: Kimberly, when I think of the Cancer Society, I think of the research dollars going to help cure cancer. But as we were talking earlier about how it helps with driving patients to treatment, the society’s partnerships with a Wellstar or other healthcare systems may be less well known. Can you address that?
Jackson: Collaboration is absolutely critical. So many cancer patients and their families are facing barriers and challenges that are too complex for just one organization to address on its own. To help overcome those barriers, we unite organizations in partnership to improve the lives of people facing cancer.
One example, we have Hope Lodges all over the country where individuals and a family member are able to stay for free and they're wonderful. It’s a great resource for our patients and their families.
Another example is we partner with Wellstar and other health systems in Georgia to provide those transportation grants that Nicole talked about and service to people who need it the most.
For some people with cancer, transportation is a challenge and it creates that barrier to receiving the treatment that they need. Many of them need daily or weekly treatment and often over the course of several months and the need was particularly pronounced during the pandemic. We were able to provide funding to 251 health systems across the country to alleviate that financial burden of transportation.
Another way we mobilize the cancer community on both the national and the local level is through our mission-critical roundtables. We're providing organizational leadership and expert support to multi-organizational roundtables focused on breast, cervical, colorectal and lung cancer, HPV vaccination and patient navigation. Each roundtable has a shared vision to support people to prevent and support and survive cancer. It’s a proven model close to home. Wellstar Health System was a key partner in launching our Georgia Lung Cancer Roundtable, whose primary goal is to improve screening rates and lung cancer outcomes.
Rubinger: Our society has come a long way in terms of reducing smoking. What are the trends in lung cancer that you're seeing? Does it primarily impact your older patients or is it across the age spectrum?
McCune: It can be any age and certainly there are people who are non-smokers who are much more likely to have a lung cancer that is driven by a single gene mutation and those are usually treatable with targeted therapy, which is typically an oral drug. So, in one sense, lung cancer is a disease of people who have smoked for a long time, 30 or 40 years. But it’s also a disease of nonsmokers. I do think people are generally smoking less. I remember people used to smoke in the pediatrician’s office when I was little. Things have changed dramatically.
There is a very active lung cancer screening program at Wellstar through the thoracic surgeons and the pulmonary physicians. It looks at people who have had some smoking history, who are typically at more risk for developing lung cancer. They'll have a low-dose screening CT scan, and we do see a number of lung cancers get discovered earlier. That’s a worthwhile initiative when something is surgically curable, as opposed to it’s gotten so advanced that people are having symptoms.
The pandemic impact – screenings & DEI
Rubinger: During the pandemic, I didn't see my doctors as often. None of us did. It was harder to access healthcare the way we did before. What has that done?
Centers: The pandemic did change us. A lot of screening procedures at the beginning of the pandemic were paused, but we were still able to quickly to return to those services. But the temporary delay made some patients think that screening wasn't as important as it once was. We really worked hard to get the message out there about the importance of early detection.
We use a lot of automated tools like our lung nodule software to help us identify nodules in patients who come into our system for other reasons and have those incidental findings. We also work with our church network here at Wellstar. We work with BLKHLTH in Atlanta, and there’s lots of healthcare organizations that are reaching out to their communities to get people back to screening.
We at Wellstar have made a very concerted effort to go back out and say, “We have kit testing that you don't have to come into the hospital to have done. You can do that at home. Let us help you get the kits.” We reopened our screening mammography centers with all the safety protocols in place. And then we called the patients and said, “Hey, you missed your cancer screening.”
We did see an initial dip because if you're not screening, you're not finding it, as cancer usually doesn't hurt. So most people don't know that there’s something in there growing. Now we're seeing patients come in with later stages, or more advanced tumors than we traditionally would have seen. That’s because of the lag in screening.
Rubinger: Kimberly, is this consistent with what you've been seeing?
Jackson: Yes it is. Early during the pandemic, cancer screening rates decreased dramatically and an estimated 35% of Americans missed routine cancer screening due to Covid-19-related fears and care disruptions when many facilities reduced or suspended services. Screening rates remain below historical averages. In addition to the coronavirus, top barriers to screening are that individuals have no symptoms, procrastination, lack of recommendation, cost, and no insurance. During the pandemic we worked with healthcare systems to address the issue as part of the “Get Screened” initiative. Through donor support, we were able to provide $2.2 million in grant funding to 77 health partners to implement quality improvement strategies to rapidly increase cancer screening rates and reduce the barriers that have been exacerbated through the pandemic. Wellstar was one of our partnering health systems in the Get Screened initiative. They were able to increase their breast cancer screening rate by 6.8 percentage points, which resulted in over 44,000 people in Georgia being up to date with their breast cancer screenings.
Rubinger: One of the crises in our society is the ability that people have to access care. When you think about those things from the DE&I perspective, where do we see the biggest challenges and where are the biggest opportunities?
Jackson: While the pandemic is shining a light on the issue, the reality is if we were focusing on having more diverse physicians, nurses, etcetera, if we were focused more on removing the barriers and investing more, we would have fewer people who are getting diagnosed at later stages, or, you know, unfortunately losing their lives to cancer. That’s a fact. There’s an opportunity right now that we cannot shy away from. The evidence is there to show the tie between the impact on an entire community by ensuring equitable health for all by focusing on the ones that need the most is actually equalizing and improving the health of the community itself.
Rubinger: I'm curious what role can the employer play?
Jackson: The employer, they have team members and staff that make up the community that we're seeking to serve. So what they can do immediately is educate the employees on the resources that are available on the prevention side. They can also make prevention a priority and establish norms of only offering healthy snacks, for example.
As well, they can encourage employees to go to their doctors, and also for the top leaders to serve on these boards and these councils of the hospitals and organizations like the American Cancer Society, to be aware and to stay ahead of the issues and to be informed and proactive about helping the community.
Centers: There’s really three ways to look at equitable care, and it’s not a one-path journey. First off, there’s a screening environment and the diagnostic environment, getting people to the services where they are and getting them access to care.
The second part is a mistrust of the healthcare system, which is ingrained in many of our societies across the U.S., so educating them to the safety parameters we have in place to ensure that all patients have equal access to care.
The third component is to teach our healthcare providers, be they nurses, medical assistants, physicians, about diversity and the things that happen to patients who maybe don't look like you, that walk through the door. What we know is, especially among our patients of color, that when they come in, sometimes their complaints aren't taken as seriously as others. We see that in the national studies.
What we have to do is educate our providers and our healthcare workers, but also educate our patients to say “you are your own best advocate.” If you go to a doctor and you're not getting the care that you think that you need or you deserve, then you can go to another place or else you can reach out to your patient advocates at the facility that you're going to. At Wellstar, we have invested a lot of time and energy into educating all staff so that all patients who walk through the door regardless of their social standing, regardless of what they look like, regardless of their history, are all treated equitably, and we do our best.
Rubinger: Dr. McCune, anything to add on that topic?
McCune: Yes. We have a diverse group of research coordinators, both African-American and native Spanish-speaking, so I do think there are opportunities to narrow some of those health gaps. I will say the pandemic across the board affected clinical trial enrollment, because there are typically more procedures like more CT scans that a person has to go through to go on a clinical trial, than just receive what we would call standard of care therapy. So across the board, that is something that has reduced clinical trial participation and that is starting to come back.
But I do think you have to meet people where they are. We obviously have a health system that covers some urban to rural areas in Georgia. One of the things that we're able to do is take clinical trials to people who are as far west as Carrollton, as far north as Cartersville, or closer to the Atlanta area in Marietta, Austell and Douglasville. We're expanding that research network as well.
Not everybody can drive two hours. Not everybody has a family member who can drive them when they're too sick. Access to care is a huge list of things that don't sound like much but a ride to the doctor’s office, a ride to a CT scan is the difference between someone getting care or not getting care. It’s things that seem little but are really not.
When you were talking about what can corporations do, I'll just say, it seems like most people’s experience is very dependent on whether the human resources person is nice to them. From the patient’s point of view, either “they're working with me and I can show up,” or “if I have a bad day, I can just stay home,” or “they fired me yesterday.” So maybe just a little bit of grace there. People have their federally mandated leave but they need more than that. They need a little attitude of caring or just going the extra mile, to help somebody get through their cancer treatment. They'll probably be a better employee and grateful if you treat them nicely.
;
If you’re a MyChart user, E-visits are a convenient way for you to receive care from a Wellstar clinician without needing to schedule an appointment or come to the clinic.
In addition to virtual visits and our Virtual Urgent Care, Wellstar has expanded access to care with E-visits. These visits are completed using our secure patient portal and offer treatment for non-emergency conditions.
Here’s how it works
Through MyChart, tell us about your health concern by answering a few questions about yourself and your symptoms, then a primary care clinician will respond in MyChart with your care plan.
Conditions that can be treated with an E-visit include:
- cough
- sinus problems
- urinary tract infection
- conjunctivitis
- back pain
- diarrhea
- vaginal discharge
- heartburn
How to start your E-visit
Log on to MyChart and click Symptom Checker from the menu in the top left of the screen. Select your condition and confirm you are currently located in Georgia. We’ll ask for information about your medications, allergies, health history and preferred pharmacy so that our team can tailor care specifically for you. Next you’ll see the estimated cost for your visit. Finally, click Submit to contact our care team. One of our providers will follow up with your care plan.
“A Wellstar primary care provider will review the information about your symptoms and health history, and we’ll create a customized care plan just for you,” said Wellstar Primary Care Physician Dr. Monika Karakattu. “E-visits offer the same personalized care you’d receive in person at Wellstar, conveniently delivered online and on your schedule.”
Learn more about getting care with an E-visit.
If you don’t have MyChart, you can make an account online if you are an established Wellstar patient. With MyChart, you can securely access all your health records with a single username and password. Once you’re connected, you can view your test results, schedule appointments, request prescription refills and pay your bills.
Not a Wellstar patient yet? Find a primary care clinician here.

If you test positive for COVID-19 and are experiencing mild to moderate symptoms, your Wellstar care team can help you get back to feeling better with Paxlovid.
Paxlovid is an antiviral medication that can be prescribed to patients who are 12 or older and weigh at least 88 pounds. It’s best to start the medication as soon as possible, and you must begin taking it within five days of your first symptoms. Paxlovid is a pill you can take at home.
Read the U.S. Food and Drug Administration’s fact sheet about Paxlovid.
Where to get care
If you are feeling sick, you have several options for care. Learn more about the types of care available at Wellstar and what is right for your health needs.
If you have tested positive for COVID-19 with a home test and have mild symptoms, you can speak with a clinician using our 24/7 Virtual Urgent Care. They will evaluate your symptoms and work with you on a personalized care plan, including a prescription for Paxlovid if appropriate.
Patients who have tested positive with a home test can also call their Wellstar primary care clinician about a Paxlovid prescription or visit a retail pharmacy to be assessed by a pharmacist.
Wellstar retail pharmacies and many other pharmacy locations can fill Paxlovid prescriptions. Your Wellstar care team can send your prescription to your local pharmacy.
Find a location that offers COVID-19 testing and treatment. At these locations, patients are either tested on site or can bring in a positive test result from another testing site or an at-home test. Eligible patients will receive a prescription and can have that prescription filled on site.
Getting vaccinated
As new variants of COVID-19 emerge, it’s important to remain vigilant. You can do your part to “stick it to COVID” and keep yourself and the community safe by getting vaccinated. The COVID-19 vaccine is available at a Georgia Department of Public Health location or your local retail pharmacy. Find a vaccination site near you.

Ortho-On-Demand
Sports injuries, broken bones and sprains don’t have to interfere with your schedule—Wellstar Ortho-on-Demand at 1220 West Wheeler Parkway in Augusta has you covered with convenient care when you need it. Our expert team provides prompt treatment for people ages 8 and older for musculoskeletal injuries, including:
- Immediate orthopedics specialty care
- X-rays to assess fractures and breaks
- Bone, joint or muscle injuries
- Ankle sprains or strains
- Knee sprains or strains
- Hand, elbow, wrist or shoulder injuries
- Broken bones without an open wound
- Splinting, casting and bracing by specialty clinicians
- New back pain
We welcome walk-ins and offer same-day appointments for fast, efficient care. Learn more about Ortho-On-Demand.
Urgent Care
If you’re dealing with a minor injury or need care after your physician’s regular office hours, going to urgent care is often the right choice. Wellstar Urgent Care Centers provide quick, convenient care for non-emergency medical conditions.
We also offer Virtual Urgent Care, which provides virtual health visits for minor medical concerns from the comfort and convenience of home.
Wellstar Urgent Care provides:
- Care for minor injuries, such as sprains and broken bones
- Treatment for medical issues like bites, burns and cuts
- Lab and X-rays
- Sports physicals
- Occupational health services
- Worker’s compensation services
Wellstar Urgent Care has locations in Evans, Grovetown and South Augusta, or you can use our Virtual Urgent Care.
Emergency Care
In a life-threatening medical emergency, every second counts. Never put off getting the proper care when lives are on the line. Remember, driving yourself to the Emergency Department (ED) may delay care, so call 911 for the fastest access to emergency care.
When the unexpected happens, Wellstar MCG Health Medical Center’s Emergency Department is always ready. Our trained team provides expert emergency care 24 hours a day for people of all ages. At Wellstar Children’s Hospital of Georgia, the dedicated Pediatric Emergency Department team is specially trained in treating children.
Recognize the signs of a medical emergency:
- Fainting or loss of consciousness
- Sudden, severe pain
- Uncontrolled or severe bleeding
- Choking, coughing up blood or severe vomiting
- Changes in mental status, such as confusion or unusual behavior
- Traumatic injury due to a motor vehicle or other accidents
- Broken bones with an open wound
Remember, call 911 right away in a medical emergency. That way, care can begin sooner during the crucial time it takes to be transported to the hospital.
Some conditions, such as sports concussions or gout, may be best treated by a primary care or orthopedics clinician. Our Ortho-On-Demand team can refer you to other Wellstar locations if needed.
;ENABLED PAGINATION vertical limit-10/TEXT ALIGN -LEFT
.jpg?rev=0c641d247be3492db97099991e0fef7f)
To celebrate Women’s Health Month, more than 150 executives gathered Thursday at The Studio Theatre in Sandy Springs for insightful discussions on advancing women’s health in Atlanta and throughout Georgia.
The Women's Health Summit, presented by the Atlanta Business Chronicle and Wellstar Health System, featured two panels of experts and a keynote address by renowned health and wellness expert Emma Lovewell.
Cheryl Preheim, anchor at 11Alive (WXIA), welcomed attendees and served as a moderator.
;
For more than a year, our communities have done their part to fight COVID-19.
We have stayed home, worn masks when we’ve gone out, been extra careful with washing our hands and avoided large gatherings. That’s meant that holidays and birthdays have looked a little different, all so we can stay safe and healthy.
The separation and fear have been draining, and many of us have dealt with loneliness and stress as we worry about our health and our loved ones.
But now we have something to celebrate. Hope has arrived in the form of the COVID-19 vaccine. All Georgians age 12 or older are now eligible to get their shots.
At Wellstar, we've chosen to lead by example. Across our health system, frontline healthcare workers and leadership have "stuck it to COVID." Whether they want to gather with friends and family, travel to a new destination or help protect vulnerable members of the community, our Wellstar team members all have their #MyWhy — the reason they chose to get vaccinated.
For Dr. Jeffrey Hines, chief of gynecologic oncology for Wellstar, getting the shot was about a sense of responsibility. As medical director of the Wellstar Center for Health Equity, Dr. Hines works to ensure our underserved populations have access to the care they need to stay safe and healthy. He got the COVID-19 vaccine to protect those around him.
“I’m a father, I’m a husband, I’m a brother and I’m a grandfather, and it’s important for me to protect my family,” Dr. Hines said. “I understand the science, and the science is important, but equally important to me is I want to be a trusted voice to people in the community who are most at risk for this and perhaps may have the most questions.”
Dr. Sophia McIntyre, senior vice president of Wellstar Medical Group, also said she got her shot to stop the spread, noting that COVID-19 has disproportionately affected minority communities.
“The reason why I got the COVID-19 vaccine is to ensure that I’m doing my part to bend the curve,” Dr. McIntyre said. “We know that African Americans and Latino Americans are dying at a higher proportion.”
Dr. Danny Branstetter, Wellstar’s medical director for infection prevention, has been at the forefront of Wellstar’s work to fight COVID-19 and keep our communities safe. Now, he wants to see life return to normal, because health isn’t just about your body. It’s also about your personal connections and overall well-being.
“I’m tired of being separated from my friends and family. I’m tired of seeing small businesses fold,” Dr. Branstetter said. “I’m tired of seeing the increased burden this places on those without resources. I’m tired of the loneliness this puts on those who are isolated and the elderly. My question is, aren’t you tired, too?”
All of us play a part in ending this pandemic.
“We’re in this together, and we can end this together through vaccination,” Dr. Branstetter said.
To find a vaccination site near you, visit the Georgia Department of Public Health website or local retail pharmacy.
;

Christmas carols and telephones ringing filled the Wellstar Children’s Hospital of Georgia lobby December 7 through December 9, 2023 for the 23rd annual iHeartMedia Cares for Kids Radiothon.
Thanks to the generosity of supporters, a check for $262,693 was presented to Wellstar Children’s at the conclusion of Radiothon on Saturday, December 9.
Throughout the event, radio stations 104.3 WBBQ, 96.3 Kiss-FM and 105.7 The Bull broadcast live from the lobby while WRDW News 12/NBC 26 shared stories of hope. Families of pediatric patients who have successfully finished treatment or are undergoing treatment at Wellstar Children’s, which is a member of the Children’s Miracle Network, stopped by to share stories of the world-class care their children received from the caring staff and expert caregivers.
“Every dollar that’s raised this weekend with Radiothon stays right here at Wellstar Children’s Hospital of Georgia and directly benefits the care of the children,” said Pediatrician-in-Chief Dr. Valera Hudson. “We’re the second largest children’s hospital in Georgia and the only children’s hospital outside of Atlanta. We offer the highest level of care to the sickest and most complex children. We hope you never need us, but if you ever need us, we’re here.”
Donations to Radiothon are used to purchase much-needed items that are unique to a children’s hospital, such as a vein finder for the neonatal intensive care unit. This device shines a red light through an infant’s arm or leg and helps caregivers find their tiny veins without having to stick them with a needle multiple times to administer fluids and medications.
The funds are also used to provide additional supplies for patient care as needs arise.
Though Radiothon is over, pledges are accepted year-round by calling (706) 721-4004 or by visiting the Cares for Kids Radiothon website.
;
Christmas music and cheers filled the halls of Wellstar Children’s Hospital of Georgia Dec. 5 through 7 as listeners and viewers of local iHeartMedia radio stations and WRDW-TV generously supported patients and families for the 24th consecutive year.
In the end, the community pledged $255,612 to support Wellstar Children’s.
iHeartMedia generously donated the 72 hours of airtime to the cause while three of its popular radio stations—104.3 WBBQ, 96.3 Kiss FM and 105.7 The Bull—and WRDW News 12/NBC 26 broadcast live from the hospital.
“The children’s hospital could not survive without the support of the community. I’m just so grateful for everyone’s support,” said Dr. Valera Hudson, pediatrician-in-chief of Wellstar Children’s. “No children’s hospital thrives without philanthropy; 100% of the money that’s raised is used directly to help the children we take care of here. All of the funds stay right here at the Wellstar Children’s Hospital of Georgia.”
Wellstar Children’s is a not-for-profit hospital with specialists who care for pediatric patients with a range of conditions, including the most complex conditions.
Some of the patients who have been treated at Wellstar Children’s shared their stories with DJs and reporters throughout Radiothon. For example, 9-year-old Kensley Woodberry began developing spots on her hands and feet that became so painful, she could no longer walk. She stopped eating and refused to play. A team of specialists at Wellstar Children’s diagnosed her with juvenile dermatomyositis, a rare autoimmune disease that causes the body to attack its own muscles and leads to inflammation throughout the body.
This past summer, Kensley attended Camp Joint Venture, a summer camp for children with rheumatic conditions. It gives kids like Kensley the opportunity to enjoy the summer camp experience while a team of medical personnel is nearby in case they are needed. The camp is one of several summer camps funded through Radiothon.
Radiothon also allows for purchases of comfort items like Zaky Hugs, which mimic the warmth and security of a parent’s touch for babies in the NICU; red wagons for transporting young patients around the hospital; and sensory toys for children with autism. These are only a few of the items that bring joy, comfort or care to young patients that the hospital could not purchase without community support.
Though Radiothon has concluded, donations can be made throughout the year by calling (706) 721-4004, by emailing Wellstar Children’s Director of Philanthropy Catherine Stewart or through the Cares for Kids Radiothon website.
;
The iHeartMedia Cares for Kids Radiothon filled the lobby of Wellstar Children’s Hospital of Georgia Dec. 4 through 6 for its 25th year of fundraising. Surrounded by a winter wonderland of Christmas trees and red, white and silver balloon arches, volunteers took donations from generous supporters while iHeartMedia radio stations and WRDW-TV broadcast stories of the miracles that happen every day at Wellstar Children’s Hospital of Georgia.
The event raised $291,617 to support the children’s hospital, which is a part of the Children’s Miracle Network.
“Thank you, thank you, thank you! This is life-changing,” said Ralph Turner, president of Wellstar MCG Health Medical Center. “This can support many of our young patients. They come to us and we take care of them. We don’t turn them away, and this really helps support our mission.”
Dr. Valera Hudson, pediatrician-in-chief, echoed Turner’s gratitude.
“We couldn’t do this without community support. We are so grateful for everyone who is here who helped pull this off,” she said.
Each year, iHeartMedia generously donates 72 hours of airtime as DJs from 96.3 Kiss FM, 104.3 WBBQ and 105.7 The Bull join WRDW-TV to broadcast live from the event, sharing success stories from patients and families grateful for the care they received.
“Thank you, CSRA, for making miracles happen. Exactly 291,617 miracles. Thank you!” said Ivy Elam, market president of iHeartMedia in Augusta.
Donations from the iHeartMedia Cares for Kids Radiothon are used throughout the year to purchase pediatric equipment such as vein finders for babies in the neonatal intensive care unit and a gaming system for patients in the pediatric operating room.
They also support programs that are unique to a children’s hospital. These include the facility dog program, featuring three hospital-owned dogs who provide comfort and help Child Life Specialists more easily communicate with young patients. Donations also help fund summer camps for children living with chronic conditions—such as Camp Rainbow for cancer patients—which allow kids to just be kids while remaining under medical supervision.
Radiothon has ended, but donations can be made throughout the year by calling (762) 375-4004, by emailing Wellstar Children’s Hospital of Georgia Director of Philanthropy Catherine Stewart or by visiting the Wellstar Foundation.
;
Hepatitis B vaccine
What it does: Protects your baby from Hepatitis B, a virus that attacks the liver and can cause lifelong infection Why it’s important: Hepatitis B isn’t just a risk for adults later in life. Most importantly for newborns, the virus can be passed from mother to baby during childbirth. Studies show that up to 75% of mothers with chronic Hepatitis B don’t know they’re infected—and 90% of infants who catch the virus during delivery will develop a chronic infection. Chronic Hepatitis B can lead to serious liver disease, cancer or even death. What to expect: The Hepatitis B vaccine is a series of three doses given at birth, 1 month and 6 months. Side effects are rare, other than mild soreness at the injection site.Beyfortus (RSV protection)
What it does: Shields your baby from RSV (respiratory syncytial virus), a common virus that can be much more serious in infants Why it’s important: For most adults, RSV feels like a mild cold. But for newborns—especially those born prematurely—RSV can sometimes lead to serious lung infections and hospitalization. In severe cases, babies may need breathing support in the hospital. Beyfortus provides antibodies that protect your baby through their first RSV season. What to expect: One injection lasts about five to six months. The most common side effects are pain, redness or swelling at the injection site. Studies show Beyfortus reduces the risk of severe RSV illness by about 85% to 90%. Extra protection tip: Moms can also receive an RSV vaccination late in pregnancy, which helps pass antibodies to their newborns. Keeping siblings and visitors with colds away from newborns—and encouraging good handwashing—are other ways to help protect your baby.Vitamin K shot
What it does: Gives your baby the vitamin needed to help blood clot and prevent dangerous bleeding Why it’s important: Babies are born with very little vitamin K, and breastmilk and formula don’t provide enough. Without the shot, newborns are at risk for vitamin K deficiency bleeding—a rare but serious condition that can cause internal bleeding in places like the brain and intestines. These bleeds can happen suddenly and may lead to life-altering complications. What to expect: The vitamin K shot has been safely given to newborns in the U.S. since the 1960s, with no significant side effects. If you have questions about newborn immunizations, speak with your baby’s pediatrician. At Wellstar Children’s of Georgia, we’re here to partner with you through every stage of your child’s life.;
The gynecologic oncologists at Wellstar care for women at all stages of life, treating a variety of conditions with compassion and offering advanced care options. Our team are experts in treating cancers such as uterine, ovarian, cervical, vaginal and vulvar cancers. Here, we answer common questions about gynecologic cancer care with the help of Dr. Rosa Miller Polan, a gynecologic oncologist at Wellstar Cobb Medical Center.
What is a gynecologic oncologist?
Gynecologic oncologists are specialists trained in the multidisciplinary management of patients with cancers of the female reproductive tract. Trained originally in obstetrics and gynecology, gynecologic oncologists treat patients with complex benign gynecologic issues, as well as gynecologic cancer patients who may need surgery, chemotherapy, immunotherapy or a combination of different treatments.
When should you seek care?
Gynecologic cancers have different warning signs. When a person experiences concerning symptoms, a physical exam, including a pelvic exam, should be performed. Cervical and vaginal cancer symptoms include abnormal vaginal discharge, vaginal bleeding and pain. The most common warning sign for uterine cancer is abnormal vaginal bleeding. In postmenopausal women, any bleeding or spotting is abnormal and should prompt an evaluation.
Ovarian or fallopian tube cancer symptoms include bloating, constipation, pelvic or abdominal pain and difficulty eating or feeling full quickly. Vulvar cancer symptoms include itching, burning, discoloration, and new bumps or lumps on the skin outside of the vagina.
Who is at risk for developing gynecologic cancer?
Women who smoke cigarettes are at elevated risk for cervical, vaginal and vulvar cancer development. People who are immunosuppressed and those who have tested positive for the human papillomavirus (HPV) are also at increased risk. Genetics can contribute to the development of uterine, ovarian or fallopian tube cancers and these types of cancers can run in families. Obesity and use of hormone replacement therapy can put women at risk for the development of uterine, ovarian and fallopian tube cancers. A history of infertility, endometriosis and pelvic radiation are also risk factors for developing gynecologic cancer.
What services are available at Wellstar?
At Wellstar, gynecologic oncologists provide comprehensive care for patients with gynecologic cancers, including administering chemotherapy and performing surgeries when needed. As high-volume pelvic surgeons, gynecologic oncologists also care for patients who need elective and emergent complex benign gynecologic surgery.
For many patients, robotic-assisted surgery offers a minimally invasive approach with less associated blood loss, shorter hospital stays and fewer post-operative complications. Gynecologic oncologists are some of the top users of the innovative DaVinci 5 robotic surgery platform. Performing complex gynecologic cancer surgeries, minimally invasive or otherwise, requires the type of highly specialized and multidisciplinary teams that work at Wellstar—and an infrastructure of resources to ensure patients have access to best-in-class care in their own backyard.
Learn more about gynecologic oncology at Wellstar at wellstar.org/gyncancer.

By Dr. Joanna Dolgoff, Wellstar pediatrician
When school is in session, finding the perfect after-school snack that balances nutrition and deliciousness can feel like quite a task. As a board-certified Wellstar pediatrician, I understand the importance of fueling growing bodies with the right nutrients. With that, I'm excited to share five wholesome after-school snack ideas that are easy to make and fun for kids to eat.
1. Celery Caterpillars
This creative snack recipe offers a good balance of protein from peanut butter, along with a variety of fruits and vegetables, providing essential vitamins and antioxidants for growing children.
What You’ll Need:
Peanut butter
Celery
Grapes
Blueberries
Grape tomatoes
Candy eyes
Directions:
- Fill stalks of celery with peanut butter.
- Place grapes, blueberries or grape tomatoes atop celery sticks. These will be the body and head of your caterpillars.
- Apply peanut butter to the backs of candy eyes, then place eyes on grape, tomato or blueberry to create face.
- Optional: Cut thin matchsticks from a celery stick and place behind candy eyes to create the antennae.
2. Apple Sailboats
This recipe is excellent for kids as it combines the crisp sweetness of apples, a good source of fiber and vitamins, with protein-rich peanut butter and the added crunch of Cheerios to create a tasty and nutritionally balanced snack. Toothpicks may be a choking hazard for children, so supervise as your family makes and enjoys this snack.
What You’ll Need:
One apple
Peanut butter
Cheerios
Low-fat cheese
Toothpicks
Directions:
- Cut apple in half and remove the apple’s core.
- Spread peanut butter across the flat side of your apple halves.
- Place Cheerios on top of peanut butter spread.
- Using a thick slice of cheese, cut triangular sails for your apple boats.
- Attach sail to boat using toothpick.
3. Krazy Kabobs
This krazy kabob recipe is a playful and nutritious way to encourage children to enjoy a variety of fruits. Filled with hydrating watermelon, sweet cantaloupe, refreshing honeydew, juicy pineapple, antioxidant-rich blueberries and grapes, these skewers provide a spectrum of vitamins and flavors, promoting a fun and healthy snacking experience for young taste buds.
What You’ll Need:
Watermelon
Cantaloupe
Honeydew
Pineapple
Blueberries
Grapes
Wood skewers
Fruit-shape cutters (stars, hearts, etc.)
Directions:
- Cut horizontal slices of your larger fruits (watermelon, cantaloupe and honeydew).
- Use your fruit cutters to cut shapes out of your fruit slices.
- Place any creative combination of fruits or fruit shapes onto your skewer to create the ultimate krazy kabob.
4. Veggie Cars
This wholesome veggie car recipe is a fun way to encourage children to enjoy their vegetables. With vibrant baby peppers and baby cucumbers, the snack not only provides essential vitamins, but also engages kids in a fun, hands-on experience of assembling their own veggie cars, promoting both healthy eating and interactive play. Toothpicks may be a choking hazard for children.
What You’ll Need:
10 baby peppers
Six baby cucumbers
Toothpicks
Directions:
- Slice cucumbers into half-inch rounds, discarding the ends. These will be your wheels.
- Place two toothpicks through each pepper. The toothpicks will serve as the axels to your cars.
- Push one cucumber round onto the ends of each toothpick to form the full car.
5. Banana Lollipops
These banana lollipops offer a delightful and healthier alternative to traditional sweets. With the natural sweetness of bananas and the richness of dark chocolate, the recipe makes for an enjoyable, nutritious after-school snack for kids of all ages.
What You’ll Need:
One banana
Chopped dark chocolate bar
Popsicle sticks
Wax paper and baking sheet
- Unpeel banana and slice into inch-thick rounds, discarding the ends.
- Insert one popsicle stick into each round.
- Place chopped dark chocolate into microwave-safe bowl and heat until melted.
- Dip each banana round into chocolate.
- Place popsicles onto wax paper-covered baking sheet and let freeze for 45 minutes.
As a pediatrician dedicated to the well-being of children, these snack ideas offer more than delicious bites—they pave the way for a lifetime of healthy habits. Incorporating a variety of fruits and vegetables, these recipes not only provide essential vitamins and minerals, but also engage young minds in the joy of preparing and enjoying wholesome foods. Learn more about how to keep your kids happy and healthy by scheduling an appointment with a world-class Wellstar pediatrician today.
A graduate of New York University Grossman School of Medicine, Dr. Joanna Dolgoff is a board-certified pediatrician with Wellstar.
Wellstar’s content, and all related media, are provided for educational and informational purposes only and does not constitute providing medical advice or professional services. Consult a pediatrician for the diet that’s best for your child.
;
Small changes add up to big results. By incorporating simple habits into your life, you can kickstart your wellness journey and stay on track for the long run.
Setting healthy, realistic goals
Use the SMART goal-setting system to help define your goal and develop attainable resolutions.
- Specific—Be clear about exactly what you want to accomplish. Include as many details as necessary, such as potential obstacles or extra requirements.
- Measurable—Measure your progress and determine how to meet the goal. If you have a big goal, you may need to set smaller milestones to stay on track.
- Achievable—Attainability is an important factor to consider when it comes to goal setting. “While behavior change comes with any resolution, it is unfair to yourself if you set a goal that is not feasible,” said Dr. Rebecca Gomez, Wellstar clinical health psychologist and Clinician Resiliency & Well-Being Program lead.
- Relevant—Align your resolutions with your overall life goals and think about what you hope to accomplish by reaching that goal.
- Time bound—Set a realistic, target deadline to reach your goal with checkpoints at intervals along the way. Markers provide an opportunity to measure progress and reassess any changes needed to stay on track.
Keep in mind, you may encounter some bumps in the road along the way. Recognizing all the small accomplishments can help you stay motivated and win in the long run.
“Focus on what small steps you’ve accomplished rather than how far you have to go,” Dr. Gomez shared. “Also, have a resiliency plan to help you bounce back after a more challenging day.”
Build new habits into your regular routine by beginning small and adding on over time. With this “habit stacking” technique, you pair your new habit with something you’re already doing. For example, if your goal is to drink more water, drink a glass of water while making your morning coffee or tea.
Schedule a wellness exam
Seeing your primary care clinician at least once a year is the single most important thing you can do for your health.
At your annual exam, your care team will help keep you healthy and reach your wellness goals. They screen for diseases to stay ahead of medical issues and check in on your overall well-being.
Set a reminder on your phone or calendar to prompt you to book an appointment. You can also use an important date, such as your birthday, anniversary or a holiday, as a marker to remind you to schedule a visit.
Get moving to stay well
If you’re focused on improving your fitness routine, put a plan in place to be more active.
“Begin to incorporate a little more exercise into your daily routine,” said Wellstar Primary Care Physician Dr. Jeremy Boyd. “The Centers for Disease Control and Prevention offers a suggestion of 150 minutes of aerobic activity a week. I like to break that down to a good 40 minutes four times a week.”
Set a sleep routine
Having a bedtime routine is essential to catch more Zs throughout the year. When you wake up feeling rested, you often feel more productive and energized throughout the day.
Get started by setting a specific time to go to sleep—and stick to it. Make sure you reserve at least seven to nine hours per night for sleep.
Limit your screen time before getting in bed. Bright screens from a phone, computer or TV can keep your brain awake and make it harder to fall asleep.
If you’re having trouble getting to sleep, have a decaffeinated cup of tea or take a warm bath to help you relax.
Eat a balanced diet
When it comes to losing weight, many people look for a quick fix, which can often create unhealthy ways of eating. Creating a healthy eating plan from the start can help avoid any fad diet pitfalls.
Nutrition plans that restrict or eliminate food groups and those with extreme calorie deficits are difficult to maintain and can often produce more weight gain or undesired results, according to Wellstar Registered Dietitian Kelly Prian.
Diet trends can also create a negative relationship with food, which can make it harder to achieve your goals. Prian shared that those with long-term success focus on maintaining a plan that enables steady weight loss over time.
A healthy nutrition plan is balanced and emphasizes whole foods, such as fruits and vegetables, lean proteins, low fat dairy, nuts and seeds, and whole grains.
Try not to overcomplicate healthy eating. You can start by filling half your plate with vegetables or having fun trying new recipes.
Take care of your mental health
Self-care is an important aspect of your mental well-being and should be made a consistent part of each day.
“Make self-care a priority and a non-negotiable,” Dr. Gomez said.
“Think of self-care as a form of personal healing and a way to strengthen resilience,” Dr. Gomez explained. “Much like the way exercise enhances physical health, self-care enhances mental health.”
According to Dr. Gomez, it can be helpful to turn tasks we do on “autopilot” into more meaningful experiences.
“When washing your hands, give yourself a hand massage,” Dr. Gomez shared. “When driving, use red lights to practice deep breathing. Listen to a book on tape or language lessons rather than the radio or call someone to reconnect.”
If you feel overwhelmed by stress or anxiety, Wellstar behavioral health specialists are here for you.
“Working with a mental health provider is different than speaking with a friend or even a life coach,” Dr. Gomez said. “Mental health professionals are trained and licensed to address psychological or emotional wellness.”
Need support? Connect with a Wellstar behavioral health specialist.
;
Pay attention to early signs of stress.
Recognizing stress early is key to managing it effectively. When stress becomes chronic, it can affect both your mental and physical health. Learning to identify warning signs can help you take action before it escalates. This is true across all areas of life, including the workplace, where job stress can quietly build over time and lead to more serious mental health concerns if left unaddressed. “Paying attention to feelings of emotional exhaustion and general cynicism is important,” said Dr. Ryan Breshears, a board-certified clinical health psychologist and chief behavioral health officer at Wellstar. “Those are the foundational signs of occupational burnout, which certainly affects our well-being in the workplace, but when unchecked, can also spill over into our personal lives.” That spillover can show up as irritability, mood changes, social withdrawal or insomnia. “Any of those could point to a problem that warrants intervention,” Dr. Breshears said.Treat your whole health to support your mental well-being.
Mental and physical health are deeply interconnected—and we shouldn’t treat them in silos. At Wellstar, integrated care is a key part of our approach. “I think the days of talking about problems that are physical problems versus mental problems are over,” said Dr. Breshears. “We have a body of research now and decades of science that show the interplay between the physical and the emotional.” He explained that changes in thinking patterns can trigger physiological shifts in heart rate, stress hormone levels and more. Recognizing these mind-body connections can help you take a more proactive approach to your mental health. “Wellstar is making a concerted effort to deconstruct old ideas about mental health and remove barriers to access,” Dr. Breshears added. “For example, we’re bringing behavioral health into primary care, cardiac care, pediatrics and women’s health. We want to strategically integrate behavioral health services wherever patients are receiving care.” By treating the whole person and bringing behavioral health into every corner of healthcare, Wellstar is helping people take charge of their well-being in a way that’s compassionate, connected and convenient.Prioritize recovery.
Stress is inevitable, and recovery is essential. Without it, your mind and body stay in overdrive, increasing your risk for burnout and long-term health issues. Taking time to recover is not a sign of weakness—it’s a strategy for resilience. “Our bodies are designed to return to baseline, what we call homeostasis, after high-stress periods,” Dr. Breshears said. “Research suggests it's often the failure to prioritize recovery, not the stress itself, that actually contributes to the most lasting problems.” Dr. Breshears shared a study comparing elite marathon runners to non-elite runners. The surprising finding? Elite runners were better at identifying stress early and adjusting their pace to recover, ultimately helping them perform better. That same principle can apply to your mental health. If you notice signs of stress—like fatigue, irritability or changes in focus—take time to reset. That might mean getting more sleep, going for a walk, reaching out to a friend or seeking professional support. Being intentional about recovery helps you maintain balance, build resilience and continue showing up for what matters most.Nurture relationships and workplace well-being.
Meaningful relationships are a powerful buffer against stress. For many people, the workplace is a central source of community—and a critical place to nurture mental health. “We’re social creatures,” said Dr. Breshears. "Having environments where people come in and feel good about their day-to-day interactions is really important.” Dr. Breshears said it starts with employers being committed to understanding the inadvertent threats to their team’s well-being and removing barriers to care. “First, I think we have to pay attention to the occupational drivers of stress on our employees and commit to resolving those issues,” he explained. “All of the human resources and benefits in the world will fail if we’re not also working upstream to eliminate the root causes. Secondly, we need to establish clear pathways so people can easily access support without all the stumbling blocks and delays they often run into.” Employers who lead with empathy—and prioritize flexibility, compassion and connection alongside performance—help create cultures where people feel empowered to seek help when needed. “We have to ensure that we have accessible resources,” Dr. Breshears said. “People bring their personal struggles into the workplace, and take their struggles in the workplace home. The lines have certainly blurred.”Know when to seek help.
While self-care and support systems can go a long way, there are times when professional help is essential. Mental health conditions are common—and treatable. The sooner you seek help, the better. This is especially true for men, who often face cultural and emotional barriers when it comes to seeking support. “Men on average tend to delay help-seeking more than women,” Dr. Breshears said. “And this is especially true when men are suffering. Frankly, it's a mortality issue.” He noted that men are more likely to die by suicide and experience substance abuse disorders, which makes early intervention even more critical. Dr. Breshears also emphasized the need to remove barriers and promote action: “We have to create environments in which people feel safe to talk about the struggles that they’re having.” If you’re struggling, don’t wait. Explore Wellstar Behavioral Health services and find the support you need today. If you or someone you know is in crisis, call or text 988 for the Suicide and Crisis Lifeline, or contact the Crisis Text Line by texting TALK to 741741.;
Let’s cut to the chase: What is the best way to lose weight?
Dr. Rubin: There is no magic fix that works for everyone. Many people have tried every fad diet out there. They’ve tried being more active. Maybe they’ve even had bariatric surgery or used injectable weight loss drugs—but nothing works. If this sounds like you, schedule an appointment at a comprehensive weight loss center. Find one that offers medical and surgical treatment options and personalized recommendations. And make sure they provide ongoing support to help you meet and maintain your weight loss goals. Dr. Hilton: Both of our centers take this comprehensive approach. We use every tool available to treat obesity. You may be successful with lifestyle changes alone, or perhaps you need to meet with a behavioral therapist or consider surgery, medicine or a combination of therapies. Everyone is unique, and their treatment plan has to be unique too.What’s your take on weight loss injectables—are you a fan?
Dr. Rubin: I’m excited about drugs like Wegovy and Ozempic, which people sometimes refer to as GLP-1s. They work because they control your appetite and reduce ‘food noise,’ a persistent, unwanted focus on food. However, not everyone can tolerate the side effects, which include nausea, constipation and diarrhea. If you want to lose more than 20% of your body weight, using one of those drugs alone probably won’t get you there. Another consideration is that many people need to continue taking these drugs for life—even after they reach their weight loss goals.What are some misconceptions about bariatric surgery?
Dr. Hilton: Two big misconceptions are that bariatric surgery is dangerous and it doesn’t work. Here’s what I’d say: First, bariatric surgery is as safe as a routine procedure like gallbladder removal. Second, bariatric surgery is the most long-lasting and effective treatment for obesity available. Most people who have bariatric surgery maintain their weight loss at the 10-year mark.With weight loss drugs dominating the headlines, have you noticed a shift away from surgery?
Dr. Hilton: Yes, but I think that’s temporary. The drugs are sparking conversations about obesity and weight loss, which is a good thing. Patients who have never considered bringing up obesity to their primary care provider are asking about the injectables. They’re making appointments at a comprehensive weight loss center, and they are discovering they have a lot of choices. It isn’t ‘medicine or surgery’ or ‘medicine versus surgery.’ Sometimes the best answer is both.Can you share a weight loss success story with us?
Dr. Rubin: We’ve had so many success stories. One of our rock star patients has lost 250 pounds under our care. Now, she’s living her life again. Her diabetes is in remission, and her cholesterol has improved. She’s no longer depressed and isolated. My whole team is so proud of her—she has completely changed her lifestyle, sees our dietitian regularly and attends our support group. Another patient has lost 135 pounds. He and his wife are losing weight together, and it’s fantastic. Dr. Hilton: We ask our patients at their first visit, ‘What does success look like to you?’ Most have a number in mind, but non-scale victories are important too. Some want to get off their diabetes medicine or shop in a regular store instead of a big and tall store. Others want to take their kids to Disney World or a water park and have fun on the rides—not just watch.What is the No. 1 key to weight loss success?
Dr. Rubin: The key is to make lasting lifestyle changes. Medication and bariatric surgery can only get you so far. If you are ready to make these changes, consider finding a team who offers personalized, long-term support. Dr. Hilton, myself and others at Wellstar are here to help! Ready to take your first step? If you’re considering lifestyle changes, medication or surgery for weight loss, it all starts with a conversation. Schedule a visit with your primary care clinician to discuss your goals, health history and next steps.;
1. High blood pressure can be silent—and dangerous.
Some women develop high blood pressure during pregnancy, even if they’ve never had it before. High blood pressure can lead to preeclampsia. It’s a condition that can cause organ damage and, in severe cases, seizures. When high blood pressure isn’t treated, it can increase the risk of stroke or heart failure. Checking your blood pressure regularly can help catch problems early.What to do about high blood pressure
If you have a history of high blood pressure, heart disease or a family history of cardiovascular issues, tell your care team. Preconception counseling is essential if you have a known heart condition. Your physician may recommend that you monitor your blood pressure at home and report any sudden swelling, headaches or vision changes immediately.2. Heart failure can happen—even in healthy moms.
A rare but serious condition called peripartum cardiomyopathy (PPCM) weakens the heart, usually in the last month of pregnancy or the months following delivery. If you have shortness of breath, swelling or often feel extremely tired, don’t ignore those signs.What to do if you have shortness of breath or a racing heart
Talk to your provider immediately if everyday activities leave you exhausted or struggling to breathe. Other concerning symptoms include persistent coughing, swelling in your legs or feet and dizziness. Don’t ignore symptoms like chest pain, shortness of breath, severe fatigue or a racing heartbeat. These could signal a serious heart problem—seek help right away.3. Pre-existing heart conditions and hypertensive disorders require extra care.
If you’ve ever had heart disease, a heart defect or high blood pressure—including hypertension or hypertensive disorders—pregnancy can increase your risks. Even women without symptoms before pregnancy may need extra monitoring.What to do if you have a pre-existing heart condition
Talk with your provider early about a care plan. High-risk pregnancies may require specialist support, like a maternal-fetal medicine physician or cardiologist. If you’ve been diagnosed with a heart condition before pregnancy, ask your provider how it may affect labor and delivery. If something doesn’t feel right, speak up. You know your body best, and your concerns deserve attention.4. Blood clots are more common during pregnancy.
Pregnancy increases the risk of thromboembolism, a serious condition where blood clots can travel to the lungs and cause a pulmonary embolism. The risk is even higher for women with a history of clotting disorders, obesity or limited mobility.What to do to prevent blood clots
To reduce your risk of blood clots, stay active, stay hydrated and watch for warning signs like leg swelling, redness or pain. If you notice these, call your provider right away. If you’re on bed rest, ask your provider about ways to improve circulation. Learn the signs of deep vein thrombosis and pulmonary embolism.5. A racing heartbeat may be abnormal.
You can expect some changes in heart rhythm during pregnancy, but arrhythmias (irregular heartbeats) can be a sign of something more serious. Hormone changes, increased blood volume and underlying conditions like thyroid disorders can all contribute to an irregular heartbeat.What to do about a racing heart
If your heart races often, feels like it’s skipping beats or you feel dizzy or faint, let your provider know immediately. Keep track of when these symptoms happen and whether they occur at specific times, such as during physical activities or when your stress levels are high.6. Postpartum recovery still puts stress on the heart.
The risk of heart complications doesn’t end at delivery. Many serious conditions, including heart failure or high blood pressure, can develop in the weeks or months after childbirth. Postpartum heart issues can be life-threatening if you don’t address them.What to do during the postpartum period
Keep all postpartum checkups, even if you feel fine. Watch for new symptoms like chest pain, shortness of breath or extreme fatigue. If you had high blood pressure during pregnancy, continue monitoring it after delivery. Be aware that cardiovascular complications can develop up to a year postpartum, and follow-up care is so important for your long-term health.7. Your hospital choice matters
For women at high risk, delivering in a hospital with access to specialized prenatal tests, genetic testing like amniocentesis, fetal evaluations and emergency cardiac care can make all the difference. Not all hospitals have the same level of maternal heart care, so it’s important to plan ahead. Choose a hospital that is equipped to handle pregnancy-related cardiac emergencies. Wellstar provides specialized care for mothers and babies close to home, including:- Wellstar Acworth Health Park: Perinatal cardiology
- Wellstar Avalon Health Park: Perinatal cardiology
- Wellstar Cherokee Health Park: Perinatal cardiology
- Wellstar Children’s Hospital of Georgia: Level IV NICU
- Wellstar Cobb Medical Center: Emergency cardiac care, level III NICU, maternal-fetal medicine, medical genetics, perinatal cardiology
- Wellstar Douglas Medical Center: Emergency cardiac care, maternal-fetal medicine
- Wellstar East Cobb Health Park: Perinatal cardiology
- Wellstar Kennestone Regional Medical Center: Emergency cardiac care, Level III NICU, maternal-fetal medicine, medical genetics, perinatal cardiology
- Wellstar MCG Health Medical Center: Cardio-obstetrics, emergency cardiac care, maternal-fetal medicine, medical genetics
- Wellstar North Fulton Medical Center: Emergency cardiac care, medical genetics
- Wellstar Paulding Medical Center: Emergency cardiac care, medical genetics, perinatal cardiology
- Wellstar Spalding Medical Center: Maternal-fetal medicine
- Wellstar Vinings Health Park: Perinatal cardiology
- Wellstar West Georgia Medical Center: Emergency cardiac care
What to do about your hospital choice
If you are high-risk, consider hospitals with advanced cardiac care and those that have expertise in pregnancy-related heart conditions. Talk to your care team well in advance about your birth plan, especially if you have a heart condition. If possible, tour the hospital beforehand and ask about its capabilities in managing pregnancy-related heart complications.8. Mental health and stress impact heart health.
Anxiety and stress can affect your heart. If you’re feeling overwhelmed, talk to someone. Your mental health is just as important as your physical health. Depression, anxiety and even post-traumatic stress disorder are common in pregnancy and postpartum, and they can impact heart health.What to do to keep your mental health in check
Access mental health resources and practice stress management techniques to help you manage your mental health. Simple practices like deep breathing, mindfulness and connecting with loved ones can help lower stress levels. Remember, you are empowered to take control of your health—talk with your provider or a support person and get the help you need.Take Action for a Healthier Pregnancy.
Eat well, stay active and avoid smoking or alcohol. These efforts can protect your heart and your baby’s health. Small, consistent changes—like reducing salt intake or walking daily—can make a difference. Regular prenatal visits are just as important. Remember, knowledge is power. Stay informed, speak up when something feels off and choose a hospital that meets your needs. These simple steps can help you take control of your heart health and reduce the risk for you and your baby. Find an OB/GYN or perinatal cardiologist and learn about labor and delivery at Wellstar.;
According to the Centers for Disease Control and Prevention (CDC), about 1 in 10 Americans have diabetes. Of that group, 90 to 95% have type 2 diabetes. Because this condition often develops in people over 45, getting screened and getting the best treatment to live your healthiest life is essential.
"Diabetes is a chronic and complex condition, and treatments are continuously changing," said Dr. Georgia Forrest, Wellstar primary care physician. "Teaming up with a primary care provider who personalizes your care plan to you and everything that makes you unique should be a top priority."
Whether you currently have type 2 diabetes, a family history of the disease or feel concerned about your overall well-being, you can take proactive steps to manage your health. Here are some key facts to help you better understand the relationship between diabetes and good health.
1. Undiagnosed diabetes costs you money & health
Not knowing you have diabetes carries high medical costs. Undiagnosed diabetes can increase your risk for death and other medical issues.
Diabetes was the eighth leading cause of death in 2021, the most recent data reported by the U.S. Preventive Services Task Force. And according to the American Diabetes Association, having diabetes doubles your risk for heart disease and stroke—heart disease is the number one killer in the U.S.
2. A diagnosis and personalized treatment can save your life
Knowing you have diabetes and then working to manage your blood sugar, blood pressure and cholesterol effectively can lower your risk of death and help you live a better quality of life.
3. Getting screened for diabetes is easy
The U.S. Preventive Services Task Force now recommends getting screened with a simple blood test at the age of 35 for people with no symptoms but who are overweight or obese. Even if you have no signs or family history of diabetes, it can lurk in your numbers. Getting screened can help you catch it early and even prevent it altogether.
Consider getting screened for diabetes if you:
- Are obese or overweight
- Are physically inactive
- Have a parent or full sibling with diabetes
- Are an African American, Latino, Native American, Asian American or Pacific Islander
- Have a history of cardiovascular disease
- Have hypertension
- Have blood work that shows an HDL of less than 35 mg/dl or triglycerides greater than 250 mg/dl
- Have a diagnosis of polycystic ovarian syndrome
- Have other medical conditions that lead to insulin resistance
4. Some people have pre-diabetes
If your screening shows that you have pre-diabetes, your blood sugar levels run higher than average but aren't within the range of type 2 diabetes. However, you have an increased risk of getting type 2 diabetes.
Identifying that diabetes is around the corner can help you stop it before it starts.
5. Diabetes treatment plans should be unique
When crafting a plan to address diabetes, the conversation must be about more than the numbers.
"Additional diseases or conditions you may be experiencing in conjunction with your diabetes should also become part of your individualized health plan," Dr. Forrest said.
A complete medical history helps your healthcare provider understand how other medications and treatments may interact with your symptoms and treatments related to type 2 diabetes.
6. Lifestyle modifications can make a big impact on diabetes
Lifestyle modifications may involve slight changes to your weight, the amount of exercise you get, your diet and even your sleeping patterns.
Changes don't have to be major. For instance, your doctor may suggest you lose around 10 pounds and exercise for 30 minutes five days a week.
Our primary care providers work with patients one-on-one but can also refer patients with pre-diabetes and diabetes to Wellstar Diabetes Services to help prevent the onset or manage the effects of diabetes.
7. S.M.A.R.T. diabetes treatment plans
According to Dr. Forrest, your overall plan should include "specific, measurable, achievable, relevant and timely (S.M.A.R.T.) goals and involve shared decision-making between you and your care provider. There should be plenty of follow-ups to keep the conversation fluid and open to modification."
8. Know your numbers — and acronyms (A1C, CGM, TIR)
Should your screening lead to a type 2 diabetes diagnosis, conversations with your health providers will focus on several acronyms and numbers.
"Know your ABCD’s of diabetes," said Dr. Forrest. "Your A1C, blood pressure, cholesterol and the medications you are taking. Knowing these facts about your health will be key to your success."
• A = Hemoglobin A1C goal is <7
• B = Blood pressure goal is <130/80
• C = Cholesterol goal is to keep bad cholesterol <100
• D = Drugs
Keeping the A1C low and within an optimal range will help prevent complications like eye damage, blindness, kidney failure and nerve damage.
A mainstay for type 2 diabetes management centers around constant glucose level monitoring. Continuous glucose monitoring (CGM) provides readings every few minutes via a sensor inserted just below your skin. Monitoring glucose is a common way to help regulate insulin in your body, giving you the readings you need to self-adjust with insulin when appropriate. Average glucose levels should be 100 mg/dl or lower though they can increase if you've just eaten.
New developments introduced the importance of tracking Time in Range (TIR). Along with monitoring your glucose levels, TIR may impact your customized plan for maintenance. According to Dr. Forrest, the goal for TIR is 70% or more.
9. Receive individualized diabetes care at Wellstar
For diabetes management, a personalized, proactive approach can make all the difference. Wellstar primary care providers are here to partner with you to help prevent or manage diabetes, heart disease and many other conditions.
"A true patient-centered approach for managing diabetes is the key to the future of this disease," Dr. Forrest said. "Get screened and speak up when it comes to your care. Opportunities for personalized and individualized medicine should be a part of your treatment plan as you move forward."
Find a primary care provider near you.

Over the years, advice about breast self-exams and breast cancer screenings has changed. So what exactly should you be doing to make sure you’re staying your healthiest? We brought together a panel of women’s health experts to discuss the best strategies to keep tabs on your breast health—and who to talk to if you’re diagnosed with breast cancer.
I do breast self-checks every month. Why do I need a mammogram too?
Dr. Paula Greaves, MD, OBGYN, Wellstar chief Women's Health officer: Unfortunately, 1 in 8 women will develop breast cancer in their lifetime, so early detection is key. We have shown over the years that the sooner we detect breast cancer, the more successfully it can be treated. Survival has increased significantly since we started finding breast cancer earlier—before there are symptoms, such as feeling a lump during a self-exam.
Mammograms are essential for early detection. It’s recommended that women start getting mammograms at age 40. However, if you have a family history of breast cancer or other risk factors, your gynecologist or primary care provider may recommend starting earlier and will help you create a personalized screening plan. There are some risk factors that women cannot change, such as genetics, but there are some ways women can lower their risk, like quitting smoking, eating a healthy diet and exercising regularly. Wellstar offers 16 mammography locations, and our patients have state-of-the-art technology on their side. We offer high-resolution breast screening, including 3D mammograms.
Women should continue not only getting annual mammograms, but also seeing their gynecologist or primary care provider for regular breast exams. Women should also be aware of physical changes within their bodies, including breast changes. Changes in the texture of the skin or a lump or pain in the breast should always be checked out by their healthcare provider.
Margie Apacible-Mancao, MSN, RN, CBCN, nurse navigator: I am so passionate about breast cancer screening—every opportunity I have I tell patients to get a screening mammogram when they’re of age. Tell someone in your circle that you’re going, then they’ll tell someone in their circle and the circle gets wider so more people will get screened.
Does it mean I have cancer if the doctor recommends a biopsy?
Dr. Sujatha Hariharan, MD, medical oncologist: When a mammogram detects an abnormality, a biopsy might be indicated. Many breast biopsies will be non-cancerous such as fibroadenomas.
If cancer is found on a breast biopsy, there are several parts of the pathology result that the care team will utilize to make a treatment plan. For example, the presence of estrogen and progesterone receptor positivity allows the potential for hormone therapy as part of the treatment plan. The HER-2 gene is also tested for and if that is present and positive, it allows for medication directed at the HER-2 gene to be given along with chemotherapy.
Sequencing of the various treatments for breast cancer—surgery, chemotherapy, radiation and hormone therapy—will be determined as a collaborative effort between the breast surgeon and medical oncologist.
If I’m diagnosed, who should I talk to next?
Margie: The anxiety of not knowing their diagnosis or what’s next is one of the hardest parts. At Wellstar, patients have access to a nurse navigator on the day they are recommended to have a biopsy. We make an appointment with the specialists as quickly as possible because just knowing that someone is helping them get to the next step and get that appointment fast dials down their stress level.
Dr. Karen Xu, MD, radiation oncologist: If you are diagnosed with breast cancer, you will need to see a breast surgeon first to discuss your surgery options—lumpectomy or mastectomy; a radiation oncologist to discuss the duration of radiation treatment and whether lymph nodes should be included in the target; and a medical oncologist about whether endocrine therapy or chemotherapy is indicated and the timing of systemic therapy. Patients who desire reconstruction after mastectomy will discuss with a plastic surgeon the type and timing of reconstruction they want.
Schedule a mammogram
Find a breast imaging location near you online or call (678) 581-5900.

Heart attack is the leading cause of death in Georgia, according to the American Heart Association. To save more lives, Wellstar provides advanced heart care services, ranging from minimally invasive procedures to open heart surgery. The health system recently expanded its offerings to bring an advanced technology called rotational atherectomy to more people in our community. The tool our physicians use for this procedure is called a Rotablator, which has a small but mighty diamond tip.
Who rotational atherectomy helps
Wellstar has offered percutaneous coronary intervention (PCI), formerly known as angioplasty, for a number of years. This procedure helps treat the main cause of heart attacks—the build-up of cholesterol filled plaque within a coronary artery. The build-up decreases blood flow and oxygen to the heart. By opening the artery, blood and oxygen can move freely once again.
The benefits of having a PCI typically include fewer complications, faster recovery time and shorter hospital stays.
Not everyone is a candidate for PCI, especially when the blockage is heavily calcified. But rotational atherectomy changes that.
“For heavily calcified coronary blockages, rotational atherectomy works as a drill to decrease the bulk of calcium,” said Wellstar interventional cardiologist Dr. Omer Mirza.
This technology makes non-surgical heart attack treatment available to people with more complex blockages that could not typically be cleared with balloon angioplasty.
Rotational atherectomy has been available at Wellstar Kennestone Regional Medical Center, and now we have expanded availability recently to Wellstar Cobb Medical Center.
“By expanding Wellstar Cobb’s technology, we can offer more comprehensive care for the patient and prevent transfers and subsequent delays to patient care,” Dr. Mirza said.
How rotational atherectomy works
At Wellstar, a rotational atherectomy is performed using a Rotablator, a small, diamond-tipped tool. This revolving instrument is inserted into the blocked artery using a catheter while a patient is under local anesthesia.
When the interventional cardiologist guides the Rotablator to the blockage, it begins to rotate, going as fast as 190,000 rpm. It gently breaks apart the blockage, making the plaque particles small enough to pass safely through the bloodstream.
Stents are then placed in the artery to widen it so blood can flow through. This procedure can improve blood flow and heart function within minutes.
Effective treatment with advanced technology
Studies indicate that rotational atherectomy results in high procedural success rates.
Giving patients the ability to resume normal activities within a few days, the recovery time for this procedure is significantly less than open heart surgery. Patients undergoing a rotational atherectomy typically spend one night in the hospital.
Learn more about interventional cardiology at Wellstar or find a specialist near you.

It all started with a gift and a special note.
April Sather had just undergone surgery for her breast cancer and was struggling to sleep at night. She would spend the night tossing and turning, trying to get comfortable. “I’m a side sleeper, so that is kind of an issue,” she said when describing her sleeping troubles.
One day she received a gift from a friend: a heart-shaped pillow made with soft flannel that was light pink with beautiful clouds across it. Sather was able to tuck it under her arm and sleep comfortably throughout the night. This gift, combined with a lovely note from one of her nurses after surgery, inspired Sather to want to do the same for others.
“I thought, ‘Wouldn’t it be cool if we could make heart-shaped pillows for other breast cancer patients so that after they get out of surgery, they could feel that same love that I received?’” Sather said. “I shared the idea with a few ladies at church, and the rest is history.”
Healing Hearts Ministry at Warren Belvedere Church now meets once a month to sew, stuff, pray, write notes and package up the hearts to be delivered to patients with breast cancer across the CSRA. There is no commitment, and volunteers are welcome to take the materials with them if they prefer to work in the comfort of their own homes.
“It makes me feel like I’ve done something that’s worthy of helping someone else go through a hard time in their life,” volunteer Susan Elliot shared about each time the group finishes a pillow to be delivered to a patient.
Elliot is one of the women who answered Sather’s call for help with her idea. While she has no personal experience with breast cancer, she is a seamstress and was more than happy to use her knowledge and experience with sewing for the program.
Healing Hearts provides the sewing pattern, fabric and fluff needed to create the pillows, so all that volunteers have to bring are their hands and good spirits. Sometimes the group welcomes speakers during the meetings; in fact, they celebrated their first anniversary by inviting a Wellstar Georgia Cancer Center patient and breast team nurse navigator to come and share their story.
If you would like more information or to make a donation to assist the program, visit the church’s website, select the Belvedere campus, then make the message out to April Sather or Susan Elliot. You can also get in touch through the church’s Facebook page.
;


Dr. Joanna Dolgoff, Wellstar Children’s of Georgia pediatrician and author of the bestselling book “Red Light, Green Light, Eat Right,” uses her “no time, some time, never all the time” philosophy to provide families with guidance around screen time. At nearly every wellness visit, Dr. Dolgoff talks with parents about how to set healthy limits with screen time. “We’re seeing language delays in children from too much screen time,” she explained. Some signs that children may be spending too much time on social media, gaming or watching videos can include:
- Aggression
- Difficulty handling boredom without a screen
- Trouble connecting with peers
- Sleep disruption
- Poor focus in school
- Withdrawing from hobbies or activities they once enjoyed
Troubling trends in children’s media habits
Common Sense Media is a nonprofit organization that advocates for children’s health in the digital age. Its most recent survey of the digital habits of children 8 and younger showed that by age 2, 40% of children have their own tablet. By age 4, that number climbs to 58%. The survey also found that 1 in 5 children use mobile devices during meals, at bedtime or to cope with emotions. Dr. Dolgoff stresses that parents must monitor and regulate their children’s digital use across all platforms. Yet the same survey shows gaps in how families co-view content: 62% of parents occasionally watched YouTube with their children, compared to only 17% on TikTok. The survey also found that screen use varies by income. Children in lower-income households spend twice as much time on screens (3 hours, 48 minutes) as those in higher-income households (1 hour, 52 minutes).Guidelines for screen time by age
As a spokesperson for the American Academy of Pediatrics, Dr. Dolgoff suggests that parents know and follow the organization’s screen time guidelines for children:- Under 18 months: No screen time
- 18 to 24 months: Only educational content with parents
- 2 to 5 years: No more than one hour per day
- 6 years and older: Balanced screen time that doesn’t interfere with family, friends and schoolwork
What do screen time limits look like?
According to Dr. Dolgoff, parents don’t need to worry if little ones under 18 months use screens for video chats with loved ones like grandparents. But she adds an important distinction: “Content matters. Mindlessly scrolling through TikTok videos is not what we want children doing for hours each day.” Fortunately, children’s programming has expanded considerably since the parents of today were kids. YouTube Kids, PBS Kids, Netflix, Apple TV and other streaming services serve a variety of programs. Here are some healthy screen time choices, along with suggested time limits:- Toddler (2 to 3 years): Video call with grandparents and 30 minutes of educational programming such as Daniel Tiger’s Neighborhood or Sesame Street with parents watching
- Elementary school (6 to 10 years): Homework on Chromebook or other platform and 30 minutes of YouTube Kids, unstructured outside play and bedtime stories
- Teens (13 years and older): Homework time and no more than two hours of other screen use for gaming or socializing with friends
- “What do you think will happen next?”
- “How would you feel if that happened to you?”
- “Could this happen in real life?”
- “How would you have made this better?”
Sound screen habits begin with parents
Young children develop social and communication skills by observing, listening, talking (babbling counts!), reading, singing and playing with parents, siblings and others. The American Academy of Pediatrics advocates that parents put down their phones so they can focus on those activities and interactions. For help, parents can turn to apps designed to monitor their smartphone and tablet use. They can also examine their habits by asking themselves questions such as:- “Am I scrolling at the dinner table?”
- “Am I texting while driving?”
- “How much are my children watching me use my phone for entertainment?”
- “Am I setting a good example by having hobbies and interests that don’t involve screens?”
Experts advise ways to set and enforce limits
The American Academy of Child & Adolescent Psychiatry and the American Academy of Pediatrics understand the temptations of screens and parents’ difficulty setting limits. Some of their advice for parents:- Avoid using screens as pacifiers, babysitters or to stop tantrums.
- Create tech-free times, with extended breaks and tech-free zones, including the meal table.
- Learn about and use parental controls on devices, including phones, tablets, laptops and televisions.
- Make family outings technology-free—and that includes cameras.
- Remove screens from bedrooms 30 minutes to an hour before bedtime.
- Set a timer when using a device as a reminder to turn it off or put it away.
Tips for enforcing screen-time limits
It’s in children’s nature to resist when they don’t want to stop doing something pleasant or fun. It’s the parents’ job to stick to the limits they’ve set. Some more ideas for managing children’s reactions to screen-time limits include:- Have a designated “quiet spot” for younger children to calm down if they rage after time on a device is up.
- Offer alternatives after a device is turned off. Those could include playing a board game, reading a book together, playing with a favorite toy or creating an art project.
- Warn children before their time limit is up.
Resources for parents
- The American Academy of Child & Adolescent Psychiatry on screen time limits, music and music videos, video games, movie and video choice, and screen violence
- Common Sense Media
- Google and Apple content about online safety and parental controls
- Healthychildren.org, a website of the American Academy of Pediatrics
- know2protect, guidelines for protecting children online from the U.S. Department of Homeland Security

If you’ve had a stroke, you don’t have to replace flavorful cuisine with bland foods on your journey to recovery.
There are easy, delicious meal options that follow American Heart Association nutrition guidelines for lowering your risk of another stroke. More fiber, whole grains, fruit, vegetables and lean protein, with less trans fat, saturated fat, sodium and sugar are key to supporting your recovery efforts. Rehabilitation care teams and dietitians at Wellstar recommend keeping meals and snacks interesting with variety and new recipes like these.
Coconut Truffles satisfy your sweet tooth without any added sugar.
Ingredients:
12 medjool dates, pitted
2 tablespoons water
4 tablespoons unsweetened cocoa powder
½ cup puffed brown rice
½ cup shredded unsweetened dried coconut
Directions:
- Using a blender or food processor, puree dates and water until a sticky paste forms.
- Add cocoa powder and pulse until a solid dough forms.
- Stir in puffed brown rice.
- Using a small scoop, form mixture into 14 tablespoon size balls.
- Roll each ball in the shredded coconut for a light coating.
- Refrigerate for one hour.
- Enjoy!
Southwestern-Style Breakfast Casserole is a great way to start your morning.
Ingredients:
6 slices hearty whole-grain bread, cut into cubes
1 10-ounce package frozen chopped spinach, thawed and liquid squeezed out
1 7-ounce jar roasted red peppers, drained and chopped (or 1 red bell pepper, roasted and chopped)
1 ½ cups (6 ounces) Mexican-style cheese
3 cups non-fat milk
8 ounces egg substitute
1 teaspoon garlic powder
1 teaspoon cumin
½ teaspoon black pepper
½ teaspoon salt
Directions:
- Coat a 9 x 13 inch baking dish with non-stick cooking spray.
- Layer the bread in the bottom of the baking dish.
- Sprinkle evenly with the spinach, red peppers and cheese into baking dish.
- Combine the non-fat milk, egg substitute, garlic powder, cumin, black pepper and salt, then pour into baking dish.
- Cover and refrigerate at least four hours or overnight.
- Preheat oven to 350 degrees F.
- Bake, uncovered, for 45 minutes or until a knife inserted into the center comes out clean.
- Let stand 10 minutes before serving.
For more heart-healthy recipes, visit American Heart Association Recipes.
To learn more about how you can partner with Wellstar rehabilitation care teams to reduce your risk of another stroke, visit https://www.wellstar.org/medical-services/treatments-procedures/rehabilitation-services/neuro-rehabilitation..
;
Augusta University Health System (AUHS) has signed a letter of intent with Wellstar Health System to form an innovative new partnership that would expand Augusta University’s educational and research missions and allow Wellstar Health System to create a broader affiliation with the university’s Medical College of Georgia (MCG) as AUHS joins the Wellstar Health System.
The potential partnership is the culmination of a thoughtful and deliberate process begun in 2019 by AUHS, its governing board and Augusta University to strategically grow MCG while expanding and improving both patient care and Georgians’ access to health care services across the state.
The proposed partnership would innovate clinical care, training and research while adopting a successful model of bringing together community-based health systems and academic medical centers such as MCG and its teaching hospitals. MCG and Augusta University are part of the University System of Georgia (USG), and MCG serves as the only public medical school in the state.
“AUHS, Augusta University and the Wellstar Health System have a shared mission to solve Georgia’s health care challenges,” USG Chancellor Sonny Perdue said. “By joining forces and working together, we can leverage Wellstar’s clinical platform and leading-edge systems to support patients while providing more opportunities for students to learn, train and care for residents in local communities across Georgia.”
Pending a definitive agreement and regulatory approval, the partnership would focus on three strategic initiatives:
- Expanding digital health offerings to create more convenient access to care and provide more individualized care regardless of location.
- Growing the pipeline of physicians and other health care providers serving Georgia by increasing the number of students who train and conduct research through MCG.
- Developing new treatments, innovative care offerings and scalable care models to optimize the health and well-being of every patient.
“By bringing Augusta University Health System together with Wellstar Health System and leveraging our respective strengths, we would improve the health of the community, address social determinants of health and expand access to quality care for all Georgians,” said Candice L. Saunders, FACHE, president and chief executive officer of Wellstar Health System.
While there are aspects of the proposed partnership yet to be determined, the partnership would likely result in significant investments to improve existing healthcare facilities and to expand access to care across the state, including a new hospital and medical office buildings in Columbia County.
“Providing health care has never been as dynamic and complex as it is today, and this partnership with the Georgia-based, not-for-profit Wellstar Health System would enable us to extend our mission of improving health through excellence in patient care, education and research for the benefit of Georgians,” said Brooks A. Keel, PhD, acting chief executive officer of Augusta University Health System and president of Augusta University.
Through an expanded affiliation with the university’s Medical College of Georgia, the partnership would address the need to train more physicians and address a growing statewide shortage. With 60 percent of MCG graduates entering a primary care residency, training more physicians in these disciplines would support increased access to frontline care provided by specialists such as family medicine physicians and general pediatricians, especially in underserved areas of the state.
A new teaching campus in Atlanta at Wellstar Kennestone Hospital could also be established under the proposed partnership. As a result, MCG, which already has the ninth-largest freshman medical school class in the nation, would grow to become one of the largest public medical schools in the country.
“With our entire nation facing a physician shortage and our state typically ranking about 40th in the number of physicians per capita, educating the next generation of physicians is more critical than ever,” said David Hess, MD, dean of the Medical College of Georgia and executive vice president of medical affairs and integration at Augusta University. “I’m excited about the partnership with Wellstar, since it will enable our students and residents to continue to learn from some of the most highly qualified physicians and other health care professionals in the state while allowing MCG to expand its contributions to improving public health in Georgia especially in more rural regions.”

This article was originally published on Atlanta Business Chronicle on August 19, 2022.
Cancer is the second-leading cause of death in the United States, with more than 600,000 people dying of cancer in the country in 2021. While the U.S. death rate, or the percentage of people dying from cancer, is decreasing — partly due to fewer people smoking — the number of cancer deaths is going up due to our aging population. All these statistics are behind the call to decrease cancer deaths by 50% in the next 25 years. Atlanta Business Chronicle recently talked with a panel of experts from Wellstar Health System and the American Cancer Society, headquartered in Atlanta, about ways to accelerate cancer care progress through scientific research, patient care, partnerships, early detection, diversity and inclusion, and local care.* (Remarks edited for clarity and brevity.)
Panelists & moderator
Moderated by David Rubinger, market president and publisher, Atlanta Business Chronicle.
*Wellstar partners with Northwest Georgia Oncology Centers to provide world class cancer care close to home.
Research & treatment
David Rubinger: Where are we today in the world of scientific research? Are we in a good place in terms of research dollars?
Kimberly Jackson: I think we’re in a good place, but we can always be doing better and that’s a fact. There’s no other nongovernmental, nonprofit organization in the United States that’s focused on finding the cause and cures for cancer like the American Cancer Society. We’re committed to continuously funding the best new and ongoing projects at institutions across the country. For instance, right now in Georgia, we are currently funding eight research multi-year grants that are totaling more than $6.3 million. In addition to funding and conducting research, we are mobilizing our grassroot network advocates to increase the funding for cancer research. We’re primarily supporting those investigators that are early in their career, who are doing the most innovative cancer discovery research.
Rubinger: While the aging population is causing the cancer deaths to increase, the average death rate for the population has actually decreased. What do you attribute recent successes to and how will we continue to fight cancer deaths in the future?
Dr. Steve McCune: The mission of the Wellstar and Northwest Georgia Oncology Centers partnership is to help cancer patients live longer by providing innovative therapies in their local communities. What we have seen in the last 10 years has revolutionized the treatment of certain cancers, particularly lung cancer and melanoma, with immunotherapy and targeted therapies, oral drugs that address a gene mutation. What may be a good way to think of that is it’s the Achilles heel for certain cancers: they have one gene that drives their growth. And there are, because of the research that has occurred, typically one or more drugs that may specifically treat that mutation and block it so that it no longer encourages the growth of cancer cells.
Next-generation sequencing makes it very easy and fast to sequence 400 to 500 genes in a tumor from an individual patient, so that you know exactly any gene mutations in that particular tumor. It’s the most individualized medicine you could have. That’s the reality and that’s very accessible for many patients.
Rubinger: Nicole, from the nursing standpoint on the front line with patients, how has immunotherapy changed the relationship between the patient and the healthcare provider psychologically?
Nicole Centers: From the patient care perspective, it’s very clear that patients are more involved in their care. They want to have more say in their care. When we can educate patients appropriately up front about all of their different options and their care along with their providers, they feel like they have more control. We know when patients feel more in control of their care, they’re more compliant to the plan of care. When it comes to immunotherapy and monoclonal antibodies that are given, they’re generally tolerated far better than chemotherapies of the past. That doesn’t mean everything can be treated with an immunotherapy or monoclonal antibody. However, when we have more options to give patients that they can tolerate better, then it kind of alleviates all of those nightmares of, “This is a horrific journey,” and, “It’s not going to work for me.” Overall, we have medicines that work with your body to fight the cancer in ways that we just haven’t had before.
Patient care & partnerships
Rubinger: The cancer “moonshot" is a term that excited everyone. Have you seen the concept of patient care change from when you first got into the field to where it is today?
McCune: I think it’s dramatically different. In some ways the moon shot has already happened and I'll explain what I mean by that.
Immunotherapy revolutionized the treatment of cancer. If you have a chemotherapy that kills 99% of cancer cells, well that means eventually that 1% keeps coming back. Immunotherapy can work for years, even after the actual immunotherapy has stopped. It’s not a vaccine, but it works in much the same way that a person’s own immune system actually can control or eliminate the cancer. I think that, in a sense, was the biggest game changer for the way that people were treated.
I started doing this about 20 years ago. And so most things that we treated were chemotherapy, very few things that were actually what we would have called targeted therapy or intelligently designed targeted therapy. The first drug was really coming out at that time called Gleevec, which treated CML (chronic myeloid leukemia.) I treated patients before that era who had to have a bone marrow transplant or they were basically going to die of CML. And now we think of CML as a condition that’s almost 100% survivable. We have eight different medicines that are commercially available for treating CML. It’s totally changed the future for some patients who would have had very poor outcomes otherwise.
Melanoma used to be very difficult to treat. Chemotherapy didn't work well. A treatment called Interleukin-2 worked for about 8% of patients and no one really knew why. It basically is an early immunotherapy but with a lot of toxicity. Now you have drugs like Opdivo, Yervoy, Keytruda, which are really the standard of care. Chemotherapy is rarely, if ever, used for melanoma.
There are antibody drug conjugates — something that basically has a payload on the monoclonal antibody, so it homes in on certain proteins on the outside of different cancer cells. That’s a way of delivering a toxin directly to the cancer cells with less impact on normal tissues.
There are companies all over the United States, from large to small, that are really driving the innovation in targeted therapies, antibody drug conjugates, so it’s an exciting time in oncology.
Wellstar has participated in trials for 15 years. In just the last three years, we have participated in cancer trials resulting in over 20 FDA approvals for either new medicines or new combinations of medicines. Usually, it is four to five years before something is FDA-approved. Now not everything’s approved, not everything works better, but it gives people hope and it gives them the chance to have cutting-edge therapies in their local communities.
Rubinger: Nicole, how have advances like these changed the psychology of talking with a patient with a cancer diagnosis?
Centers: I think it has changed. When I started in this field 20 years ago, we would say “the breast cancer down the hall" or “this is the breast cancer treatment.” Now we say, “the patient with breast cancer,” “the patient with lung cancer,” and we treat it as an illness that is part of the whole person, versus the whole person being the illness. That’s a different way that we think about things and that’s how we approach our patients differently when it comes to nursing.
There’s a very unique field inside of nursing called navigation. And one of the things that moonshot really promoted was something that we've been out here doing for a pretty good while, but it brought it to the center stage for all Americans to hear this word called a navigator. It meant someone that was going to guide you on your cancer journey. Several years ago, there was just one kind of navigator and they tried to do the whole care path, but we at Wellstar recognize that there’s lots of pieces to people who could have cancer, people who are being tested for cancer, and those patients that actually have cancer. So we have screening navigators, we have diagnostic navigators, and we have actual care trajectory navigators, which are oncology nurse navigators. We have over 15 of those in our system and some of those specialize by tumor type and some of those are more generalized.
What they do is they actually bring the whole person into view during their care. It means if you have childcare or if you have your parents, that you're taking care of first, or that transportation is an issue, these navigators work with you and your provider as well as your payers, whether it’s insurance or if you don't have insurance, we try and get you on insurance — to be sure that those things that would affect your compliance to the plan of care, they're helping you resolve.
It’s great if you can come in for your treatment. But if your dog has to be walked at two o'clock every single day and your treatment starts at noon, then we need to help you get a dog walker. We need to help you link to resources. For years there have been resources out there that patients didn't even know to utilize. And so organizations have this money that’s sitting there trying to help patients, but no one to link them to it. Navigators link patients to community resources, to national resources. The American Cancer Society has this really great program that will offer patients free rides to go get their cancer care, and most patients don't even know about that. But you talk to the navigator and they're like, “Wait, I have them on speed dial” because they get to know what those resources are, and they can help patients keep their appointments and keep a total life balance.
When we look at that, what that does is it makes their care more effective because they're more compliant to the plan of care.
The other thing navigators do is to help timeliness of care. So if two providers talk and say “we're both going to go see Sally Sue,” or whoever your patient is, and they turn to the front desk and say, “be sure we get this patient on the schedule.” However, the front office staff may not be aware the appointment doesn't meet the latest benchmark for timely care. So what a nurse navigator does is say, “Wait, we have some timeliness to care parameters that we know are best practice.” And they work with that provider or that office to help expedite those appointments.
The best part of navigation is it really brought care back into the patient’s community. Patients didn't understand what was available to them in their community. They thought you had to go to an academic center in a large city that cost them lots of money because they had to stay in hotels or take a flight or go get a car, because there’s so many patients in the states that don't have valid transportation that can take them two hours away. Navigators help patients understand what’s available in their community and the care that they can receive. They can also link them to clinical trials, arrange for assisted lodging and help patients get the best care out there to survive their cancer.
We've also seen an uptick in clinical trials because the navigators say, “Do you remember when your doctor talked to you about clinical trials? Do we want to circle back on that? And do you want to go talk to your doctor again?" They're reinforcing that education.
Second opinions & local care
Rubinger: Let’s move to another topic: the second opinion. The second opinion might be local, but if you have the resources, it might be at Sloan Kettering, MD Anderson or Mayo. Is there less of that going on today because local providers are able to provide that level of confidence in what the care is going to be? Twenty years ago you would have maybe run to Houston.
McCune: I think people still do, but maybe for a different reason. I think they have more information and more knowledge and they're not just running to Houston, they're running to a specialist in Houston or New York or Atlanta. I say, “Hey, you're not stepping on my toes. I want you to get a second opinion. I can help you get that, more than just a cold phone call. Let me try to get you to the right person.”
At Wellstar, we do have Mayo Clinic Care Network e-consults available. That’s a pretty easy way to get a quick question answered if we need a specific answer or a second opinion without someone having to travel somewhere.
In addition to second opinions, we believe in collaborative care. We have groups of cancer experts who diagnose and plan treatments together in tumor boards so patients have the best outcomes. In Specialty Teams & Treatments (STAT) Clinics, multiple cancer specialists meet with the patients and their families in one place on one day to help them get questions answered. This helps them start treatment faster so they have better outcomes.
Centers: At Wellstar, 300 cancer specialists in our network can collaborate with each other. When they do request second opinion e-consults from the Mayo Clinic, it is free to patients which is a really nice thing because they usually have to pay for second opinions.
Rubinger: Kimberly, when I think of the Cancer Society, I think of the research dollars going to help cure cancer. But as we were talking earlier about how it helps with driving patients to treatment, the society’s partnerships with a Wellstar or other healthcare systems may be less well known. Can you address that?
Jackson: Collaboration is absolutely critical. So many cancer patients and their families are facing barriers and challenges that are too complex for just one organization to address on its own. To help overcome those barriers, we unite organizations in partnership to improve the lives of people facing cancer.
One example, we have Hope Lodges all over the country where individuals and a family member are able to stay for free and they're wonderful. It’s a great resource for our patients and their families.
Another example is we partner with Wellstar and other health systems in Georgia to provide those transportation grants that Nicole talked about and service to people who need it the most.
For some people with cancer, transportation is a challenge and it creates that barrier to receiving the treatment that they need. Many of them need daily or weekly treatment and often over the course of several months and the need was particularly pronounced during the pandemic. We were able to provide funding to 251 health systems across the country to alleviate that financial burden of transportation.
Another way we mobilize the cancer community on both the national and the local level is through our mission-critical roundtables. We're providing organizational leadership and expert support to multi-organizational roundtables focused on breast, cervical, colorectal and lung cancer, HPV vaccination and patient navigation. Each roundtable has a shared vision to support people to prevent and support and survive cancer. It’s a proven model close to home. Wellstar Health System was a key partner in launching our Georgia Lung Cancer Roundtable, whose primary goal is to improve screening rates and lung cancer outcomes.
Rubinger: Our society has come a long way in terms of reducing smoking. What are the trends in lung cancer that you're seeing? Does it primarily impact your older patients or is it across the age spectrum?
McCune: It can be any age and certainly there are people who are non-smokers who are much more likely to have a lung cancer that is driven by a single gene mutation and those are usually treatable with targeted therapy, which is typically an oral drug. So, in one sense, lung cancer is a disease of people who have smoked for a long time, 30 or 40 years. But it’s also a disease of nonsmokers. I do think people are generally smoking less. I remember people used to smoke in the pediatrician’s office when I was little. Things have changed dramatically.
There is a very active lung cancer screening program at Wellstar through the thoracic surgeons and the pulmonary physicians. It looks at people who have had some smoking history, who are typically at more risk for developing lung cancer. They'll have a low-dose screening CT scan, and we do see a number of lung cancers get discovered earlier. That’s a worthwhile initiative when something is surgically curable, as opposed to it’s gotten so advanced that people are having symptoms.
The pandemic impact – screenings & DEI
Rubinger: During the pandemic, I didn't see my doctors as often. None of us did. It was harder to access healthcare the way we did before. What has that done?
Centers: The pandemic did change us. A lot of screening procedures at the beginning of the pandemic were paused, but we were still able to quickly to return to those services. But the temporary delay made some patients think that screening wasn't as important as it once was. We really worked hard to get the message out there about the importance of early detection.
We use a lot of automated tools like our lung nodule software to help us identify nodules in patients who come into our system for other reasons and have those incidental findings. We also work with our church network here at Wellstar. We work with BLKHLTH in Atlanta, and there’s lots of healthcare organizations that are reaching out to their communities to get people back to screening.
We at Wellstar have made a very concerted effort to go back out and say, “We have kit testing that you don't have to come into the hospital to have done. You can do that at home. Let us help you get the kits.” We reopened our screening mammography centers with all the safety protocols in place. And then we called the patients and said, “Hey, you missed your cancer screening.”
We did see an initial dip because if you're not screening, you're not finding it, as cancer usually doesn't hurt. So most people don't know that there’s something in there growing. Now we're seeing patients come in with later stages, or more advanced tumors than we traditionally would have seen. That’s because of the lag in screening.
Rubinger: Kimberly, is this consistent with what you've been seeing?
Jackson: Yes it is. Early during the pandemic, cancer screening rates decreased dramatically and an estimated 35% of Americans missed routine cancer screening due to Covid-19-related fears and care disruptions when many facilities reduced or suspended services. Screening rates remain below historical averages. In addition to the coronavirus, top barriers to screening are that individuals have no symptoms, procrastination, lack of recommendation, cost, and no insurance. During the pandemic we worked with healthcare systems to address the issue as part of the “Get Screened” initiative. Through donor support, we were able to provide $2.2 million in grant funding to 77 health partners to implement quality improvement strategies to rapidly increase cancer screening rates and reduce the barriers that have been exacerbated through the pandemic. Wellstar was one of our partnering health systems in the Get Screened initiative. They were able to increase their breast cancer screening rate by 6.8 percentage points, which resulted in over 44,000 people in Georgia being up to date with their breast cancer screenings.
Rubinger: One of the crises in our society is the ability that people have to access care. When you think about those things from the DE&I perspective, where do we see the biggest challenges and where are the biggest opportunities?
Jackson: While the pandemic is shining a light on the issue, the reality is if we were focusing on having more diverse physicians, nurses, etcetera, if we were focused more on removing the barriers and investing more, we would have fewer people who are getting diagnosed at later stages, or, you know, unfortunately losing their lives to cancer. That’s a fact. There’s an opportunity right now that we cannot shy away from. The evidence is there to show the tie between the impact on an entire community by ensuring equitable health for all by focusing on the ones that need the most is actually equalizing and improving the health of the community itself.
Rubinger: I'm curious what role can the employer play?
Jackson: The employer, they have team members and staff that make up the community that we're seeking to serve. So what they can do immediately is educate the employees on the resources that are available on the prevention side. They can also make prevention a priority and establish norms of only offering healthy snacks, for example.
As well, they can encourage employees to go to their doctors, and also for the top leaders to serve on these boards and these councils of the hospitals and organizations like the American Cancer Society, to be aware and to stay ahead of the issues and to be informed and proactive about helping the community.
Centers: There’s really three ways to look at equitable care, and it’s not a one-path journey. First off, there’s a screening environment and the diagnostic environment, getting people to the services where they are and getting them access to care.
The second part is a mistrust of the healthcare system, which is ingrained in many of our societies across the U.S., so educating them to the safety parameters we have in place to ensure that all patients have equal access to care.
The third component is to teach our healthcare providers, be they nurses, medical assistants, physicians, about diversity and the things that happen to patients who maybe don't look like you, that walk through the door. What we know is, especially among our patients of color, that when they come in, sometimes their complaints aren't taken as seriously as others. We see that in the national studies.
What we have to do is educate our providers and our healthcare workers, but also educate our patients to say “you are your own best advocate.” If you go to a doctor and you're not getting the care that you think that you need or you deserve, then you can go to another place or else you can reach out to your patient advocates at the facility that you're going to. At Wellstar, we have invested a lot of time and energy into educating all staff so that all patients who walk through the door regardless of their social standing, regardless of what they look like, regardless of their history, are all treated equitably, and we do our best.
Rubinger: Dr. McCune, anything to add on that topic?
McCune: Yes. We have a diverse group of research coordinators, both African-American and native Spanish-speaking, so I do think there are opportunities to narrow some of those health gaps. I will say the pandemic across the board affected clinical trial enrollment, because there are typically more procedures like more CT scans that a person has to go through to go on a clinical trial, than just receive what we would call standard of care therapy. So across the board, that is something that has reduced clinical trial participation and that is starting to come back.
But I do think you have to meet people where they are. We obviously have a health system that covers some urban to rural areas in Georgia. One of the things that we're able to do is take clinical trials to people who are as far west as Carrollton, as far north as Cartersville, or closer to the Atlanta area in Marietta, Austell and Douglasville. We're expanding that research network as well.
Not everybody can drive two hours. Not everybody has a family member who can drive them when they're too sick. Access to care is a huge list of things that don't sound like much but a ride to the doctor’s office, a ride to a CT scan is the difference between someone getting care or not getting care. It’s things that seem little but are really not.
When you were talking about what can corporations do, I'll just say, it seems like most people’s experience is very dependent on whether the human resources person is nice to them. From the patient’s point of view, either “they're working with me and I can show up,” or “if I have a bad day, I can just stay home,” or “they fired me yesterday.” So maybe just a little bit of grace there. People have their federally mandated leave but they need more than that. They need a little attitude of caring or just going the extra mile, to help somebody get through their cancer treatment. They'll probably be a better employee and grateful if you treat them nicely.
;
If you’re a MyChart user, E-visits are a convenient way for you to receive care from a Wellstar clinician without needing to schedule an appointment or come to the clinic.
In addition to virtual visits and our Virtual Urgent Care, Wellstar has expanded access to care with E-visits. These visits are completed using our secure patient portal and offer treatment for non-emergency conditions.
Here’s how it works
Through MyChart, tell us about your health concern by answering a few questions about yourself and your symptoms, then a primary care clinician will respond in MyChart with your care plan.
Conditions that can be treated with an E-visit include:
- cough
- sinus problems
- urinary tract infection
- conjunctivitis
- back pain
- diarrhea
- vaginal discharge
- heartburn
How to start your E-visit
Log on to MyChart and click Symptom Checker from the menu in the top left of the screen. Select your condition and confirm you are currently located in Georgia. We’ll ask for information about your medications, allergies, health history and preferred pharmacy so that our team can tailor care specifically for you. Next you’ll see the estimated cost for your visit. Finally, click Submit to contact our care team. One of our providers will follow up with your care plan.
“A Wellstar primary care provider will review the information about your symptoms and health history, and we’ll create a customized care plan just for you,” said Wellstar Primary Care Physician Dr. Monika Karakattu. “E-visits offer the same personalized care you’d receive in person at Wellstar, conveniently delivered online and on your schedule.”
Learn more about getting care with an E-visit.
If you don’t have MyChart, you can make an account online if you are an established Wellstar patient. With MyChart, you can securely access all your health records with a single username and password. Once you’re connected, you can view your test results, schedule appointments, request prescription refills and pay your bills.
Not a Wellstar patient yet? Find a primary care clinician here.

If you test positive for COVID-19 and are experiencing mild to moderate symptoms, your Wellstar care team can help you get back to feeling better with Paxlovid.
Paxlovid is an antiviral medication that can be prescribed to patients who are 12 or older and weigh at least 88 pounds. It’s best to start the medication as soon as possible, and you must begin taking it within five days of your first symptoms. Paxlovid is a pill you can take at home.
Read the U.S. Food and Drug Administration’s fact sheet about Paxlovid.
Where to get care
If you are feeling sick, you have several options for care. Learn more about the types of care available at Wellstar and what is right for your health needs.
If you have tested positive for COVID-19 with a home test and have mild symptoms, you can speak with a clinician using our 24/7 Virtual Urgent Care. They will evaluate your symptoms and work with you on a personalized care plan, including a prescription for Paxlovid if appropriate.
Patients who have tested positive with a home test can also call their Wellstar primary care clinician about a Paxlovid prescription or visit a retail pharmacy to be assessed by a pharmacist.
Wellstar retail pharmacies and many other pharmacy locations can fill Paxlovid prescriptions. Your Wellstar care team can send your prescription to your local pharmacy.
Find a location that offers COVID-19 testing and treatment. At these locations, patients are either tested on site or can bring in a positive test result from another testing site or an at-home test. Eligible patients will receive a prescription and can have that prescription filled on site.
Getting vaccinated
As new variants of COVID-19 emerge, it’s important to remain vigilant. You can do your part to “stick it to COVID” and keep yourself and the community safe by getting vaccinated. The COVID-19 vaccine is available at a Georgia Department of Public Health location or your local retail pharmacy. Find a vaccination site near you.

Ortho-On-Demand
Sports injuries, broken bones and sprains don’t have to interfere with your schedule—Wellstar Ortho-on-Demand at 1220 West Wheeler Parkway in Augusta has you covered with convenient care when you need it. Our expert team provides prompt treatment for people ages 8 and older for musculoskeletal injuries, including:
- Immediate orthopedics specialty care
- X-rays to assess fractures and breaks
- Bone, joint or muscle injuries
- Ankle sprains or strains
- Knee sprains or strains
- Hand, elbow, wrist or shoulder injuries
- Broken bones without an open wound
- Splinting, casting and bracing by specialty clinicians
- New back pain
We welcome walk-ins and offer same-day appointments for fast, efficient care. Learn more about Ortho-On-Demand.
Urgent Care
If you’re dealing with a minor injury or need care after your physician’s regular office hours, going to urgent care is often the right choice. Wellstar Urgent Care Centers provide quick, convenient care for non-emergency medical conditions.
We also offer Virtual Urgent Care, which provides virtual health visits for minor medical concerns from the comfort and convenience of home.
Wellstar Urgent Care provides:
- Care for minor injuries, such as sprains and broken bones
- Treatment for medical issues like bites, burns and cuts
- Lab and X-rays
- Sports physicals
- Occupational health services
- Worker’s compensation services
Wellstar Urgent Care has locations in Evans, Grovetown and South Augusta, or you can use our Virtual Urgent Care.
Emergency Care
In a life-threatening medical emergency, every second counts. Never put off getting the proper care when lives are on the line. Remember, driving yourself to the Emergency Department (ED) may delay care, so call 911 for the fastest access to emergency care.
When the unexpected happens, Wellstar MCG Health Medical Center’s Emergency Department is always ready. Our trained team provides expert emergency care 24 hours a day for people of all ages. At Wellstar Children’s Hospital of Georgia, the dedicated Pediatric Emergency Department team is specially trained in treating children.
Recognize the signs of a medical emergency:
- Fainting or loss of consciousness
- Sudden, severe pain
- Uncontrolled or severe bleeding
- Choking, coughing up blood or severe vomiting
- Changes in mental status, such as confusion or unusual behavior
- Traumatic injury due to a motor vehicle or other accidents
- Broken bones with an open wound
Remember, call 911 right away in a medical emergency. That way, care can begin sooner during the crucial time it takes to be transported to the hospital.
Some conditions, such as sports concussions or gout, may be best treated by a primary care or orthopedics clinician. Our Ortho-On-Demand team can refer you to other Wellstar locations if needed.
;
- CyberKnife, a non-invasive robotic system that focuses radiation treatment with precision
- STAT Clinics, where specialists collaborate on one day to evaluate a patient and plan cancer treatment
- Nurse navigators to guide patients to resources at Wellstar and in the community
- Expanded inpatient capacity and distinctive surgical specialties
CyberKnife targets hard-to-treat tumors
Wellstar North Fulton was the second Wellstar location to receive a CyberKnife system. CyberKnife precisely targets cancerous and non-cancerous tumors. This minimizes damage to healthy tissue around tumors. CyberKnife allows radiation oncologists to deliver “very high doses of radiation at a very small target,” said Dr. Mark McLaughlin, a radiation oncologist. This type of precise treatment is called radiosurgery. Patients treated with CyberKnife typically have shorter treatment spans. For example, breast cancer patients undergoing conventional radiation might have four to six weeks of treatment, five days a week. With CyberKnife, patients may complete their treatment in just five days. According to Dr. McLaughlin, another CyberKnife advantage is the machine’s ability to deliver targeted treatment even when a patient moves. “For example, if a patient has breast cancer, she’ll be breathing during treatment. She has to breathe, of course, but with breathing, the tumor volume or target volume is constantly changing. The CyberKnife allows us to track and move the machine (to target the tumor) in real time,” he said.Providers collaborate to diagnose and begin treatment without delay
Wellstar North Fulton also has STAT Clinics, which stands for Specialty Teams and Treatments, for many types of cancer, including breast, head and neck, brain and spine, and lung. Dr. Pearson described STAT Clinics as a “one-stop shop where patients meet all the people who will be part of the cancer team in one day: surgeons, radiation oncologists, medical oncologists, potentially plastic surgeons and genetics experts, if that’s appropriate.” Patients and their families appreciate not making multiple trips or trying to piece together a treatment plan. They’re also comforted to see the communication among everyone involved in their care, she noted.Cancer nurse navigators map the road to treatment and recovery
A cancer diagnosis can leave patients and their families feeling shocked, scared and unsure of where to turn. Nurse navigators help patients get their bearings by:- Answering questions about treatment and scheduling appointments
- Connecting patients and families to community resources for transportation, nutrition, financial support and more
- Helping with insurance questions
- Providing emotional support during a difficult time
Distinctive specialties and expanded inpatient capacity
Wellstar North Fulton has added beds for post-surgical cancer patients who need an overnight hospital stay. The medical center’s intensive care unit (ICU) is also tailored to care for cancer patients’ needs. “For our more complicated cases, like colorectal or prostate patients, it allows us to make sure we have the space and the resources for them to get the care they need while they’re recovering,” Dr. Pearson said. “Neurosurgery has expanded its footprint too. We not only treat brain tumors, but we also do a lot of vascular and neurovascular procedures,” Dr. McLaughlin said. “We’re doing some very high-tech things.” Added Dr. Pearson: “I’m so proud of how we’ve brought this all to the North Fulton community. Patients don’t have to feel like they have to leave the area to get the expert care they need.” Learn more about Wellstar North Fulton Cancer Center.;
When it comes to getting high-quality care for your heart, you can count on Wellstar.
Because we know heart health is an essential part of overall wellness, we offer leading expertise, innovative treatments and compassionate care to protect your cardiovascular health.
From heart attacks and rehabilitation to cardiac surgery and psychological support, your heart is in expert hands at Wellstar.
High-tech heart treatments
With the largest network of certified Emergency Cardiac Care Centers (ECCC) in Georgia, Wellstar ensures world-class heart care is never far away.
Our cardiovascular experts are ready to treat patients at the first signs of a heart attack. We use high-tech equipment—including electrocardiograms (EKG), chest X-rays and cardiac catheterization—to diagnose heart attacks quickly.
Getting the right care can minimize or even prevent heart damage. That’s why Wellstar relies on the most advanced treatments, such as Shockwave technology, medicines and life-saving cardiac surgery, to effectively prevent and treat heart attacks as fast as possible.
Wellstar Kennestone Regional Medical Center has a cardiac hybrid operating room, bringing a catheterization lab and surgery suite together in one place. With catheter-based procedures, our interventional cardiologists can provide expert, minimally invasive heart attack care.
We also perform structural heart procedures, including valve repairs and replacements, along with cardiac surgery and electrophysiology procedures that can determine the cause of heart rhythm problems.
At Wellstar, we don’t just treat heart conditions when they happen. Our providers also offer world-class preventative care, helping people like Latoya Jordan catch chronic conditions—such as high blood pressure—at the very start.
The Wellstar Comprehensive Aortic Program provides treatment for people with emergency and non-emergency diseases of the aorta. We offer cutting-edge procedures and devices to diagnose, monitor and repair all types of aneurysms. From screening to treatment, our team uses a coordinated approach to care which includes comprehensive diagnostic testing. When urgent care is warranted, we can treat aortic emergencies quickly.
Care that never skips a beat
If an on-going heart condition, such as atrial fibrillation (AFib), is keeping you down, Wellstar has a team of experts who can help.
When Frank Ryan’s heart had trouble keeping pace and kept him from playing the tuba, he felt off-beat in everyday life. After getting specialized care at Wellstar, he’s back in the band again.
Wellstar Cardiac Electrophysiologist Dr. Narendra Kanuru shared state-of-the-art treatments available for heart rhythm disorders.
“Along with advanced medical therapies, we have numerous interventional or surgical therapies, including pacemakers, defibrillators and other advanced cardiac devices as well as cardiac catheter ablation,” Dr. Kanuru said.
Cardiac catheter ablation is a non-surgical procedure available at Wellstar that helps restore a regular heart rhythm by blocking abnormal electrical signals.
With the latest advances in electrophysiology at Wellstar, we’re keeping hearts going strong.
Hope for heart failure
Wellstar also provides expert care for people with congestive heart failure like Bow Matthews. The husband and father-of-two found support from our Heart Failure Academy and learned how to take care of his well-being for the long haul.
To help prevent heart failure flare-ups, Wellstar offers a remote heart monitoring technology that provides real-time health information to our providers.
“With heart failure, as with all health issues, it’s best to take preventative action and stop problems from occurring,” said Dr. Hans Lee, medical director for the Wellstar congestive heart failure program. “Monitoring your heart health and staying in touch with your cardiologist can help keep you out of the hospital and keep your heart in shape.”
For those whose hearts need extra assistance like Mike Clements, a left ventricular assistance device (LVAD) can be a game-changer. An LVAD is a battery-powered pump that is surgically implanted to help the heart more effectively pump blood.
"An LVAD gives patients with severe heart failure the opportunity to get their lives back,” said Dr. Brian Howard, medical director of the advanced heart failure and LVAD program at Wellstar Kennestone. “These life-saving devices are powerful enough to take over for the failing heart. They allow patients to enjoy life with their loved ones as they await a heart transplant, and in some cases, they even serve as an alternate to a heart transplant entirely.”
At the Heart Failure Clinic at Wellstar Cobb Medical Center and the Advanced Heart Failure Program at Wellstar Kennestone, trained experts provide specialized care for those with heart failure and LVAD implants, helping to improve quality of life.
After Mike received his LVAD implant, he was able to walk his daughter down the aisle at her wedding. Thanks to advanced technology available at Wellstar, patients with heart failure can keep doing what matters most.
Specialized support services
Wellstar has dedicated resources to help people with cardiac conditions find support.
Following a medical event like a heart attack or other serious cardiac problem, Wellstar offers cardiac rehabilitation to get people back on track.
Cardiac rehabilitation is a medically monitored program that provides education, support and lifestyle modifications. Our team helps you learn heart-healthy behaviors and lower your risk for future heart issues.
However, we understand health journeys aren’t just about physical healing. Dealing with heart issues can also cause many difficult mental health challenges, including anxiety and depression.
“At Wellstar, we wanted to build out a program just for our cardiovascular patients because behavioral health and cardiac health are really closely connected,” said Dr. Shawn Coyne, Wellstar director of health psychology and cardiac psychologist. “In fact, cardiac patients are three times more likely to be depressed than the general population.”
After living with three chronic heart conditions for years, John Petrick found solace in meeting with a Wellstar cardiac psychologist. Now, he’s learned new coping skills and how to prioritize his mental well-being.
With support services at the ready, patients with complex conditions can better understand themselves and their overall health.
Care to keep your heart healthy
No matter what your cardiovascular concerns may be, Wellstar is dedicated to helping people with heart conditions live life to the fullest.
Learn more about how Wellstar is protecting heart health in Georgia, and how you can take control of your cardiovascular health.

Many men are reluctant to seek diagnosis and treatment of prostate cancer because they fear the effects of treatment on their urinary and sexual function. Enter modern technology. MRI scans, PET scans and molecular testing of blood and tissue samples not only help physicians know how and where to treat, but also identify those who may not need any treatment.
Having a PSA blood test is usually the first step in detecting prostate cancer. Now, modern MRI scans can help the urologist target abnormal areas for biopsy, like how a GPS pinpoints a destination. With this technique, patients can be more confident that the biopsy samples accurately represent their condition. In fact, this confidence has allowed men with slow-growing forms of prostate cancer to observe their condition rather than immediately pursue treatment. Since the formation of cancer cells all starts with changes in a cell’s genetic material, specialized testing of the biopsy sample can help further define the behavior of an individual’s prostate cancer.
When treatment for prostate cancer is needed, the latest methods bring next-level precision to protect the delicate nerves and muscles surrounding the prostate. Now in its second decade as a standard treatment for prostate cancer, robotic prostate removal continues to break barriers with new instrumentation, refined techniques and artificial intelligence. Not only do these advancements speed up recovery, but they also facilitate less traumatic access to spaces that were previously very difficult to reach. Similarly, the latest radiation therapy techniques allow delivery of a thin beam to the prostate.
For more aggressive forms of prostate cancer, the latest type of PET scan can identify the cancer in other locations. First, a radiotracer (slightly radioactive substance) is injected into a vein, and it binds to prostate cancer cells, wherever they may be hiding. Then the resulting X-ray images are superimposed onto a CT scan to highlight any areas of suspicion. We can now attach medications to this radiotracer to attack and kill remote prostate cancer cells like a guided missile.
With these recent advancements in technology, the management of prostate cancer continues to be more effective and gentler for the modern man. One can only imagine what’s on the horizon.
Learn how to support a loved one through their prostate cancer diagnosis.

This article was originally published on Atlanta Business Chronicle on April 12, 2024.
Orthopedic care has evolved from injury treatment and corrective surgery into a critical component of modern healthcare. As primary care remains foundational in managing overall health, the demand for orthopedic services has surged, reflecting changing lifestyles, demographics and expectations. In any given year, 12% to 14% of the adult population will visit their physician for back pain, according to the United States Bone and Joint Initiative (USBJI).
Against this backdrop of widespread musculoskeletal issues, Wellstar recently convened with the Atlanta Business Chronicle for a panel discussion to delve into the changing landscape of orthopedic care. This insightful forum explored key trends, challenges and innovations shaping the field, with leading healthcare professionals offering valuable perspectives. These discussions unraveled the complexities of orthopedic care, ranging from preventive strategies to cutting-edge treatments. Among the panelists was Steve Quehl, a former college football player for Notre Dame, who started as a tight end before transitioning to a center. Other panelists were Dr. Hodari Brooks, orthopedic surgeon, Wellstar Health System; Dr. Joseph Burns, chief musculoskeletal officer, Wellstar Health System; Dr. Timothy Oswald, pediatric orthopedic surgeon, Wellstar Pediatric Orthopedics. Moderator was David Rubinger, market president and publisher, Atlanta Business Chronicle.
The rise of orthopedics and interventions
David Rubinger: There’s an uptick in the demand for orthopedic services and these specialists have become increasingly essential to healthcare. What societal changes drive this heightened need for specialized ortho care?
Dr. Joseph Burns: We’re facing an aging population alongside a growing desire for an active, pain-free lifestyle. In the past, individuals had to endure their limitations and pain for life. Today, people have more options. Technology, techniques and training advancements now provide surgical alternatives that significantly enhance quality of life well beyond middle age.
Wellstar conducts numerous community campaigns through various channels, including community events, the media and in our offices and hospitals, highlighting the value of maintaining health and establishing a relationship with a primary care physician.
Dr. Hodari Brooks: Societal changes for both our youth as well as adults have resulted in the increased need for orthopedic care. Physical activity has decreased, with fewer kids participating in physical education. This leads to more injuries related to obesity and lack of activity. The need for joint replacements is soaring, driven by both baby boomers aging and younger individuals seeking treatment earlier. Half of my practice is caring for patients under 55, a shift from when people would wait years for treatment. Now, we prioritize improving quality of life sooner rather than later.
Patients, including those seeking joint replacements, are opting for earlier interventions. They are less inclined to wait for treatment, indicating a shift within the healthcare system towards promptly addressing patient needs.
Rubinger: What new injury trends are emerging in sports due to changing physical activity patterns, especially with the rise of extreme sports and diverse workout routines?
Dr. Burns: The rise in overuse injuries among our younger population is disheartening. Young athletes don’t diversify their sports as they once did, leading to year-round specialization and an increased risk of injury. This relentless pursuit of success often comes at the cost of rest and diversity in physical activities.
We’re also encountering complex medical issues that require specialized treatment, reflecting both advancements in medical care and the aging population’s evolving healthcare needs. Conditions once considered untreatable are now within our reach, marking a significant shift in the scope of orthopedic care over the years.
Rubinger: Dr. Oswald, as a pediatric orthopedic specialist, have you frequently observed the concept of subspecialization and the decline in diversification among young athletes?
Dr. Timothy Oswald: It’s a significant area of concern for us, and we’re conducting more research. Recent studies have highlighted the insufficient breaks and rest periods given to children, as well as the trend of starting high-level athletics too young, which aligns with the issue of subspecialization. Kids are not miniature adults. Their orthopedic stresses differ due to growth plates and differing stress responses.
We’re educating the community, including coaches and parents, about the importance of rest periods during training through channels like social media. We aim to implement better training methods so young athletes can continue playing into their college years, as we’re noticing a concerning trend where many high-level athletes quit sports as early as eighth grade.
Rubinger: Steve, as a former college athlete yourself, what’s your observation of the sports world’s changes regarding how injuries are approached, especially compared to when we were younger?
Steve Quehl: I view this issue through the lens of my grandchildren and their friends, and I agree with the insights shared by these doctors. Their perspectives must influence parents’ decisions, particularly regarding the early specialization trend. Parents often have unrealistic expectations of their children becoming professional athletes, which can lead to overtraining and injuries. Kids should have a balanced approach to sports. I’m grateful my daughters chose activities like swimming over contact sports for their children, considering the risks to growing bones and muscles.
Prior to my enrollment at Notre Dame, I appreciated the joy of playing multiple sports during each season for fun, without the pressure of turning it into a professional pursuit.
Efficient outpatient care benefits
Rubinger: I’ve noticed remarkable changes in my lifetime regarding the duration of procedures and the efficiency of hospital stays or visits to outpatient surgery centers. I’m curious about your perspective on this shift away from extended hospital stays. Do you believe it’s ultimately beneficial or detrimental to patients? What are your thoughts on this evolution of the time spent in hospitals or surgery centers?
Dr. Brooks: There’s been a significant shift in the duration of hospital stays, especially concerning joint procedures. In the past, patients would typically spend several days in the hospital before and after surgery. In my practice, around 90% of primary joint patients can return home the same day, which is remarkable. This change is not only due to patient preferences for quicker recovery but also has medical benefits, such as reducing the risk of infection. Outpatient joint replacement is not done everywhere, however, and it is important to discuss this option with your individual surgeon.
Insurance companies have started incentivizing shorter hospital stays. While this trend has clear advantages, it also comes with challenges, such as pressure to discharge patients quickly. The ability to expedite recovery and minimize specific complications is a positive development I believe will continue.
Rubinger: Do we have data showing a decrease in complications due to the trend of shorter hospital stays, particularly for joint procedures?
Dr. Burns: Evidence indicates improved outcomes for outpatient procedures, with data supporting this trend. The shift involves a comprehensive approach beyond simply performing the surgery and discharging the patient. It requires a multidisciplinary effort, with investments in establishing preoperative optimization programs, patient education classes and a coordinated team approach on the day of surgery.
Patients undergo physical therapy before returning home, but the care doesn’t stop there. We must ensure effective pain management, minimize infection risks and create a safe home environment to support their recovery. This process goes beyond safely discharging patients. It’s about ensuring their complete and safe recovery. I’m proud of the extensive teamwork and complex processes that Wellstar has implemented to support these programs.
Quehl: When it was time to correct my right shoulder this past year, I went in the morning and came back home in the evening. Dr. Burns assured me that I’d be home the same day, and it was a wonderful experience. I didn’t want any overnight stays. It was well-planned and executed, with proper anticipation and expectations set. The follow-up was excellent, too.
Dr. Brooks: Patients are shocked or hesitant when I inform them that they’ll go home the same day. It’s about managing expectations and explaining the benefits, especially as it relates to improved outcomes. Involvement in these programs gives physicians more control over the process. It’s a serious undertaking but rewarding because we can provide more input, especially in an outpatient setting. Collaboration with anesthesia colleagues has improved, particularly with techniques like regional blocks, as patients need to be up and about after surgery. Almost universally in my experience, patients prefer their outpatient surgical experience to any previous hospital stays.
Multimodal pain management success
Rubinger: This leads me to my next question regarding opioids and pharmacology. Has pharmacology evolved over the last decade to improve patient treatment?
Dr. Burns: Most of us are employing what we refer to as multimodal pain control, which involves a process aimed at sparing, if not entirely eliminating, the need for opioids as a primary method of pain management. By utilizing different medications that target distinct pain receptors, we can effectively manage pain while minimizing potential side effects that may arise from relying solely on opioids or multiple doses of the same medication. Advancements in regional blocks, administered by anesthesiologists, allow injections that can provide numbing effects in the affected areas for several days, alleviating initial post-operative pain and reducing patients’ overall need for pain medication over time.
Dr. Oswald: The opioid crisis in the greater Atlanta area is a significant concern for both children and adults, and it’s something we’re all acutely aware of. We’ve initiated extensive research efforts at Wellstar to address this issue and lead advancements in pain management that don’t rely on narcotics. Similar to the approach described in the total joint experience, we’ve been observing this trend for some time now, even in pediatric cases.
When I trained for pediatric spine surgery 20 years ago, patients stayed in the hospital for at least a week post-surgery. By implementing multimodal approaches, we’ve managed to reduce narcotic use by nearly 90% while also transitioning from a week-long hospital stay to just a 23-hour observation period for certain procedures.
Patient satisfaction is higher with these approaches, directly correlating with their overall experience. Are we expediting discharge solely for the sake of pushing people out? Actually, no. It’s about ensuring patients feel empowered in their recovery process, with their pain managed effectively, and their ability to return to the quality of life they desire. These patient-centered care programs optimize outcomes and enhance the overall healthcare experience.
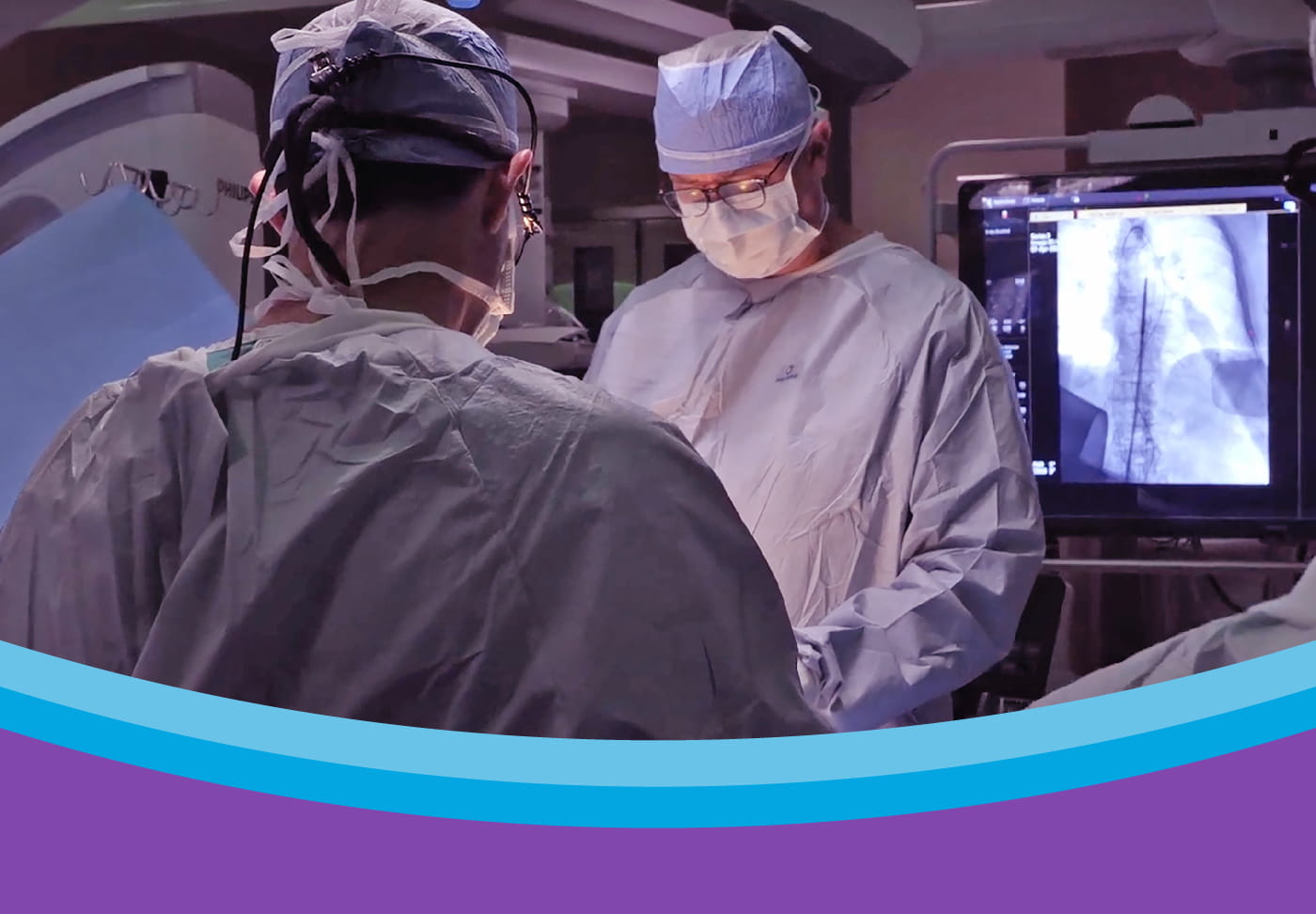
Wellstar’s Comprehensive Aortic Program has identified thousands of hidden aneurysms in the past two years. The goal of the program is to help people before their conditions become life-threatening.
Aortic aneurysms are bulges in the body’s largest blood vessel. They can burst and cause severe damage or death if they become too big. Unfortunately, most people never know they have one because they are typically asymptomatic until they rupture.
However, the aortic experts at Wellstar found a way to help people before they have an emergency.
“When patients have CT scans at Wellstar for other reasons, we use artificial intelligence (AI) to sift through them and find images of someone who may have aneurysm,” said Wellstar Cardiothoracic Surgeon Dr. James Ryan Burke. “That allows us to proactively contact them and bring them in if appropriate for evaluation to discuss that diagnosis.”
Since the program launch in July 2022, more than 4,700 people with aneurysms have been placed under surveillance—a protocol to monitor people who have a risk. Surveillance allows people to avoid undergoing unnecessary surgery but to know when the aneurysm grows larger and becomes a greater concern.
For people who had large, potentially life-threatening aneurysms, cardiovascular surgeons and vascular surgeons performed more than 700 advanced procedures at Wellstar Kennestone Regional Medical Center since the program began.
“These are major cardiac operations only performed in centers that offer complex aortic surgery,” Dr. Burke said. “The outcomes are best when done in experienced centers that do a high volume of procedures, like Wellstar Kennestone.”
Patient-centered aortic care
“This program is very patient-oriented. We have an excellent team of dedicated physicians at Wellstar to accomplish our mission and I think it’s very beneficial for both patients and physicians,” said Vascular Surgeon Dr. Michael Corey.
The aortic program at Wellstar provides a higher level of aortic care than a patient would typically find in a local hospital. What makes the program unique is:
- The multispecialty team of aortic experts working together
- The cutting-edge AI technology used to identify patients who are unaware they have an aneurysm
- A high-tech hybrid operating room (OR) for open or minimally invasive procedures
- The latest surgical techniques and technology
- A high volume of procedures performed
“The aorta is the largest blood vessel in the body. It runs from the heart, through the chest and abdomen and down to the legs,” said Dr. Burke. “When you have a disease process involving the aorta, it requires multiple specialties.”
Wellstar’s specialized aortic team includes cardiovascular surgeons, vascular surgeons, cardiologists, anesthesiologists, radiologists, nurse practitioners and physician assistants.
There is also a cardiac hybrid OR that brings a catheterization lab and surgery suite together in one space, making aortic aneurysm treatment more efficient and encouraging collaboration between our expert providers.
“The hybrid OR is a state-of-the-art, innovative, open operating room where patients can receive complex aortic reconstructions—procedures that have open surgery components to them—as well as endovascular (or minimally invasive) aortic reconstructions. This all can take place in one nice operating room,” Dr. Corey said.
The aortic program is part of a larger heart care program at Wellstar, based at Wellstar Kennestone, the first in Georgia and the fourth in the nation to receive Comprehensive Cardiac Care Center Certification by The Joint Commission and American Heart Association. This is the highest certification in cardiovascular care.
Learn more or schedule an appointment with an aortic disease specialist.
;
ENABLED PAGINATION OFF TEXT ALIGN CENTER
.jpg?rev=0c641d247be3492db97099991e0fef7f)
To celebrate Women’s Health Month, more than 150 executives gathered Thursday at The Studio Theatre in Sandy Springs for insightful discussions on advancing women’s health in Atlanta and throughout Georgia.
The Women's Health Summit, presented by the Atlanta Business Chronicle and Wellstar Health System, featured two panels of experts and a keynote address by renowned health and wellness expert Emma Lovewell.
Cheryl Preheim, anchor at 11Alive (WXIA), welcomed attendees and served as a moderator.
;
For more than a year, our communities have done their part to fight COVID-19.
We have stayed home, worn masks when we’ve gone out, been extra careful with washing our hands and avoided large gatherings. That’s meant that holidays and birthdays have looked a little different, all so we can stay safe and healthy.
The separation and fear have been draining, and many of us have dealt with loneliness and stress as we worry about our health and our loved ones.
But now we have something to celebrate. Hope has arrived in the form of the COVID-19 vaccine. All Georgians age 12 or older are now eligible to get their shots.
At Wellstar, we've chosen to lead by example. Across our health system, frontline healthcare workers and leadership have "stuck it to COVID." Whether they want to gather with friends and family, travel to a new destination or help protect vulnerable members of the community, our Wellstar team members all have their #MyWhy — the reason they chose to get vaccinated.
For Dr. Jeffrey Hines, chief of gynecologic oncology for Wellstar, getting the shot was about a sense of responsibility. As medical director of the Wellstar Center for Health Equity, Dr. Hines works to ensure our underserved populations have access to the care they need to stay safe and healthy. He got the COVID-19 vaccine to protect those around him.
“I’m a father, I’m a husband, I’m a brother and I’m a grandfather, and it’s important for me to protect my family,” Dr. Hines said. “I understand the science, and the science is important, but equally important to me is I want to be a trusted voice to people in the community who are most at risk for this and perhaps may have the most questions.”
Dr. Sophia McIntyre, senior vice president of Wellstar Medical Group, also said she got her shot to stop the spread, noting that COVID-19 has disproportionately affected minority communities.
“The reason why I got the COVID-19 vaccine is to ensure that I’m doing my part to bend the curve,” Dr. McIntyre said. “We know that African Americans and Latino Americans are dying at a higher proportion.”
Dr. Danny Branstetter, Wellstar’s medical director for infection prevention, has been at the forefront of Wellstar’s work to fight COVID-19 and keep our communities safe. Now, he wants to see life return to normal, because health isn’t just about your body. It’s also about your personal connections and overall well-being.
“I’m tired of being separated from my friends and family. I’m tired of seeing small businesses fold,” Dr. Branstetter said. “I’m tired of seeing the increased burden this places on those without resources. I’m tired of the loneliness this puts on those who are isolated and the elderly. My question is, aren’t you tired, too?”
All of us play a part in ending this pandemic.
“We’re in this together, and we can end this together through vaccination,” Dr. Branstetter said.
To find a vaccination site near you, visit the Georgia Department of Public Health website or local retail pharmacy.
;

Christmas carols and telephones ringing filled the Wellstar Children’s Hospital of Georgia lobby December 7 through December 9, 2023 for the 23rd annual iHeartMedia Cares for Kids Radiothon.
Thanks to the generosity of supporters, a check for $262,693 was presented to Wellstar Children’s at the conclusion of Radiothon on Saturday, December 9.
Throughout the event, radio stations 104.3 WBBQ, 96.3 Kiss-FM and 105.7 The Bull broadcast live from the lobby while WRDW News 12/NBC 26 shared stories of hope. Families of pediatric patients who have successfully finished treatment or are undergoing treatment at Wellstar Children’s, which is a member of the Children’s Miracle Network, stopped by to share stories of the world-class care their children received from the caring staff and expert caregivers.
“Every dollar that’s raised this weekend with Radiothon stays right here at Wellstar Children’s Hospital of Georgia and directly benefits the care of the children,” said Pediatrician-in-Chief Dr. Valera Hudson. “We’re the second largest children’s hospital in Georgia and the only children’s hospital outside of Atlanta. We offer the highest level of care to the sickest and most complex children. We hope you never need us, but if you ever need us, we’re here.”
Donations to Radiothon are used to purchase much-needed items that are unique to a children’s hospital, such as a vein finder for the neonatal intensive care unit. This device shines a red light through an infant’s arm or leg and helps caregivers find their tiny veins without having to stick them with a needle multiple times to administer fluids and medications.
The funds are also used to provide additional supplies for patient care as needs arise.
Though Radiothon is over, pledges are accepted year-round by calling (706) 721-4004 or by visiting the Cares for Kids Radiothon website.
;
Christmas music and cheers filled the halls of Wellstar Children’s Hospital of Georgia Dec. 5 through 7 as listeners and viewers of local iHeartMedia radio stations and WRDW-TV generously supported patients and families for the 24th consecutive year.
In the end, the community pledged $255,612 to support Wellstar Children’s.
iHeartMedia generously donated the 72 hours of airtime to the cause while three of its popular radio stations—104.3 WBBQ, 96.3 Kiss FM and 105.7 The Bull—and WRDW News 12/NBC 26 broadcast live from the hospital.
“The children’s hospital could not survive without the support of the community. I’m just so grateful for everyone’s support,” said Dr. Valera Hudson, pediatrician-in-chief of Wellstar Children’s. “No children’s hospital thrives without philanthropy; 100% of the money that’s raised is used directly to help the children we take care of here. All of the funds stay right here at the Wellstar Children’s Hospital of Georgia.”
Wellstar Children’s is a not-for-profit hospital with specialists who care for pediatric patients with a range of conditions, including the most complex conditions.
Some of the patients who have been treated at Wellstar Children’s shared their stories with DJs and reporters throughout Radiothon. For example, 9-year-old Kensley Woodberry began developing spots on her hands and feet that became so painful, she could no longer walk. She stopped eating and refused to play. A team of specialists at Wellstar Children’s diagnosed her with juvenile dermatomyositis, a rare autoimmune disease that causes the body to attack its own muscles and leads to inflammation throughout the body.
This past summer, Kensley attended Camp Joint Venture, a summer camp for children with rheumatic conditions. It gives kids like Kensley the opportunity to enjoy the summer camp experience while a team of medical personnel is nearby in case they are needed. The camp is one of several summer camps funded through Radiothon.
Radiothon also allows for purchases of comfort items like Zaky Hugs, which mimic the warmth and security of a parent’s touch for babies in the NICU; red wagons for transporting young patients around the hospital; and sensory toys for children with autism. These are only a few of the items that bring joy, comfort or care to young patients that the hospital could not purchase without community support.
Though Radiothon has concluded, donations can be made throughout the year by calling (706) 721-4004, by emailing Wellstar Children’s Director of Philanthropy Catherine Stewart or through the Cares for Kids Radiothon website.
;
The iHeartMedia Cares for Kids Radiothon filled the lobby of Wellstar Children’s Hospital of Georgia Dec. 4 through 6 for its 25th year of fundraising. Surrounded by a winter wonderland of Christmas trees and red, white and silver balloon arches, volunteers took donations from generous supporters while iHeartMedia radio stations and WRDW-TV broadcast stories of the miracles that happen every day at Wellstar Children’s Hospital of Georgia.
The event raised $291,617 to support the children’s hospital, which is a part of the Children’s Miracle Network.
“Thank you, thank you, thank you! This is life-changing,” said Ralph Turner, president of Wellstar MCG Health Medical Center. “This can support many of our young patients. They come to us and we take care of them. We don’t turn them away, and this really helps support our mission.”
Dr. Valera Hudson, pediatrician-in-chief, echoed Turner’s gratitude.
“We couldn’t do this without community support. We are so grateful for everyone who is here who helped pull this off,” she said.
Each year, iHeartMedia generously donates 72 hours of airtime as DJs from 96.3 Kiss FM, 104.3 WBBQ and 105.7 The Bull join WRDW-TV to broadcast live from the event, sharing success stories from patients and families grateful for the care they received.
“Thank you, CSRA, for making miracles happen. Exactly 291,617 miracles. Thank you!” said Ivy Elam, market president of iHeartMedia in Augusta.
Donations from the iHeartMedia Cares for Kids Radiothon are used throughout the year to purchase pediatric equipment such as vein finders for babies in the neonatal intensive care unit and a gaming system for patients in the pediatric operating room.
They also support programs that are unique to a children’s hospital. These include the facility dog program, featuring three hospital-owned dogs who provide comfort and help Child Life Specialists more easily communicate with young patients. Donations also help fund summer camps for children living with chronic conditions—such as Camp Rainbow for cancer patients—which allow kids to just be kids while remaining under medical supervision.
Radiothon has ended, but donations can be made throughout the year by calling (762) 375-4004, by emailing Wellstar Children’s Hospital of Georgia Director of Philanthropy Catherine Stewart or by visiting the Wellstar Foundation.
;TEXT ALIGN -RIGHT /ENABLED PAGINATION vertical limit-4

Many men are reluctant to seek diagnosis and treatment of prostate cancer because they fear the effects of treatment on their urinary and sexual function. Enter modern technology. MRI scans, PET scans and molecular testing of blood and tissue samples not only help physicians know how and where to treat, but also identify those who may not need any treatment.
Having a PSA blood test is usually the first step in detecting prostate cancer. Now, modern MRI scans can help the urologist target abnormal areas for biopsy, like how a GPS pinpoints a destination. With this technique, patients can be more confident that the biopsy samples accurately represent their condition. In fact, this confidence has allowed men with slow-growing forms of prostate cancer to observe their condition rather than immediately pursue treatment. Since the formation of cancer cells all starts with changes in a cell’s genetic material, specialized testing of the biopsy sample can help further define the behavior of an individual’s prostate cancer.
When treatment for prostate cancer is needed, the latest methods bring next-level precision to protect the delicate nerves and muscles surrounding the prostate. Now in its second decade as a standard treatment for prostate cancer, robotic prostate removal continues to break barriers with new instrumentation, refined techniques and artificial intelligence. Not only do these advancements speed up recovery, but they also facilitate less traumatic access to spaces that were previously very difficult to reach. Similarly, the latest radiation therapy techniques allow delivery of a thin beam to the prostate.
For more aggressive forms of prostate cancer, the latest type of PET scan can identify the cancer in other locations. First, a radiotracer (slightly radioactive substance) is injected into a vein, and it binds to prostate cancer cells, wherever they may be hiding. Then the resulting X-ray images are superimposed onto a CT scan to highlight any areas of suspicion. We can now attach medications to this radiotracer to attack and kill remote prostate cancer cells like a guided missile.
With these recent advancements in technology, the management of prostate cancer continues to be more effective and gentler for the modern man. One can only imagine what’s on the horizon.
Learn how to support a loved one through their prostate cancer diagnosis.

At Wellstar, our doors are open to everyone. Whether it’s an individual with a life-threatening health crisis or a family looking for a new primary care provider, we’re here to help.
Sometimes, it’s not enough to welcome people in. We also need to go out into the communities we serve to meet people where they live, work and play to ensure they receive high-quality care.
To meet more of our neighbors where they are, we partner with organizations like Ser Familia. Founded in 2001 in the Metro Atlanta area, Ser Familia equips Latino families with the tools, resources and skills they need to thrive. Ser Familia’s extensive wraparound services include support groups, family workshops, mental health counseling and educational programs. In recent years, Ser Familia has expanded its footprint with new locations across Georgia and Puerto Rico.
The power of working together
Wellstar Center for Health Equity has a long-standing relationship with Ser Familia. For example, Wellstar provides grant funding so Ser Familia can employ Spanish-speaking community health professionals. These professionals have a unique ability to provide health information where it is needed most. They can:
- Connect families with health resources in their community, including primary care providers
- Offer language translation services
- Provide health education and information
- Give informal guidance about healthy behaviors
Also, Wellstar physicians participate in Ser Familia community health outreach programs serving Latino communities.
Excitement about a planned health clinic
In the near future, Ser Familia plans to open a health clinic with the support of Someone Cares, Inc. of Marietta, another Wellstar partner. The clinic will provide comprehensive primary care, including health, education and preventive services. Nurse practitioners will see patients at the clinic under the guidance of physicians at Someone Cares. And, if patients need care that Ser Familia does not offer, the nurse practitioners can refer them to a Someone Cares provider.
When organizations like Wellstar and Ser Familia work together, we accomplish far more in our communities than we could separately by making better use of our resources. Most importantly, we help people find the care they need where they need it.
Learn more about Wellstar Center for Health Equity.
;
There’s a reason the “widowmaker” heart attack got its nickname. According to the American Heart Association, the survival rate following this type of heart attack, which is caused by a blockage in the heart’s main artery, is only 12% when it occurs outside a hospital or advanced cardiac care center. But thanks to the swift response of his cardiac-nurse wife and the excellent care of his cardiovascular surgery team, Martin Hornberger is here to tell his story and offer hope to others.
The power of CPR
It was a Saturday morning in May. Martin started his day with breakfast and a cup of coffee—as he always did. He had no pain or unusual symptoms—merely some indigestion, which he managed by taking a few antacids, and fatigue that was a common symptom of his diabetes.
Aside from having diabetes, the Cartersville resident had always considered himself relatively healthy. When he wasn’t hard at work as an engineer, he spent much of his time outdoors and enjoyed staying active.
Everything changed later that day when he and his wife, Donna, left the house to see their granddaughter play tee ball. Halfway there, Martin collapsed while driving.
“I tried to tell my wife to take the steering wheel but never got the words out,” he said.
Donna, a cardiac nurse at Wellstar Kennestone Regional Medical Center, jumped into action. Unable to move Martin’s foot off the gas pedal, she eventually got the truck under control by turning off the ignition. Then, using her nearly 50 years of emergency room and cardiac training, she began administering hands-only CPR. Another driver who stopped to help called 911.
While the EMTs were en route, Donna was able to revive Martin by delivering multiple rounds of chest compressions to mimic the heart’s pumping action.
“Knowing her, she didn’t even have to think about it. Her training kicked in and she just went to work,” Martin said of his wife. “She’s the hero of this whole thing.”
Determining a plan for treatment
The EMTs rushed Martin to a nearby hospital in Rome, where the cardiac team performed an emergency stent to restore blood flow in his main heart artery and get him stabilized. However, further tests revealed even more blockage that could not be treated with additional stents. Martin would need heart bypass surgery.
Donna immediately began advocating for him to be transferred to her unit at Wellstar Kennestone for surgery. She wanted the best possible care for her husband and knew the Marietta hospital was a Certified Comprehensive Cardiac Care Center—the first in Georgia and the fourth in the nation to receive this highest certification in cardiovascular care by The Joint Commission and American Heart Association.
“I knew the process; I knew the people,” she explained. “If anyone could save my husband, it was them.”
Patient-centered approach
On Wednesday evening Martin was moved to Wellstar Kennestone, where he was introduced to Dr. Richard Myung, the cardiothoracic surgeon who would be performing his coronary artery bypass grafting (CABG) surgery. Dr. Myung took the time to explain to Martin everything that would happen during the procedure. The surgeon’s personable demeanor and genuine empathy immediately put Martin at ease.
“He has a tremendous bedside manner—his presence in the room was comforting,” Martin said. “The smile on his face and the relaxed confidence [gave me] reassurance that things are going to work out.”
Dr. Myung works as part of a larger multidisciplinary team to provide the highest quality care to every patient, from diagnosis to surgery and through recovery. His commitment to excellence has helped Wellstar Kennestone’s cardiovascular program earn a distinguished three-star rating from the Society of Thoracic Surgeons for its patient care and outcomes in isolated CABG. The award places the hospital among the most elite programs for heart bypass surgery in the U.S. and Canada.
Advanced techniques for improved outcomes
Martin’s case, unfortunately, was not unique for Dr. Myung. “Probably a third of our cases are bypass cases,” the surgeon explained.
CABG is regularly performed to treat people with multiple blocked coronary arteries. It involves a surgeon taking a healthy vein or artery from another part of the body (in Martin’s case, Dr. Myung used a vein from his leg and an artery from his chest wall) and attaching it to the aorta and the coronary artery above or below a blockage. This creates a new route for blood to flow around the blockage.
Although the most common approach is traditional open-heart CABG, where the heart is stopped and a heart-lung bypass machine is used, other less-invasive methods—including “off-pump” procedures, in which the heart does not have to be stopped—are sometimes an option. Dr. Myung determined that Martin could undergo an off-pump CABG, which reduces the risk of complications and often leads to a shorter hospital stay.
When the big day arrived, Martin’s procedure went smoothly, Dr. Myung reported. Thanks to his expert team and their advanced techniques, Martin was going to be okay.
Compassionate care at every step
Martin is grateful to the nursing team at Wellstar Kennestone for supporting him before, during and after his procedure.
“From beginning to end, they were attentive, encouraging [and] they coached me through each step,” he shared.
One nurse in particular made a lasting impact on Martin through his clear, comforting instructions that let him know exactly what to expect.
“Prior to the surgery, he was telling me, ‘Now, when you wake up, you’re going to have a tube in your throat. Don’t fight it. Just remember that this is part of the recovery.’ And you know, that stuck in my mind,” Martin recalled. “They had prepared me for everything I was going to face. There were no surprises, and I really appreciated that.”
Within 24 hours of his bypass surgery, Martin was out of bed and walking laps around the hospital floor with a walker. “I even heard a patient telling the nurses, ‘Tell that guy to slow down!’” he said with a laugh.
With the specialized care of his nursing team, he continued to improve daily and was discharged only four days after surgery.
“That whole place is full of heroes. They do it day in and day out,” Martin said. “They love what they do and they’re good at it. They take pride in that—and they should.”
Adjusting to a new normal
Thanks to Dr. Myung and his less-invasive techniques, Martin experienced a relatively painless recovery. Six weeks after his surgery, Martin felt well enough to return to his full-time job.
Determined to get back to life as normal as quickly as possible, Martin kept himself moving at home and also visited Wellstar Cardiac Rehabilitation in Woodstock to continue building his strength. Wellstar has one of the largest cardiac rehabilitation programs in Georgia, which helps patients improve their long-term outcomes.
Martin will continue to monitor his cardiac wellness through regular check-ups with expert Wellstar cardiologists. The Wellstar Center for Cardiovascular Care ensures patients who recently had heart surgery can easily receive the follow-up care they need by offering more than 20 convenient locations across Georgia.
Martin recognizes that adjusting to life after a heart attack—and all the emotional challenges and physical limitations that come with it—will take time. For now, he is focused on making small strides every day.
“I do get tired but not as often, so I’m seeing progress in the length of time that I’m doing activities, that I’m able to sustain it longer,” Martin shared. “That’s encouraging.”
Staying the course
Without the first-rate care he received at Wellstar, Martin wouldn’t be where he is today—back to work, living an active lifestyle and surrounded by his children and grandchildren, who lovingly call him “Gramps.”
He also wouldn’t have had the chance to make a memory he would cherish forever. On a Sunday afternoon in August, Martin was selected by Wellstar to throw the opening pitch at the Atlanta Braves vs. Miami Marlins baseball game. He was joined by Donna and their family on the field at Truist Park and later enjoyed cheering on the home team alongside Dr. Myung.
“That was a huge experience in my life,” Martin said. “Never in my wildest dreams did I imagine I would ever do that in my lifetime.”
Today, Martin is sharing his story to encourage others who may be recovering from a heart condition. “It does get better,” he offered. “It doesn’t happen as quickly as you want it to, but I can see it progressing.”
By recounting her husband’s experience, Donna has inspired several of her patients to consider cardiovascular procedures that could detect potential blockages. She also hopes it will influence more people to learn CPR.
“If our story can even save one life, that would mean the world to us,” she said, humbly adding, “I’m not a hero; I’m a wife that loves her husband that just so happens to be a cardiac nurse.”
Martin is all too aware that his wife’s combination of critical thinking skills, composure under pressure and cardiac training is why he is still here today. “I was lucky to have a cardiac nurse as my passenger that day,” he shared. “I am very blessed to be alive.”
Learn more about Cardiovascular Surgery at Wellstar.
Wellstar Kennestone Regional Medical Center has received several major commendations highlighting the high level of heart care continuously provided to patients—putting Wellstar’s cardiothoracic surgery program among the top in the nation. The Marietta-based heart care program received:
- The coveted three-star rating in the following key areas from the Society of Thoracic Surgeons (STS): isolated coronary artery bypass grafting (CABG, or open-heart surgery), aortic valve replacement (AVR), AVR + CABG, and multiprocedural cardiothoracic surgeries. This is the highest category of quality, placing Wellstar Kennestone among the best programs for heart surgery in the U.S. and Canada.
- The prestigious Comprehensive Cardiac Care Certification—the highest distinction awarded by The Joint Commission and the American Heart Association. Wellstar Kennestone was the first in Georgia to receive this certification.
These recognitions demonstrate Wellstar’s commitment to keeping advanced heart care close to home.
“These accomplishments speak volumes about the skill, precision and teamwork of our cardiothoracic team,” said Dr. Richard Myung, medical director of cardiothoracic surgery at Wellstar Kennestone. “We’re proud to deliver exceptional outcomes for patients from across the Southeast who have some of the most complex heart conditions.”
Three-star STS rating
STS ratings reflect not only surgical excellence, but also the quality of care patients receive in the critical 30-day period following surgery.
These results highlight the importance of a multidisciplinary approach—one that includes surgeons, anesthesiologists, perfusionists, nurses, cardiologists, respiratory therapists, rehabilitation specialists, critical care specialists, hospitalists, advanced practice providers and many others.
“This achievement is a testament to the entire care continuum,” said Steve Cermak, executive director of cardiovascular service line and hospital operations at Wellstar Kennestone. “From the operating room to recovery and rehabilitation, every team member plays a vital role in delivering outstanding outcomes.”
Among the three-star rankings is CABG. This procedure is commonly performed to treat people having a heart attack or other conditions including coronary heart disease with chest pain, multiple blocked coronary arteries or serious heart failure. The procedure is performed by cardiovascular surgeons at Wellstar Kennestone—Dr. Theresa Luu, Dr. James Burke and Dr. Richard Myung—who work as part of a large multidisciplinary team to give every patient the highest quality care at every step of the process, from diagnosis through surgery and recovery.
“This amazing recognition is about the great lengths we go to care for our patients, and why people travel from across the region to receive their care at Wellstar Kennestone,” added Director of Wellstar Cardiothoracic Surgery Services and the Structural Heart and Valve Program Karrie Davis. “We care for every patient like they’re a family member or close friend. That’s why we hold ourselves to the highest standards.”
Wellstar Center for Cardiovascular Care offers patients care close to home across Georgia communities at more than 25 cardiovascular locations, with more than 110 cardiologists and cardiothoracic surgeons standing ready to provide heart care for both routine and complex heart conditions. Wellstar also has one of the largest cardiovascular rehabilitation programs in Georgia, which helps patients improve their long-term outcomes.
Certification by The Joint Commission
The Joint Commission has also awarded Wellstar Kennestone with a Gold Seal of Approval in conjunction with the American Heart Association’s Heart-Check mark and certification as a Comprehensive Cardiac Center for the third consecutive time.
For the certification, Wellstar Kennestone underwent a rigorous, unannounced onsite review. During the visit, a team of Joint Commission reviewers evaluated compliance with related certification standards including evaluating the care of the cardiac patient at every touch point in the cardiac care continuum with ongoing process improvement and health promotion for patients, as well as the community. Joint Commission standards are developed in consultation with healthcare experts and providers, measurement experts and patients. The reviewers also conducted onsite observations and interviews.
The hospital first received the two-year certification in 2019. This recertification makes the third cycle—or sixth year—it has remained in place. Wellstar Kennestone was the first hospital in Georgia and remains the only one in the state to hold the comprehensive certification.
From prevention to post-cardiac event recovery, our well-connected and collaborative heart care team is dedicated to empowering you to regain your strength and independence. We offer top-quality cardiovascular care including diagnostics, treatment, psychological support and ongoing monitoring all focused on your well-being. Learn more about award-winning heart care at Wellstar.

John Petrick loves the simple things in life. He revels in time spent with family, reeling in a big catch and feeling the crisp wind in his face during a morning bike ride.
However, for a man that enjoys such simple pleasures, John’s heart health is quite complicated. For a long time, his well-being felt like a puzzle that no one could quite figure out.
John’s complex heart issues first began over two decades ago, when he nearly died after his heart suddenly went into an abnormal rhythm.
After the life-threatening heart episode, specialists in California diagnosed him with ventricular tachycardia (VT), a severe heart condition in which abnormal electrical signals cause the heart to beat faster. Then later, he was also diagnosed with atrial fibrillation (AFib), an irregular and rapid heart rhythm that can cause heart palpitations and shortness of breath.
From defibrillators to heart surgeries, John and his Californian care team worked hard to manage the ups and downs of his heart conditions. But after spending years in the Golden State, John was ready to take on a new adventure: moving over 2,000 miles away to Georgia.
“The decision to move to Georgia was difficult because of my heart conditions,” John shared. “I needed a doctor who would really take the time to sort everything out.”
Luckily, it wasn’t long before John was connected with an entire team of Wellstar heart experts delivering comprehensive care all within the same health system.
Finding the right rhythm
Before being referred for specialty care by his Wellstar primary care provider, John briefly received heart care from another health system in Georgia. However, he had some reservations about his treatment.
“Honestly, it wasn’t the level of care—especially in terms of empathy—that I was used to,” he admitted. “And that’s a scary situation when you have a condition like mine.”
That was never a problem at Wellstar. As soon as he met with Wellstar Health System Director of Cardiac Electrophysiology Dr. Narendra Kanuru, John knew the physician was in his corner.
“I could tell Dr. Kanuru really took the time to study my case,” John said, remembering his first visit with the specialist. “He recited my medical history from the last 20 years, without having to look at any papers.”
Since then, they have developed a great healthcare partnership, always keeping an open line of communication.
“I feel so comfortable expressing any fears or apprehensions about my conditions or treatment with Dr. Kanuru. He’s always very receptive,” John shared. “His level of empathy, professional expertise and ability to communicate and understand me is just as valuable as his technical, medical skills.”
Along with Dr. Kanuru’s expertise, Wellstar Cardiologist Dr. David Caras provides an essential complement to John’s cardiovascular care. While a cardiac electrophysiologist hones in on the functional and rhythmic areas of the heart, a cardiologist offers a broad spectrum of heart care.
While each focusing on their areas of expertise, the two heart specialists collaborate to create the best treatment plan for John, and adjust it along the way.
“Dr. Kanuru and Dr. Caras work together as a team,” John said. “It’s truly remarkable and beautiful. Often, I’ll go to see one of the doctors and they’ll mention a conversation they had about me with the other recently.”

The largest emergency department (ED) in Georgia just passed a huge milestone. Wellstar Kennestone Hospital’s new, state-of-the-art ED has now been serving Cobb County and the surrounding community for one year.
From saving lives with advanced medical care to fighting COVID-19 on the frontlines, our expert emergency team has truly risen to the challenge over the last year — and we’re just getting started.
At 263,000 sq. ft., our Level II Trauma Center is more than double the size of the hospital’s prior ED. However, it’s not just the impressive size of the building that sets it apart.
With cutting-edge technology, leading treatments and expert providers always at the ready, the Wellstar Kennestone ED delivers better, faster care when it matters most.
PeopleCare when it counts
When it comes to emergency care, every second matters.
From top to bottom, the new ED is built to save lives. The innovative layout includes separate care zones based on medical service, level of care and age, allowing us to treat patients faster. We even have a full-service pediatric area so our littlest patients can receive specialized, kid-friendly care.
Since its opening on July 23, 2020, the Wellstar Kennestone ED has:
- Served 104,980 of our family, friends and neighbors in the community.
- Treated 10,759 pediatric patients, who can get back to being kids again.
- Performed 319 emergency surgeries with advanced, life-saving technology.
- Landed 244 helicopters, which flew patients in for fast, expert treatment.
While those may be a lot of statistics, Wellstar never treats people like a number. With the ED’s high-tech capabilities and smart design, our medical experts can still personalize care even amid a life-threatening situation.
So, whether you or a family member experiences a traumatic injury or sudden medical emergency like a heart attack or stroke, the Wellstar Kennestone ED offers quick, effective emergency care close to home.
Care during COVID-19 & moving forward
Emergencies don’t stop — even during a pandemic. When the Wellstar Kennestone ED opened during the height of the COVID-19 outbreak, Georgians still needed to find safe emergency care.
We’ve added new infection prevention protocols into our already thorough safety routines, ensuring our medical experts can provide safe, life-saving care every day. In uncertain times, people count on Wellstar for expert trauma and emergency care.
Today, the Wellstar Kennestone ED is continuing to protect the people and communities we serve. From emergency surgery to expert trauma care to behavioral health services, we make sure people can get the emergency care they need without going far.
Learn more about the Wellstar Kennestone ED and how we are making a difference in Georgia.

Every day, Scott Hullihen’s gaze falls on a very unique piece of art hanging in his home.
To the untrained eye, the spiraling streaks across the canvas could be mistaken for an abstract painting in a museum. But for Scott, it holds a much deeper, personal meaning: hope for a cancer-free future.
A closer look reveals a puzzling QR code in the corner of the print and, when scanned, it plays the very voicemail from his Wellstar radiation oncologist that got him through the most difficult days in his cancer journey.
“The picture is his voice in soundwaves. I get to see it every day,” said Scott. “It’s the most thoughtful thing I’ve ever seen in my entire life.”
The ebbs and flows of the piece show how he conquered the highs and lows of his difficult rectal cancer diagnosis, with support from Wellstar as the constant through it all.
Just like the highly personalized art print, his expert team of physicians formed a tailored care plan for Scott, right down to his DNA.
Together with his Wellstar team, Scott beat cancer and is back to living life to the fullest.
A surprising diagnosis
Scott was a typical guy in his 30s, working in technology and spending time with friends and family.
“Everything was normal,” he said. “I’d go to sporting events or concerts.”
But his diagnosis of colorectal cancer at just 35 years old was anything but typical.
“That was shocking,” he said.
In 2020, Scott’s stomach started hurting—and it didn’t stop. He started eating better and cut certain ingredients from his diet. He regularly rode his bike for 15 miles.
“I was getting in good shape!” he said.
But the pain continued, with an urgency to use the bathroom, constipation and blood. His doctor referred him to a gastroenterologist for a colonoscopy in August. Immediately after the procedure, he learned there was a tumor in his colon.
“It was a quiet car ride,” Scott remembered sitting silently next to his mother, who had driven him there.
That Friday, a biopsy confirmed it was cancer. Scott was immediately referred to the Wellstar Rectal Cancer Multidisciplinary Program, the first and only treatment center in metro Atlanta accredited by the National Accreditation Program for Rectal Cancer (NAPRC), a quality program by the Commission on Cancer.
Getting the highest level of rectal cancer care
After the weekend, Scott met with Dr. Sahir Shroff, a cancer surgeon.
“People raved about how good a surgeon Dr. Shroff is—I learned he was one of the best in the state,” Scott said. “He saved my life.”
The board-certified and fellowship-trained surgical oncologist reassured Scott.
“This is one of the most subspecialized rectal cancer programs in metro Atlanta,” he said. “Every person with rectal cancer is reviewed at our multidisciplinary meeting to provide the highest level of care.”
Select doctors are designated to stage and treat rectal cancer patients following evidence-based guidelines. The team includes colorectal surgeons, medical oncologists, radiation oncologists, gastroenterologists, pathologists and radiologists. Higher experience in treating rectal cancer leads to better outcomes for patients.
Scott also had a nurse navigator coordinate his cancer staging and treatment. Nancy Page answered questions and scheduled important appointments, such as CT scans and MRIs as well as meetings with various specialists.
A licensed Wellstar genetic counselor was also on Scott’s team. Amy Ekwurtzel found that Scott had two genetic abnormalities that make him slightly more susceptible to colorectal cancer. This information gave the team additional clues about the best way to care for Scott.
;
Wellstar Health System honored the life, legacy, and many contributions of Dr. Martin Luther King Jr. with a tribute and virtual ceremony on Jan. 13. The event included team members, faith leaders, and powerful voices from the diversity, equity, and inclusion community with uplifting and moving blessings, song, dance, images and messages.
Allyship, connectedness, and advocacy emphasized as tools to combat injustice
Wellstar physicians, caregivers, and team members are connected by the desire and commitment to serve with compassion, pursue excellence and honor every voice as the system strives to meet the vital needs of patients and communities.
During the virtual event, Wellstar president and CEO Candice L. Saunders reflected on the organization’s deep commitment to caring for people and Dr. King’s view of the world that all life is interrelated.
The ceremony’s keynote speaker, Dr. Johnetta Betsch Cole, chair and seventh president of the National Council of Negro Women and former president of Spelman College, an historically black college, emphasized the theme of the event from Dr. King’s “Letter from a Birmingham Jail,” wherein he stated: “Injustice anywhere is a threat to justice everywhere.” She talked about the importance of being an ally and advocate for any struggles against injustice, and encouraged all to build a better world where we can stand together. Dr. Cole was introduced by Le Joyce Naylor, Wellstar’s senior vice president and chief diversity, equity & inclusion officer.
In addition to inspiring messages from Dr. Cole and Saunders, the event included prayers and blessings from David A. Spencer Jr., manager of Wellstar Spiritual Health; Cavit Agu, chaplain for Wellstar Health System; Rabbi Judith Beiner of Jewish Family and Career Services of Atlanta; and Patricia Symonette, director of Wellstar Spiritual Health, who sang “Show Me How to Love,” by Babbie Mason. The Fellowship Bible Baptist Church Worship and Arts Ministry sang and danced to “Lift Every Voice and Sing,” by J. Rosamond Johnson and James Weldon Johnson. Dr. Scott Swayze, chair of the Wellstar Board of Trustees, closed the event with a message about Wellstar’s commitment to compassion, excellence, and inclusion.
Wellstar is honored to celebrate the life and legacy of American Civil Rights Movement leader and activist Dr. Martin Luther King Jr. and acknowledge this important federal holiday and National Day of Service in recognition of his enduring impact and example. Wellstar has added Martin Luther King Jr. Day to the paid holiday calendar starting Jan. 17, 2022.
;


Wellstar Mobile Markets were featured April 26 on WSB-TV Game Changers, a Family 2 Family Special, and on People 2 People on May 14. Wellstar Center for Health Equity and the Wellstar Community Health team are working with community partners Goodr and Wholesome Wave Georgia, along with a special volunteer, former Atlanta basketball star and Wellstar Community Ambassador Dominique Wilkins, to distribute nutritious, free food and health screening education to support the well-being of our communities. Community host sites have included partners such as C.H.O.I.C.E.S. and Roswell Organization for Community Development.
Through the mobile markets, Goodr provides fresh produce, meat, shelf-stable items, milk and other beverages. In addition, a benefit specialist from Wholesome Wave Georgia, another nonprofit increasing access to healthy foods, helps connect families with additional resources.
Learn more and find a market near you at wellstarmobilemarket.com.
Watch the WSB-TV People2People Interview.

Wellstar supports people with cancer throughout their journeys, from early screenings to diagnosis to treatment. But our encouragement and dedication to delivering world-class, compassionate care doesn’t end in remission.
Across our system, Wellstar honors the bravery and strength of survivors every day, rejoicing in each milestone. This National Cancer Survivors Day, June 1, 2025, we are proud to pay tribute to the people who have conquered cancer and offer hope to those still fighting. This year’s Cancer Survivors Day theme—Strike Out Cancer—exemplifies our commitment to being a steadfast source of encouragement for cancer survivors and fighters across Georgia.
“On Cancer Survivors Day, we reflect on our patients’ journeys and cherish victories over cancer. We also offer compassion and support for people currently fighting cancer, so they and their loved ones know they’re not alone,” said Wellstar Director of Oncology Professional Practices Melissa Higdon.
Several Wellstar facilities will host events—and you can be a part of the celebration!
Northwest Georgia Oncology Centers in Cartersville
June 5, 2025
10 AM to 3 PM
100 Market Place Blvd., Cartersville
Contact Mary Ellen Smither at [email protected] or (678) 858-1146.
Wellstar Cobb Medical Center
May 30, 2025
12 to 2 PM
4040 Hospital West Drive, Austell
Behind the building in the garden and parking lot area
Contact Ashley Dapremont at [email protected] or (470) 732-4523.
Wellstar Douglas Medical Center
June 7, 2025
11 AM to 2 PM
8954 Hospital Drive, Douglasville
Surgical services lobby
Contact Diane Harris at [email protected] or (470) 644-5411.
Wellstar Kennestone Regional Medical Center
June 7, 2025
11 AM to 2 PM
320 Kennestone Hospital Blvd., Marietta
First floor
Required RSVP, contact Nancy Page at [email protected] or (470) 793-7470.
Wellstar North Fulton Medical Center
June 1, 2025
2 to 4 PM
3000 Hospital Blvd., Roswell
Main lobby in hospital
Contact Sarah Bentley at [email protected] or (770) 751-2556.
Wellstar Paulding Medical Center
June 1, 2025
144 Bill Carruth Parkway, Hiram
Second floor auditorium
Contact Kellie Mitchell at [email protected] or (470) 644-8106.
Wellstar Spalding Medical Center
May 28, 2025
12 to 2 PM
Drive-thru event
608 South 8th St., Griffin
Women’s Center
Contact Sherry Connell at [email protected] or (470) 935-5526.
Wellstar West Georgia Medical Center
June 6, 2025
10 AM to 12 PM
111 Medical Drive, LaGrange
Enoch Callaway Cancer Center
Contact Stephanie Hand at [email protected].

With dedicated health resources and caring, compassionate providers, Wellstar is making primary care more accessible to people who are lesbian, gay, bisexual, transgender and queer/questioning (LGBTQ+).
Historically, many healthcare systems have not focused on the specific needs of the LGBTQ community.
“The LGBTQ community has been marginalized by the healthcare system,” Wellstar Primary Care Physician Dr. Gabriella Maris said. “There is a lack of providers who have adequate training to understand and treat their unique health risks.”
Wellstar believes every person should have access to safe, high-quality healthcare. At each of our primary care locations, we maintain a welcoming, non-judgmental environment to treat patients. Across Wellstar, we’re committed to providing inclusive medical services in a safe, comfortable space to make LGBTQ care more available.
Dedicated health experts for the LGBTQ community
Members of the LGBTQ community may be at a higher risk for certain medical issues.
For example, lesbian and bisexual women may be at increased risk for breast, cervical and ovarian cancer, according to the American Cancer Society. The American Psychiatric Association also shared that LGBTQ people are more likely to experience mental health concerns and use mental health services.
Treating these health concerns starts with trained providers who take a caring, compassionate approach to help patients stay healthy.
Wellstar provides primary care for the LGBTQ community, including wellness exams, chronic disease management, virtual appointments and other health screenings. We also offer special services for people who identify as LGBTQ including:
- Family planning and birth control
- Prenatal and OB/GYN care
- Pap smears for men and women
- Colposcopy and anoscopy
- Hormone therapy
- PrEP and nPEP treatment for HIV prevention
- Pediatric care
Gender-affirming care
Gender-affirming care is medical treatment that supports a patient’s gender identity when their identity differs from their sex assigned at birth.
“Gender-affirming care has the ability to save lives,” said Wellstar Primary Care Physician Dr. Danielle Ortega. “We know that a large percentage of transgender individuals, even starting in adolescence, have either suicidal intent or attempts in the past, and we know that gender-affirming care, when appropriate, improves mental health and prevents suicide.”
Active partners in your care
Wellstar physicians provide great care to patients and our health experts are dedicated to being a true partner in your wellness journey.
“I want for patients to know that Wellstar is their medical home—for them to feel comfortable when they walk in our door and for them to know that this is going to be a clinic that is not judgmental, is truly empathic and is here to help them in whatever way we can,” Dr. Maris said.
Our primary care team puts patients at the center of their care, presenting them with all their options and working with them to decide how to accomplish their goals.
“I get to know patients and understand what their goals are, what their hopes are, who their supports are, what their job entails, what their community is like and, specifically, what their goals are in relation to their health,” Dr. Ortega said.
;
These days, people can connect with friends online or join a virtual business meeting with just a click of a button. So, why not make your next doctor’s appointment just as easy?
With Wellstar Virtual Care, you can visit your Wellstar physician, remotely – from the comfort and convenience of home. All you need is a smartphone, computer or tablet to stay connected with your provider.
From getting wellness exams to managing chronic conditions, Wellstar Virtual Care gives you the flexibility to find safe, expert care anywhere.
;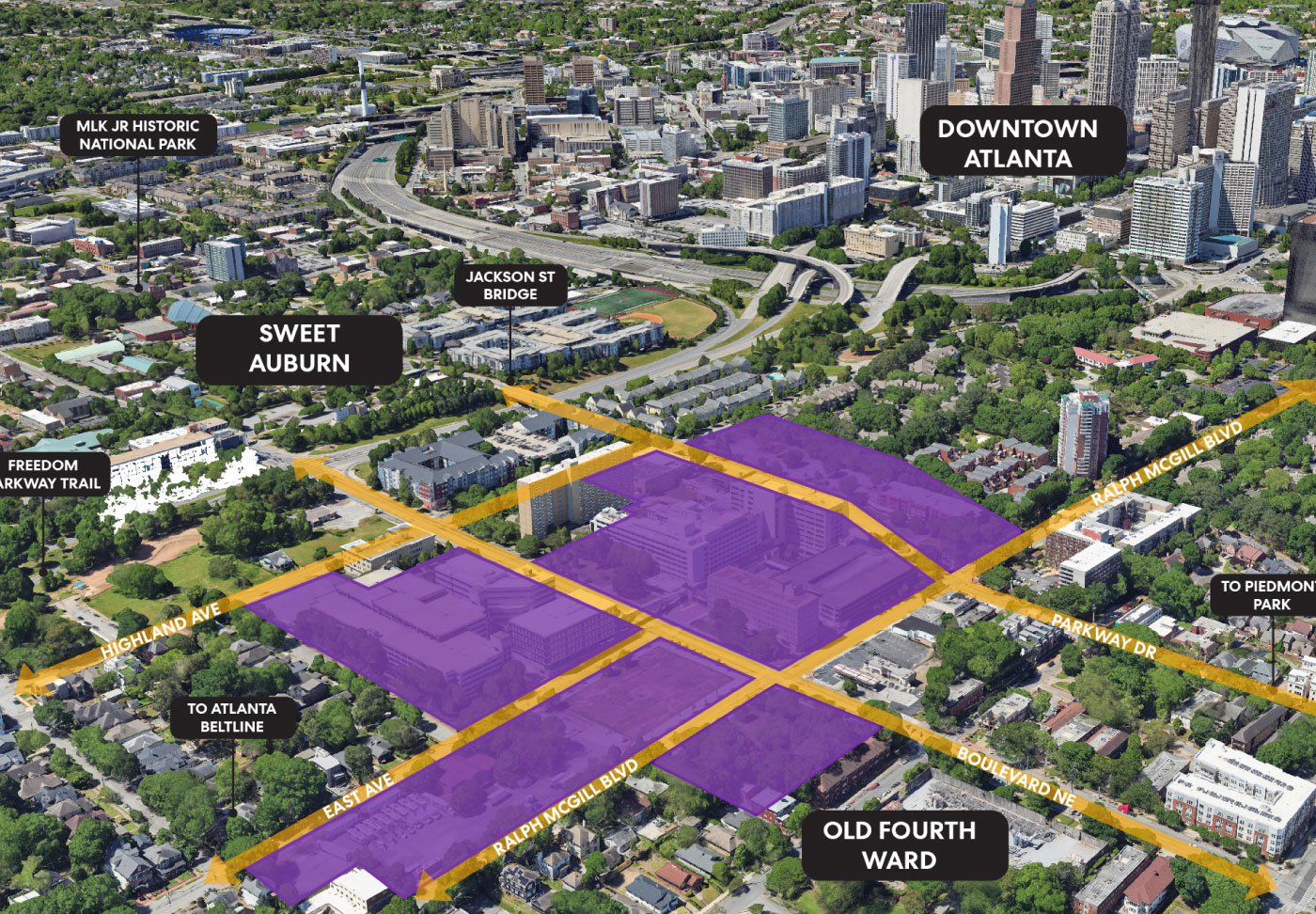
A Commitment to Community and Collaboration
The redevelopment project aligns with Wellstar’s dedication to creating healthier, more inclusive communities. The plans will reflect input from local stakeholders, ensuring the project meets the aspirations and needs of the surrounding neighborhoods. Stephen Vault, vice president of Strategic Community Development at Wellstar, shared: "By working together, we are creating a space that the community has said is important to them. This includes affordable housing, new street access and green spaces, retail and commercial businesses, and health and well-being resources that preserve the area’s rich history while embracing a vision for future growth."Environmental and Safety Stewardship
Ferma Corporation and its partners are committed to sustainability by using innovative techniques to reduce waste and implement eco-friendly practices, supporting a greener future for the community. Robust safety protocols will be implemented throughout the demolition phase to protect workers, residents, and the surrounding environment. Eric Pinckney, senior vice president at The Integral Group, added: "The demolition phase represents the groundwork for transformation. It’s not just about clearing space; it’s about building trust and ensuring the community feels engaged and heard every step of the way. Our commitment is to deliver a redevelopment that aligns with the values and aspirations of those who live and work here."A Trusted Team with Proven Expertise
The Ferma-led team was selected for their combination of technical expertise and commitment to community-centered practices and environmental responsibility. Their approach reflects a holistic focus on delivering safe and sustainable outcomes while fostering local collaboration. Key elements to their approach will include:- Expertise and Community Focus: Ferma Corporation brings decades of proven experience and dedication to practices that prioritize the needs of the local community.
- Local Economic Impact: The team emphasizes hiring and training local labor, contributing to economic opportunities and workforce development within the community.
- Minimizing Disruptions: Comprehensive measures will be implemented to manage noise, dust, and traffic during the demolition phase, reducing impacts on residents and businesses.
- Sustainability Practices: Ferma prioritizes environmentally responsible operations, ensuring materials are recycled or disposed of in compliance with local and federal regulations.
- Commitment to Safety: Safety protocols are central to their work, protecting both workers and nearby residents throughout the demolition process.
Preserving Legacy and Planning for Growth
The redevelopment will thoughtfully honor the site’s historical significance, embedding its rich cultural legacy into every aspect of the project, with particular emphasis on the design of new spaces. This intentional balance of preserving the past and embracing future growth reflects a steadfast commitment to building a meaningful, inclusive future rooted in respect for the site’s heritage.Future of the Site
The redevelopment of the former Atlanta Medical Center campus is being guided by a land-use plan unanimously approved by the Atlanta City Council with support from Atlanta Mayor Andre Dickens and the leadership of the local neighborhood association. As stewards of the property, Wellstar is committed to ensuring the redevelopment serves the needs of Atlanta while incorporating input from residents of the surrounding neighborhood. While additional planning is required to finalize specifics, Wellstar looks forward to partnering with the Mayor, City Council, the community, and other stakeholders to realize a shared vision for the site. This vision will honor the property’s historical significance while fostering new opportunities for growth, connectivity, and inclusivity.;
Wellstar patients were among the first in Georgia to benefit from an FDA-approved imaging technology that detects the extent of prostate cancer earlier and with greater accuracy than current imaging methods.
A diagnostic agent is given to patients as an injection. Once it is in the body, it binds to PSMA, or Prostate Specific Membrane Antigens. Prostate cancer cells usually have a higher level of PSMA.
When used with PET scans, this innovative technology gives physicians a clearer image of prostate cancer lesions and enables providers to determine the best course of treatment. It is the most sensitive scan available for prostate cancer.
Wellstar is among the first in Georgia to routinely offer PSMA PET scans.
While standard scans have limited sensitivity for prostate cancer, this advanced imaging is much more capable of identifying prostate cancer, which allows Wellstar doctors to determine if the cancer is limited to the prostate or if it has spread to other parts of the body.
“It allows us to make sure we’re not missing any sites of cancer that aren’t picked up with old-school imaging,” Wellstar Urologist Dr. Justin Watson said. “If there is an area of cancer outside what we’d typically treat, and we pick it up with this imaging, we can make sure we address that area, too.”
Providers can then tailor treatment to each patient’s individual needs, collaborating with the patient to find the best course of action and improve outcomes.
“This imaging helps us ensure that patients are receiving the right treatment, which improves their outcomes,” Dr. Watson said.
The new imaging technology improves upon scans that were used in the past.
“This is several leaps forward in our ability to see prostate cancer on a scan in high resolution,” Dr. Watson said. “In the older scans, things are difficult to see and sometimes not even perceptible, and with the new scans, they light right up and we know much better what we’re dealing with.”
This PSMA imaging is currently available at Wellstar Kennestone Regional Medical Center and Wellstar Cobb Medical Center, with plans to expand to other locations.
Wellstar urologists, oncologists, radiation oncologists, pathologists and radiologists work collaboratively to provide prostate cancer patients a full range of treatments to consider including active surveillance, CyberKnife/radiation therapy, surgery, hormone therapy and chemotherapy.
To learn more about prostate cancer treatment at Wellstar, visit wellstar.org/prostatecancer or call 1 (877) 366-6032.
;
From catching cancer to following through with expert care, Wellstar ensures patients never have to fight lung cancer alone.
We are dedicated to early intervention in lung cancer, which improves outcomes for patients. After detection of an abnormality on a CT scan, patients are immediately surrounded by an interdisciplinary support team devoted to their well-being.
Identifying lung cancer early
If you are at increased risk for developing lung cancer, talk to your care team about screenings. With a low-dose CT scan of the chest, it only takes a few seconds to check in on your lung health. These screenings are offered at several Wellstar imaging centers.
The United States Preventive Services Task Force has revised lung screening guidelines. Patients may qualify for screening if they are 50 to 80 years old and smoked for 20 years. If they are a former smoker, they may qualify if they quit less than 15 years ago.
“Finding lung cancer early leads to better outcomes, and screening with CT scans is recommended as the only proven way to minimize delay in diagnosis,” said Wellstar Thoracic Surgeon Dr. Daniel Fortes.
Because finding cancer and starting treatment sooner can be life-saving, Wellstar has invested in one of the nation's largest lung screening programs and an incidental nodule program. When people come into a hospital seeking care for something else—whether that be a health condition like appendicitis or a traumatic event like a motorcycle accident—they might get a scan of the abdomen or chest that also shows portions of the lungs.
Using artificial intelligence, reports of those scans are fed to report coordinators, categorized based on their risk level and if a patient is higher-risk, forwarded to nurse navigators for review. Nurse navigators consult with physicians about the findings, and Wellstar can then initiate care if cancer is suspected.
The program, which started in fall 2020, has identified a total of 203 lung cancers and 22 other types of cancer, as of November 2025.
Expert care and support at every step
From the very beginning, people with lung cancer at Wellstar are surrounded by a team of experts. Rather than go through the time-consuming process of driving to multiple appointments with different specialists, patients meet with all these physicians in one place.
The Wellstar Lung Cancer STAT Clinic—at Wellstar Cobb, Wellstar Douglas, Wellstar Kennestone, Wellstar North Fulton, Wellstar Paulding and Wellstar West Georgia Medical Centers, as well as Wellstar Cherokee Health Park and the Thoracic NOW Clinic at Wellstar MCG Health Medical Center—give patients immediate access to specialists in medical oncology, radiation oncology, pulmonary medicine and thoracic surgery.
"We plan patients’ appointments ahead of time, ordering multiple tests that will be necessary for the treatment decision-making. These can include PET scans, CT scans, MRIs and/or a pulmonary function test," Dr. Fortes said. "We’re always gaining time in the patient’s overall treatment because we are anticipating and creating a plan as a team."
Getting multiple expert opinions from the start not only gives patients peace of mind, it speeds up treatment, too. In the United States, the average time between an abnormal scan and the beginning of treatment is 60 to 90 days. The STAT Clinic reduces that time to as little as 14 days. Time-to-treatment affects long-term survival in patients with lung cancer.
"We have data to show that if we delay treatment, even in early-stage cancers, we decrease the chance of a cure," Dr. Fortes said. "The goal of the STAT Clinic is to get them the quickest we can into their final treatment plan."
High-tech surgery options
For many patients, surgery is a crucial part of lung cancer treatment. Wellstar offers several minimally invasive options, reducing recovery time for patients.
More than 90% of lung cancer surgeries at Wellstar are performed using either the Da Vinci Surgical System or Video Assisted Thoracic Surgery techniques (VATS).
Minimally invasive surgeries reduce pain, scarring, blood loss and infection, as well as time to recover—getting patients back to work and other routines quicker.
The Da Vinci system is equipped with 3D cameras and instruments that can make very intricate, precise movements, allowing for shorter incisions and more accurate surgery. Some patients can leave the hospital as early as the next day.
For biopsies, Wellstar has completed 500 procedures using the Ion system, a robotic-assisted platform.
The system uses a three-dimensional spatial recognition technology that helps guide a catheter down the airway, deep into the lung, all the way to small nodules where biopsies can be performed. The robotic catheter maintains its shape and stability throughout the biopsy process, significantly improving diagnostic yield compared to other modalities.
"The better the image and the more certainty we have of the spatial location of the catheter, the better we can avoid complications by making sure we are not too close to a blood vessel or the edge of the lung," said Dr. Fortes.
To reduce your risk of lung cancer and keep your lungs healthy, talk to your primary care team and follow a few tips, such as exercising and avoiding smoking. Learn more about treatments on our lung cancer care page.

Wellstar Paulding Medical Center is now offering device implantations and catheter ablations in a new, state-of-the-art heart care lab, expanding the hospital’s cardiology services.
If you have a heart rhythm disorder and need a permanent cardiac device like a pacemaker or defibrillator implanted, Paulding’s cardiologists now offer these procedures close to home with qualified, compassionate providers who will take the time to get to know your needs.
Your care team will continue to support you after the device is implanted, too. Your electrophysiologist will ensure your device continues to work properly and check the battery life, and you’ll be able to work with our experts to create a personalized diet, exercise, lifestyle and medication plan to keep your heart in top shape.
Paulding also offers another solution for arrhythmia—catheter ablations. During this procedure, a small tube is inserted into a blood vessel, then guided to the heart to scar areas of tissue that are causing the abnormal heart rhythm. The scars block the electrical impulses that cause the abnormal rhythm.
To make an appointment, call (678) 324-4444.
;
Wellstar now offers advanced care for people with head and neck cancer—a complex disease that is often aggressive and requires coordination amongst multiple cancer experts. The new STAT Clinic for Head & Neck Cancer opened on the campus of Wellstar North Fulton Medical Center on August 11, 2022.
People with all types and stages of head and neck cancer have access to expert care and advanced treatments that are typically only available at academic centers. Treatments available in North Fulton include complex excision and reconstruction with microvascular free tissue transfers as well as CyberKnife radiation treatments.
Technologically advanced CyberKnife care close to home
In Wellstar’s STAT Clinics—short for Specialty Teams and Treatments—patients can see multiple cancer subspecialists to be diagnosed, have questions answered and finalize a treatment plan in a single day. This reduces the need to drive to different locations and helps the patient start treatment faster.
“The concept of multidisciplinary care is tried and true and shown to be effective for cancer patients,” said Dr. Fiyin Sokoya, the head and neck cancer surgeon who co-founded the North Fulton STAT Clinic for Head & Neck Cancer. “This model decreases the time to proceed and receive care.”
First, a group of medical specialists including a head and neck cancer surgeon and facial plastic surgeon, a radiation oncologist, a medical oncologist, a pathologist and a neuroradiologist review the patient’s pathology and imaging as a group to diagnose, stage and create a personalized treatment plan.
Next, the patient and their family meet one-on-one with the head and neck cancer surgeon, radiation oncologist and medical oncologist. This is an opportunity for the patient to learn about the recommended treatments and ask questions.
“Traditionally, patients must drive to several different appointments to learn the stage of their cancer, meet with different specialists and make decisions,” said Dr. Nagender Mankan, the dedicated medical oncologist in the new STAT Clinic. “At that point, four to five weeks have gone by. In STAT Clinic, we are expediting the complicated decision-making process.”
The patient also meets with a nurse navigator. This specialized nurse helps coordinate many aspects of care for the patient including scheduling appointments and connecting patients with support team members, such as a registered dietitian, a speech therapist or a dentist who may help relieve irritation in the mouth and throat.
Why STAT Clinic is good for patients, and what to expect
When a STAT Clinic patient needs surgery, Dr. Sokoya is one of only a few surgeons in the region to perform complex excision and reconstruction with microvascular free tissue transfers.
“North Fulton has now become a destination center for head and neck cancer treatment because of our ability to offer advanced surgical care,” he explained. “The launch of this STAT Clinic is exciting, and it’s going to bring very advanced, high-level care to this area.”
Hundreds of patients travel to Roswell each year to seek Dr. Sokoya’s expertise from Georgia, Florida and Alabama.
Patients from all over the Wellstar system are seeing Dr. Sokoya for complex head and neck cancer management,” said Dr. Mark McLaughlin, a Wellstar radiation oncologist who co-founded the STAT Clinic.
Adding the new clinic allows us to invite those patients to come to North Fulton for evaluation and discussion of treatment options. Then we can work with their hometown doctors.”
Technologically advanced CyberKnife care close to home
Patients of the STAT Clinic who are candidates for radiation therapy have access to the latest CyberKnife technology at Wellstar North Fulton Cancer Center. The CyberKnife radiation suite is one of just two in the entire metro Atlanta area.
People with complex head and neck cancer such as large or recurrent tumors often benefit from CyberKnife radiation therapy. The technology minimizes radiation exposure to healthy tissue and limits side effects while shortening treatment courses. Normally patients receive five to eight weeks of radiation therapy. In many situations, they can complete their radiation course in as few as one to five treatments with CyberKnife.
“This highly advanced technology treats advanced head and neck cancers,” Dr. McLaughlin said. “You don’t have to go all the way into Atlanta.”
STAT Clinic for Head & Neck Cancer at Wellstar North Fulton Medical Center is located at 4500 Hospital Blvd, Suite 120 in Roswell, Georgia. For more information or to schedule an appointment, call the nurse navigator at (770) 751-2556.
Wellstar Health System announced a multimillion-dollar investment to bring cutting-edge radiation therapy to Wellstar Paulding Medical Center in Hiram, Georgia on November 2, 2022.
“Our motto is ‘Neighbors Caring for Neighbors’ and these new technologies will enhance access to medical care for every neighbor in Paulding County,” said Ralph Turner, Wellstar senior vice president and president of Wellstar Paulding Medical Center. “Our team is focused on providing a patient-centric experience. Having a short drive and the comforts of home and family nearby helps the healing process.”
Breaking ground for groundbreaking radiation technology
The expansion will enhance the patient experience by adding a new radiation vault to house a second linear accelerator — the technology that delivers radiation therapy — and is slated for completion in early 2023.
In the last year, patients received nearly 8,000 radiation treatments. The radiation oncology team often extended hours from 7 a.m. until 7 or 8 p.m. to accommodate patients.
During a recent press conference, a group of patients, physicians, healthcare leaders, team members, government leaders and community partners ceremonially broke ground on the major expansion of Wellstar Radiation Oncology. The facility is located on the ground floor of Wellstar Paulding Medical Center’s Outpatient Pavilion at 148 Bill Carruth Parkway in Hiram, Georgia.
The new machine will also bring a leading-edge cancer treatment called stereotactic body radiation therapy (SBRT) to Paulding County for the first time. This radiation technology uses multiple X-ray beams to treat tumors with highly precise, high-dose radiation to any location in the body, preserving surrounding tissue, organs and nerves. The technology allows patients to have significantly fewer treatment sessions.
“This is a huge step forward for cancer care for the people of Paulding County,” said Dr. William Thoms, who has served as the radiation oncology medical director for Wellstar Paulding Medical Center since 2017. “This expansion will allow people to stay in our community for more advanced treatments with shorter wait times.”
The renovation will also modernize the dressing rooms and add more space to increase patient comfort.
Wellstar Spalding Regional Hospital has begun replacing their emergency medical services (EMS) trucks with innovatively designed trucks to better serve residents in Spalding County. Easily recognizable, the first two of the bright red and white trucks with large purple lettering are now on the streets providing the latest in life-saving technologies for Spalding County, and backup emergency response care for Henry, Lamar, Butts and Pike counties.
The larger of the two EMS trucks is a tall, diesel-driven critical care vehicle equipped with advanced cardiac equipment. The truck also has the capacity to transport up to three patients at one time and is outfitted for neonatal transport. Additionally, it could be used to transport air flight crews to and from the scene and the hospital.
Both trucks feature innovative monitors and mobile hotspots to advance EMS’ use of telemedicine, linking the paramedic, physician and patient while en route to the hospital. Wellstar Spalding Regional EMS was the first to launch this webcam capacity in Georgia.
Each truck is also part of an Infectious Disease Transport Network, the only one between Atlanta and Macon. As members of this network, Wellstar Spalding Regional’s award-winning team of EMS paramedics and EMTs are specially trained and can turn either truck into an “isopod” isolation unit for emerging infectious diseases.
To reduce the number of paramedic back injuries caused by heavy lifting, the trucks incorporate new automated stretchers. These units provide support for emergency personnel by removing the need to lift a 75-pound stretcher along with the weight of the patient. This equipment is well-positioned to save EMS personnel from debilitating back injuries and lengthy rehabilitations, the number one cause of career ending disability in the EMS industry. Considered the safest in the industry, the stretchers also incorporate safety lockdowns from front to back, ensuring the patient is secure while in the truck.
Spalding Regional’s EMS paramedics and EMT’s provided input on the unique internal design to maximize efficiency and safety. For example, the trucks have been fitted with an automated lift to load and unload the large, extremely heavy, oxygen tanks that assist patients experiencing difficulty breathing. Jonathon Johnson, Director of Wellstar Spalding Regional’s EMS is proud of his team.
“Paramedics and EMT’s play a vital role in any system of care, often the first line of medical care for critical patients. This new equipment expands the safety for our patients and our personnel, and continues our long history of dedication and commitment to improvement of patient care in this community.”
Wellstar EMS is available 24/7 and responds to more than 16,500 calls annually with each truck in the fleet running between 200 and 250 hours each month. Each new truck costs the hospital between $150k and $180k. This first new critical care vehicle was purchased and outfitted through a gift from the Dundee Community Association to the Wellstar Foundation.
To keep up with the community’s high-demand, Spalding Regional has plans to replace seven additional trucks and add one more Critical Care truck to its fleet. Donations to the Foundation help. Every dollar designated to Spalding Regional funds much-needed projects that support the health and well-being of the local community. To make a tax-deductible donation, visit wellstar.org/give or call (770) 956-GIVE (4483).

Wellstar Health System has recently hit 1 million active users on MyChart. When we deployed this electronic medical record patient portal in 2015, we were the first Georgia-based health system to offer the service to patients.
Since then, MyChart has transformed the way patients interact with their healthcare information and clinical team by giving them 24/7 access at their fingertips. Patients became active participants in their care, both during their hospital stay and at home. Research shows that empowering patients to take control of their health leads to lower costs and better clinical outcomes.
MyChart’s "Open Notes" feature also allows patients to go to appointments and ask questions without having to worry about writing down information. Our physicians type up all notes and attach them to the records, allowing patients to review everything once they get home. If additional questions come to mind, patients can also ask them directly on the portal.
"I love MyChart and that I keep everything organized. What medications I'm taking, I can order them easily. I can text the doctors and Sharon at Ryan Cantwell's office, the nurse there," said Frank Ryan, who has used Wellstar to navigate through his health journey for several years.
"At Wellstar, we work as a team to take care of our patients," Wellstar Family Medicine Physician Dr. Ryan Cantwell said. "I enjoy being my patients’ quarterback and coordinating their care with other physicians. Through our electronic health records system, the referral process and communication with other specialists is easy and accurate."
That’s why Wellstar continues working on how we connect digitally with our patients to improve their experience and keep them in control of their health.
In 2018, we set the goal of reaching Epic’s top quartile for MyChart activation, which was 50 percent. At that time, the activation rate at Wellstar was 28 percent, with 420,000 patients signed up for MyChart. As of July 2022, the MyChart activation rate at Wellstar hit 65 percent.
Looking to the future, Wellstar is focusing on increasing and optimizing MyChart digital experiences, particularly around patient self-scheduling, e-Check, and MyChart bedside utilization for in-patient encounters. This high level of MyChart engagement ultimately gets Wellstar closer to our mission of providing world-class healthcare to every person we serve.
Click here to sign up for MyChart today and start taking advantage of all its benefits.
;
It’s not every day that a young man survives a nearly fatal car accident and takes a victory walk through the hospital hallways to thank his care team. After suffering a rare cricotracheal separation that left Chris LoCurto unable to effectively breathe on his own, that’s exactly what happened.
Coordinated EMS & hospital care set Chris up for survival
At 22, Chris was in a car accident that caused serious injuries he wasn’t sure he’d be able to survive. He fractured his jaw, clavicle and spine and his lung collapsed. His most life-threatening injury was a tracheal separation—his airway was cut in half.
EMS professionals arrived on the scene. Although Chris was talking and walking, they could hear something abnormal in his breathing. The paramedics coordinated care with Wellstar Kennestone Regional Medical Center so the trauma team would be assembled and ready for Chris upon arrival.
“I was trying to breathe but I wasn’t getting air,” Chris said. “Going to the hospital, I was honestly thinking I wasn’t going to make it.”
How the trauma team put Chris on the road to recovery
Led by Dr. Daniella Kington, the trauma team was waiting when Chris arrived. Immediately, they intubated him so he could breathe. They used a bronchoscope, a special camera, to see inside the airway to diagnose the injury and learn important details to plan treatment.
Chris was then put on extracorporeal membrane oxygenation (ECMO). This highly-advanced machine helps the heart, lungs or both heal after extreme trauma or organ failure.
“For Chris, ECMO supported his breathing and oxygenation during the intricate surgical repair of his trachea,” said Jamie Van Ness, MBA, BSN, TCRN, director of Trauma Services at Wellstar Kennestone.
Now a Level I Trauma Center, the hospital is one of a few in Georgia that offers ECMO.
Dr. Nelson May, a head and neck trauma surgeon, was assisted by Dr. Nicholas Mildenhall to perform Chris’ tracheal repair. The surgery required the surgeons to reattach Chris’ larynx to his trachea. Then they placed a tracheostomy tube so Chris would be able to breathe, swallow and talk again.
To allow his airway to heal, Chris was sedated for a few weeks. When he woke, his injuries had been treated but he was fighting pneumonia. He was transferred to intensive care and his condition improved within a week.
Throughout his time in the hospital, Chris received the right treatment at the right time thanks to Wellstar’s multidisciplinary approach to care.
“Coming to Wellstar Kennestone made a difference in Chris' outcome,” said trauma surgeon Dr. Ginger Justice, a physician who got to know Chris on her daily rounds. “He came to a trauma center that had all the resources to care for him—pretty much from the moment he hit the Emergency Department to discharge.”&
Providing specialized trauma care
When Chris was a patient, all the specially trained doctors and advanced technology were available to help him recover from his life-threatening injuries. Shortly after, Wellstar Kennestone was verified by the American College of Surgeons as a Level I Trauma Center, the highest level of trauma care offered.
“The first and most crucial piece [to Level I Trauma Center verification] is that we have all the different subspecialists available in one place to provide full care for our patients,” Dr. Kington said. “If a patient comes in, no matter where they’re injured, we have a subspecialist who can help with all those different injuries.”
That was exactly what Chris needed. In addition to helping people get trauma care fast, Wellstar Kennestone is home to a residency program, training the next generation of trauma doctors.
For about a month and a half, Chris recovered in the trauma unit, ICU and intensive inpatient rehabilitation. In Wellstar Kennestone’s inpatient rehab, specially trained speech, occupational and physical therapists create a specialized care plan to help each patient achieve their goals and get back to living life.
Compassionate nurses made a lasting impact on Chris
While the trauma team saved his life, Chris credits his nurses with keeping him motivated.
“Every nurse I met who came in, we ended up forming some sort of relationship,” Chris said. “They took care of me like their own. That’s not in their job title, nobody asked them to do that, which is why I’m so grateful. They went above and beyond what they get paid to do to make me better physically and mentally.”
For example, one nurse found out about Chris’ love of aviation and brought him to see an air ambulance helicopter. Another nurse shared his love for hunting and planned a reunion for Chris and his hunting companion, his dog Maddux.
“While the future was kind of unforeseen, the nurses connected with me,” Chris said. “I got to spend some time with my dog too. It was huge for my mental well-being.”
Coming back to say thanks
Chris defied the odds by walking, talking and being able to eat. Today, he’s taking steps toward a full recovery. While learning to live with a tracheostomy tube, he’s working out and increasing his cardio exercise. He spends a lot of time walking Maddux.
“I’m slowly introducing myself to normalcy again,” he said.
A crucial part of recovery was visiting the hospital and saying “thank you” to his care team.
“He and his family walked in,” Dr. Justice remembered. “I saw Chris in normal street clothes, walking with his sunglasses on. He said, ‘Hey, I’m doing great!’ To see this young man with so much potential have a good outcome was very inspiring.”
Chris made sure to thank as many care team members as possible. “Their motivation and drive to get me going is without a doubt one of the reasons I’m moving around as good as I am today,” he said.
Dr. May added, “It was gratifying to see the real-life implication of Chris’ care and to be able to participate in getting him to where he is today.”
A bright future thanks to expert trauma care
Overall, without the first-rate trauma response of Chris’ medical team at Wellstar Kennestone, he would not be where he is today—back in the wilderness with Maddux.
“The coordination of many different teams and doctors with different areas of expertise in different phases of his care allowed him to be where he is today,” Dr. May said.
Wellstar Kennestone provided the advanced care Chris needed with excellent trauma services. Now with a Level I Trauma accreditation, the trauma team can keep offering advanced care—and preparing the physicians of the future to do the same.
Learn more about Trauma Care at Wellstar.
;

As the weather starts to warm and flowers bloom, spring is in the air – and so is pollen.
If you deal with frustrating symptoms like a stuffy nose, sneezing or watery eyes, you’re not alone. Each year, more than 50 million people in the United States have allergies, according to the Asthma and Allergy Foundation of America.
Wellstar knows every Achoo! can impact your daily life, making it difficult to enjoy outside activities with family and friends. Instead of sitting on the sidelines, you can use simple strategies to take control of your seasonal allergies.
Tips to Relieve Seasonal Allergies
Seasonal allergies are your immune system’s response to certain environmental triggers, such as pollen from trees, grass or flowers. Your body’s reaction to these allergens can include coughing, sneezing, runny nose, red or itchy eyes, throat irritation and post-nasal drip.
By playing it smart and planning ahead, you can take steps to relieve your allergy symptoms. Follow the helpful tips below to say goodbye to seasonal allergies:
• Masks make a cool accessory. Wearing a mask can not only keep others safe from COVID-19, but also prevent you from breathing in pollen and other allergens.
• Try over-the-counter medications. Consult your Wellstar provider about common allergy remedies like antihistamines and nasal spray.
• Check the weather report. Avoid outside activities on days that are dry, windy or have a high pollen count of 1,000 or more.
• Don’t invite allergens inside. Keep windows and doors shut to prevent pollen from blowing into your home and contaminating surfaces.
• Stay on top of spring cleaning. Dust and vacuum often to remove potential allergens, such as dust, dander and pollen.
• Don’t forget your four-legged friends. Be sure to wash or brush your pets more often to remove loose fur and dander.
Expert Care for Allergies
When at-home remedies aren’t enough, Wellstar Allergy & Immunology is ready to care for you. If your symptoms are severe, you may need specialized treatment for allergies or be dealing with a chronic condition, such as asthma.
At Wellstar, we diagnose and treat a full range of adult and pediatric allergy conditions. Our allergists will partner with you to create a personalized care plan, which may include allergy shots, prescription medication or other therapies.
Don’t sneeze or sniffle through another season. Wellstar provides the world-class, tailored allergy care you need at convenient locations across metro Atlanta.
Click the “Book Now” button at the top of any page to schedule an appointment.

Wellstar Health System and Colquitt Regional Medical Center are launching a new residency track to train obstetrics and gynecology (OB/GYN) physicians in Marietta and Moultrie. The program is unique in that it will provide new physicians with the opportunity to train in both suburban and rural areas of Georgia.
Known as Graduate Medical Education (GME), Wellstar Kennestone Regional Medical Center's OB/GYN residency program has been approved for a rural track at Colquitt Regional in Moultrie. This rural track expansion will ultimately grow to a complement of four OB/GYN residents training on-site at Colquitt Regional at one time. Each resident physician in training will spend time at Wellstar Kennestone in Marietta, but the majority of their training will be completed at Colquitt Regional.
“This program will create opportunities for physicians specializing in women’s and maternal health to train and build their careers in rural Georgia,” said Colquitt Regional President and CEO James Matney. “It’s wonderful how Wellstar is reaching out to other health systems to help meet our local needs. Our community is encouraged and appreciative that Wellstar is helping train physicians who will care for people in rural areas across the state.”
Georgia currently ranks among the worst states in the nation for maternal care. According to the March of Dimes, more than one-third (34.6%) of Georgia counties are maternity care deserts and do not have a single obstetric healthcare provider. Additionally, Georgia is higher than the national average for maternal mortality and inadequate prenatal care. However, many maternal deaths are preventable by improving access to care.
Since 2015, 66% of physicians in training at Colquitt Regional have stayed in and near Moultrie to build their careers with residency programs that include Family Medicine, Psychiatry and General Surgery. Wellstar and Colquitt Regional aim to improve access to women’s health and maternal care in South Georgia through the new residency program.
“We have a shared goal of improving the health and wellness of every person in Georgia. This new program is another step toward meeting the critical need for physicians in rural Georgia,” said Wellstar President and CEO Candice L. Saunders. “Doctors are more likely to stay in communities where they train, which makes partnerships among health systems like Wellstar and Colquitt essential to our success.”
Including its partnership with Augusta University’s Medical College of Georgia (MCG) at Wellstar MCG Health Medical Center, Wellstar operates five teaching hospitals in the state—Wellstar Kennestone, Wellstar Cobb, Wellstar Douglas and Wellstar Spalding Medical Centers. Wellstar recently announced that its Wellstar Paulding and Wellstar West Georgia Medical Centers are also becoming designated teaching hospitals.
“Becoming a physician is an extremely rewarding experience, and that’s magnified in rural areas,” said Dr. Val Akopov, senior vice president of Wellstar Medical Group. “The physicians who train in this new program will see and feel the joy of working in a rural community.”
“Meeting the needs of people in South Georgia has always been our mission,” said Dr. Daniel York, director for OB/GYN residency at Colquitt Regional. “Our new women’s health program will go a long way to providing our region with qualified physicians in rural areas. We have enjoyed working with Wellstar to get this program approved.”
In the last decade, Wellstar has grown its GME program from 14 trainees in 2016 to nearly 300 today, many of whom have remained with Wellstar and in Georgia. Through Wellstar’s partnership with Augusta University’s Medical College of Georgia, Wellstar MCG Health is the primary clinical training site for more than 500 GME positions. With the new residencies, Wellstar will support more than 860 physicians in training.
;
Some things are just better together: Peanut butter and jelly. Popsicles and summer days. Stethoscopes and superheroes. When it comes to your child’s health, there’s no better combo than your love—and our expert pediatric care. That’s why Wellstar Children’s of Georgia is here to partner with your family.
Our name and logo may have changed, but the mission to care for children, teens and your family remains the same.
“Our new name represents a powerful collaboration, bringing together more pediatric specialists in Georgia to create a comprehensive system of care,” said Wellstar Children’s Hospital of Georgia Pediatrician-in-Chief Dr. Valera Hudson.
Where kids’ healthcare is “better together”
At Wellstar Children’s of Georgia, a child’s health is strengthened by a partnership between parents and pediatric specialists. Our physicians and advanced practice providers listen and get to know each child from the moment they’re born into young adulthood, collaborating with parents to deliver tailored care.
“We never forget that you know your child best—from their unique needs to what makes them tick,” said Wellstar Chief Pediatrics Officer Dr. Carrie Stinson. “We trust your instincts, and we’re here to support you as you help your child grow into a healthy, well-prepared and incredible human being.”
A checkup for every child, from toddlers to teens
Every kid should have a well-child exam each year. “When you have babies and toddlers, it’s routine—you’re scheduling these frequently,” said Dr. Stinson. “But when kids get older and busier, these visits may fall off your radar.” Staying on top of these vital checkups helps keep focus on your child or teen’s well-being, including their physical health and development as well as their emotional, social and behavioral health.
Navigating life’s most challenging moments
During visits to Wellstar Children’s of Georgia, pediatricians, pediatric specialists, nurses and other dedicated team members use the latest technology and innovative therapies to treat common illnesses and complex conditions. In our Pediatric Emergency Departments and imaging centers, specially trained Child Life Specialists aid children and their families during challenging healthcare moments—helping them understand and cope with unfamiliar or scary situations.
A long legacy of care
Our new name builds on a rich history of pediatric excellence throughout Georgia. For decades, we’ve worked hard to make sure our communities have access to the pediatric care they need—from preventive care to emergency care and specialty care, including cardiologists, neurologists, urologists, ENTs, orthopedics, therapists and more.
Care in Augusta
Wellstar Children's Hospital of Georgia in Augusta has been a leader in the state for nearly 30 years. We’re home to:
- Pediatric primary care and specialty care
- A 24/7 Pediatric Emergency Department
- A dedicated Level II Trauma Center
- A Level IV Neonatal Intensive Care Unit (NICU)
- The only Level I Pediatric Intensive Care Unit (PICU) in the region
- A Level IV Epilepsy Center
- One of two Pediatric Cystic Fibrosis Centers in the state
- Clinical trials for a variety of childhood conditions
- Summer camps and support programs for children with specific health conditions
Care in Metro Atlanta
Our communities in the Atlanta area have access to:
- Pediatric primary care and specialty care
- Pediatric Emergency Departments at Wellstar Cobb, Wellstar Douglas, Wellstar Kennestone and Wellstar Paulding Medical Centers
- An Inpatient Pediatric Unit at Wellstar Kennestone in Marietta
- Level III NICUs at Wellstar Kennestone and Wellstar Cobb
- Level II NICUs at Wellstar Douglas and Wellstar North Fulton Medical Centers
- Wellstar Children’s of Georgia Pediatric Center in Kennesaw offering a range of high-quality, child-centered services
Care in West Georgia
In West Georgia and central West Georgia, families can access:
- Pediatric primary care in LaGrange
- Level II NICUs at Wellstar Spalding Medical Center in Griffin and Wellstar West Georgia Medical Center in LaGrange
Our growth chart: how we’re keeping up with your kids
As you measure your child’s growth, we’re growing too! We continue to invest in our teams and facilities across Georgia so your child can have a healthy future.
In Metro Atlanta, Wellstar continues to grow care for Cobb County’s youngest residents. A new tower at Wellstar Kennestone, slated to open spring 2026, will feature an expanded NICU with more beds to meet the needs of our families.
In Augusta, Wellstar Children's Hospital of Georgia has unveiled a welcoming and fresh child-friendly lobby. Families visiting the campus will soon benefit from the addition of the Kisner Foundation and Friends Center for Pediatric Behavioral Health and Wellness. This new space brings neurology and psychology services together under one roof, providing a dedicated place for families to find help for their children's behavioral health needs.
"We’re passionate about caring for kids,” said Dr. Hudson. “Our dream is to get beyond just treating and intervening when there’s a crisis—we aim to help families thrive.”
Whether preventing illness or treating chronic conditions, Wellstar Children’s of Georgia is committed to helping children heal so they can do more of what they love.

By Christen Miller, Wellstar registered dietitian
In the ever-evolving world of diet and wellness, social media has become a breeding ground for the latest health food fads. As a registered Wellstar dietitian with experience helping hundreds of people lose weight and keep it off, my goal is to help you cut through the internet noise and develop a clean, balanced diet. So, without further ado, here are the 5 most popular health food fads and 5 corresponding tips to help you eat better than ever.
1. Juicing
When you put fruits or vegetables into a juicer, you’re left with a liquid that contains most of the vitamins, minerals and plant chemicals found in those foods. If you’re someone who really doesn’t enjoy eating fruits and vegetables, then juicing is a good way to add those foods to your diet. However, there are downsides to juicing. Whole fruits and vegetables are packed with healthy fiber, which is lost during the juicing process. Fiber plays a big role in digestive health, so my recommendation to juicers is to consider putting your fruits and vegetables into a blender rather than a juicer. Blending still delivers all the vitamins and minerals of the fruit or vegetable while preserving the dietary fiber your stomach needs to run smoothly.
2. Mushroom coffee
It might seem like a niche beverage, but mushroom coffee has exploded in popularity in the last few years. Typically, these products contain a mix of ground mushrooms and ground coffee beans. Marketers of these products make numerous claims regarding their health benefits, including stress reduction, reduced inflammation and better sleep. While it’s true that the adaptogens found in mushrooms may help achieve these effects, it’s important to note that the benefits are largely unproven. If you consume mushroom coffee and feel that it is beneficial, continue to enjoy it. This product, however, can be difficult to process, particularly if you have kidney or digestive issues. An alternative option is to simply enjoy fresh mushrooms added to meals and snacks instead.
3. Keto diet
Whether it’s on the internet, on a podcast or from a friend, almost everyone has heard about the keto diet. At a high level, the keto diet is a high-fat, low-carb diet designed to switch your body from using glucose (produced by carbohydrates) to using ketones (produced from fat) for energy. Typical foods consumed on the keto diet include things like eggs, avocados, salmon, butter, nuts (such as walnuts and pecans), low-carb veggies (like broccoli, spinach and kale) and unprocessed cheese. While there’s still not enough long-term data to conclusively say the diet is safe over a long period, it has produced great results for overweight or diabetic patients. This approach to food can help get your body out of metabolic crisis and into a healthier state. If you’re considering trying the keto diet, my recommendation would be to consult with your healthcare provider before doing so. They can make you aware of potential medical risks, so you can make an informed decision.
4. Ginger shots
Despite the spicy taste of ginger shots, many people consume them to reap the root’s many health benefits. Perks of consuming ginger include helping with digestion and reducing inflammation, thanks to the active ingredient gingerol. There's some evidence that it can improve insulin sensitivity, helping to stabilize blood sugars, and it may even help to reduce cholesterol levels. Despite these benefits, one should still be mindful about this product. Ginger is known to cause heartburn in some people. If you're prone to heartburn, dilute ginger juice to help prevent this side effect. Additionally, if you already take a ginger supplement, there's no need to also take ginger shots. Consuming too much ginger may cause nausea and gastric reflux.
5. Collagen supplements
Collagen is one of the most universal protein sources in the body. It's a major component in our hair, skin, cartilage, tendons and even our bones. Recently, collagen supplements have risen to the top of many people’s daily wellness routines, thanks to their purported skin, hair and nail benefits. While the effectiveness of topical collagen skin creams and serums is doubtful, oral collagen supplements may actually be beneficial. Research is limited yet some studies have found that oral collagen supplements produce substantive improvements to skin elasticity as well as joint mobility. There are, however, notable conflicts of interest with many of these studies, given that most are funded, in some part, by related industries.
While social media can be a valuable source of inspiration, it's crucial to approach health food fads with a discerning eye. There's no one-size-fits-all solution to nutrition and balance is key. As a dietitian, my advice is to prioritize whole, minimally processed foods, tailor your choices to your individual needs and, when in doubt, seek guidance from a qualified nutrition professional. To schedule an appointment with an expert, visit Wellstar Center for Best Health, where you’ll find customized plans for childhood and adult obesity, diabetes management, cardiovascular disorders and so much more.
Christen Miller completed her dietetic internship at Life University and has more than 10 years of experience as a dietitian. She currently serves as a bariatric dietitian with Wellstar.

Wellstar’s social media content, and all related media, are provided for educational and informational purposes only and does not constitute providing medical advice or professional services. Consult a physician for the diet that’s best for you.

According to a Modern Healthcare analysis of data from 255 health systems, Wellstar Health System provides the second-highest percentage of charity care among large nonprofit U.S. health systems. The rankings are based on a review of charity care reported as a portion of operating expenses for fiscal year 2022[1].
Wellstar devoted 6.11% of its operating expenses to charity care, making the system the top provider of charity care in the state and the second nationwide. As a nonprofit healthcare system, Wellstar is committed to bringing expert, compassionate health services to those who need them.
“Wellstar is committed to providing compassionate, expert care to the communities we serve,” Julie Teer, SVP and President of Wellstar Foundation, said. “As a nonprofit health system, we rely on the generosity of donors and strategic partnerships to help us expand access and impact. The Wellstar Foundation is the philanthropic arm of the health system and is fueling innovation and action to address the state’s most pressing health needs.”
Our nine safety net hospitals[2] care for every patient that comes through our doors, regardless of their ability to pay. Wellstar intentionally focuses on philanthropy and partnerships that support health equity, behavioral health, innovation, workforce development and clinical excellence initiatives. Each is critical to the health system’s efforts to provide holistic, tailored care that meets people’s health needs at every age and stage.
As we lead the way to a healthier Georgia, Wellstar is the only health system in the state with an established Center for Health Equity. The Wellstar Center for Health Equity (WCHE) is critical to reaching underserved communities. Every three years, a Community Health Needs Assessment is conducted to help better understand the unique health needs of the communities we serve – further enabling us to create and implement a plan to improve care and promote healthy lifestyles for every person regardless of their race, gender, culture or income.
“We are able to reach a broader range of people in need because of the partnerships we’ve formed,” Elise Lockamy-Kassim, AVP of the WCHE, said. “As a community, we are stronger together. Working with organizations like Goodr; Wholesome Wave Georgia; Healthy Mothers, Healthy Babies; Ser Familia, and hundreds of other partners, we’re able to make a much greater impact.”
Food insecurity is one of Wellstar’s six strategic initiatives because of the WCHE’s findings. Wellstar and the Wellstar Foundation first partnered with Goodr in 2020 to tackle food insecurity during the pandemic. Our partnership initially focused on Mobile Markets, pop-up grocery markets that provide food and fresh produce to thousands of families each year.
The partnership has evolved to also include a Surplus Food Recovery service where leftover food from hospitals and donated to community-based organizations. Most recently, the system launched an Organic Recycling Program with support from Goodr, the Wellstar Foundation, Catalyst by Wellstar and Wellstar Strategic Community Development.
At Wellstar, our strong commitment to clinical and community initiatives, designed to help enhance care and create a healthier Georgia, has recently grown with the addition of Wellstar MCG Health and Children’s Hospital of Georgia.
Please consider supporting Wellstar’s nonprofit work by making a tax-deductible donation through the Wellstar Foundation at wellstar.org/give.
[1] Source: Merritt Research Services, an Investortools Company
[2] Source: Georgia Department of Community Health, Safety Net Hospitals (2019 Data Year)

Augusta University Health System (AUHS) has signed a letter of intent with Wellstar Health System to form an innovative new partnership that would expand Augusta University’s educational and research missions and allow Wellstar Health System to create a broader affiliation with the university’s Medical College of Georgia (MCG) as AUHS joins the Wellstar Health System.
The potential partnership is the culmination of a thoughtful and deliberate process begun in 2019 by AUHS, its governing board and Augusta University to strategically grow MCG while expanding and improving both patient care and Georgians’ access to health care services across the state.
The proposed partnership would innovate clinical care, training and research while adopting a successful model of bringing together community-based health systems and academic medical centers such as MCG and its teaching hospitals. MCG and Augusta University are part of the University System of Georgia (USG), and MCG serves as the only public medical school in the state.
“AUHS, Augusta University and the Wellstar Health System have a shared mission to solve Georgia’s health care challenges,” USG Chancellor Sonny Perdue said. “By joining forces and working together, we can leverage Wellstar’s clinical platform and leading-edge systems to support patients while providing more opportunities for students to learn, train and care for residents in local communities across Georgia.”
Pending a definitive agreement and regulatory approval, the partnership would focus on three strategic initiatives:
- Expanding digital health offerings to create more convenient access to care and provide more individualized care regardless of location.
- Growing the pipeline of physicians and other health care providers serving Georgia by increasing the number of students who train and conduct research through MCG.
- Developing new treatments, innovative care offerings and scalable care models to optimize the health and well-being of every patient.
“By bringing Augusta University Health System together with Wellstar Health System and leveraging our respective strengths, we would improve the health of the community, address social determinants of health and expand access to quality care for all Georgians,” said Candice L. Saunders, FACHE, president and chief executive officer of Wellstar Health System.
While there are aspects of the proposed partnership yet to be determined, the partnership would likely result in significant investments to improve existing healthcare facilities and to expand access to care across the state, including a new hospital and medical office buildings in Columbia County.
“Providing health care has never been as dynamic and complex as it is today, and this partnership with the Georgia-based, not-for-profit Wellstar Health System would enable us to extend our mission of improving health through excellence in patient care, education and research for the benefit of Georgians,” said Brooks A. Keel, PhD, acting chief executive officer of Augusta University Health System and president of Augusta University.
Through an expanded affiliation with the university’s Medical College of Georgia, the partnership would address the need to train more physicians and address a growing statewide shortage. With 60 percent of MCG graduates entering a primary care residency, training more physicians in these disciplines would support increased access to frontline care provided by specialists such as family medicine physicians and general pediatricians, especially in underserved areas of the state.
A new teaching campus in Atlanta at Wellstar Kennestone Hospital could also be established under the proposed partnership. As a result, MCG, which already has the ninth-largest freshman medical school class in the nation, would grow to become one of the largest public medical schools in the country.
“With our entire nation facing a physician shortage and our state typically ranking about 40th in the number of physicians per capita, educating the next generation of physicians is more critical than ever,” said David Hess, MD, dean of the Medical College of Georgia and executive vice president of medical affairs and integration at Augusta University. “I’m excited about the partnership with Wellstar, since it will enable our students and residents to continue to learn from some of the most highly qualified physicians and other health care professionals in the state while allowing MCG to expand its contributions to improving public health in Georgia especially in more rural regions.”
EMPTY DATA SET CURATED LIST /ENABLED PAGINATION-vertical -limit-8
For a child, going to the hospital can be scary. That’s why Wellstar Douglas Hospital’s new $5.7 million Pediatric Emergency Department (ED) offers a kid-friendly and kid-sized experience for Douglas County’s youngest patients. The nautical-themed 7,600 square-foot facility provides specialized care for children from birth to 18 years of age.
The world-class “just-for-kids” facility has a separate entrance and waiting room from the main Emergency Department and is currently open from 11 a.m. to 11 p.m. The ten treatment rooms feature child-sized furniture, equipment and supplies.
“We created an environment that is optimum for healing and that helps our youngest patients feel as comfortable as possible,” said Dr. Avril Beckford, chief pediatric officer, Wellstar Health System. “Children in Douglas deserve to see doctors and nurses who understand them. We also wanted to give parents a state-of-the-art facility staffed by pediatric physicians close to home – there is no need to travel long distances with a sick child now, because this specialized facility is right here, in the Douglas County community.”
A deeper dive into kid-friendly care
Staffed by kid-friendly nurses and skilled providers devoted to children, the new kids’ ED is a result of collaboration between the architect, construction firm and pediatric experts. Wellstar’s pediatric team cares for children at more than 114,000 emergency visits a year across Wellstar’s hospitals.
“From the outside, there are colorful floor-to-ceiling glass windows,” Dr. Beckford said, as she imagined a child’s first impression. “It feels almost like you’re walking into an aquarium.”
Inside the pediatric ED, children and their parents are greeted by warm staff members, soothing murals of ocean life, a large flat screen TV and child-sized furnishings.
To help children be seen and treated more quickly, some rooms will be dedicated to patients with less serious conditions – such as sore throats and sprains. There will also be a trauma bay and a dedicated room for adolescent gynecological concerns.
;
For the first time, people in Paulding County and nearby communities have access to leading-edge robotic surgery close to home. Wellstar Health System launched a new robotic surgery program at Wellstar Paulding Medical Center.
“We’re thrilled to offer access to game-changing da Vinci robotic surgery at Wellstar Paulding Medical Center for the first time in history,” said Ralph Turner, Wellstar senior vice president and president of Wellstar Paulding Medical Center.
Robotic technology enables surgeons to make highly precise incisions smaller than the human hand can make — as tiny as a keyhole. As a result, people who have robotic surgery typically experience less blood loss, recovery pain and scarring.
“Robotic surgeries are minimally-invasive, which typically means shorter hospital stays and faster recoveries,” said Dr. Beau Dusseault, a urologist who leads the robotics program at Wellstar Paulding Medical Center.
He performed the first robotic surgery at the hospital, assisted by the $1.8 million da Vinci Xi Surgical System, on August 22. Dr. Dusseault has performed more than 440 robotic surgeries for prostate cancer and urinary tract conditions.
Experienced urologists and general surgeons are the first to offer robotic surgery at Wellstar Paulding Medical Center, primarily treating:
- Cancers such as prostate, kidney and bladder cancers
- Conditions in the kidneys, bladder and urinary tract
- Hernias and other conditions that require general surgery
The surgical team named the robot “Rosie,” a reference to the robotic maid from the 1960s sitcom “The Jetsons.” It is one of 14 robotic systems patients can benefit from at nine Wellstar locations.
“While our robotic surgery program is new to Paulding, we have high-volume robotic experience that we are bringing from the other Wellstar hospitals,” Dr. Dusseault added.

The system continues to build on its legacy and commitment to serving communities by actively listening to best understand and respond to what consumers want, need, and expect from their healthcare provider.
“As a leader in healthcare, we must take action to meet the evolving needs of people and communities. Health equity connects to everything we do, and recognizing hardships, disparities, and inequities is just the first step,” said Candice L. Saunders, president and CEO of Wellstar Health System. “Through strategic partnerships and programs, Wellstar is committed to supporting people and communities to make a tangible and lasting difference, enhancing the health and well-being of everyone we serve.”
Wellstar Center for Health Equity addresses community needs at a grassroots level
The Wellstar Center for Health Equity (WCHE) – an extension of Wellstar’s long history of community engagement and allyship to provide people-centric care – was formed to drive lasting change at a grassroots level. The six areas of focus were informed by Wellstar’s triennial Community Health Needs Assessment (CHNA) of 2019: Primary Care, Behavioral Health, Food Insecurity, Suicide, Cancer, Women’s Health.
Each of these strategic domains connects to Wellstar medical service lines to bring to bear the deep expertise and broad bench of resources needed to identify pertinent needs, relevant partnerships, and viable programs.
To create meaningful impact, Wellstar has forged strategic partnerships with government agencies, businesses, philanthropies, non-profit organizations, academia, and citizens. Examples of how WCHE has activated resources in the community include:
Walk-up, pop-up family COVID-19 testing: With the support of community partners, Wellstar conducts free walk-up, pop-up family testing at churches and school lunch pick-up sites and distributes safety kits in English and Spanish. To-date, WCHE has orchestrated 29 pop-up testing sites, administered over 3,000 COVID tests, and distributed more than 51,000 wellness kits with culturally and linguistically appropriate safety information.
Reaching faith-based congregants with vital information and vaccines: WCHE is hosting a series of community town halls to debunk myths about COVID-19 and vaccines in partnership with the Wellstar Congregational Health Network. In April, WCHE hosted a Hispanic town hall to address community questions and launched a series of equity-centric and language-proficient vaccination clinics for congregants at faith-based organizations.
Providing nutritious meals to food-insecure communities: In partnership with Goodr, an organization that provides food resources for people in need, and funded in part by Wellstar Foundation donations, the WCHE “Mobile Market” hosts “pop-up” farmers’ markets in seven communities, feeding over 700 families monthly.
Enabling technology-driven community health transformation: WCHE launched a year-long initiative to enhance access to medical care via technology with leading community partners. Supported by contributions to the Wellstar Foundation, the “Community Health Transformation” program enables the following community organizations to reach, engage, and support at-risk individuals with measurable results: Bethesda Community Clinic; Empowerment Resource Center; Healthy Mothers, Healthy Babies Coalition of Georgia; Good Samaritan Health Center of Cobb; and MUST Ministries.
Anchoring vulnerable patients with vital healthcare resources: When the Centers for Disease Control and Prevention (CDC) reported that 80% of COVID-19 patients in eight Georgia areas were Black people, WCHE developed “Anchoring Vulnerable Patients,” a project in Clayton County to assess and address the medical and social needs of Black patients with co-morbidities that put them at risk for contracting COVID-19.
;
For the first time, people in Paulding County and nearby communities have access to leading-edge robotic surgery close to home. Wellstar Health System launched a new robotic surgery program at Wellstar Paulding Medical Center.
“We’re thrilled to offer access to game-changing da Vinci robotic surgery at Wellstar Paulding Medical Center for the first time in history,” said Ralph Turner, Wellstar senior vice president and president of Wellstar Paulding Medical Center.
Robotic technology enables surgeons to make highly precise incisions smaller than the human hand can make — as tiny as a keyhole. As a result, people who have robotic surgery typically experience less blood loss, recovery pain and scarring.
“Robotic surgeries are minimally-invasive, which typically means shorter hospital stays and faster recoveries,” said Dr. Beau Dusseault, a urologist who leads the robotics program at Wellstar Paulding Medical Center.
He performed the first robotic surgery at the hospital, assisted by the $1.8 million da Vinci Xi Surgical System, on August 22. Dr. Dusseault has performed more than 440 robotic surgeries for prostate cancer and urinary tract conditions.
Experienced urologists and general surgeons are the first to offer robotic surgery at Wellstar Paulding Medical Center, primarily treating:
- Cancers such as prostate, kidney and bladder cancers
- Conditions in the kidneys, bladder and urinary tract
- Hernias and other conditions that require general surgery
The surgical team named the robot “Rosie,” a reference to the robotic maid from the 1960s sitcom “The Jetsons.” It is one of 14 robotic systems patients can benefit from at nine Wellstar locations.
“While our robotic surgery program is new to Paulding, we have high-volume robotic experience that we are bringing from the other Wellstar hospitals,” Dr. Dusseault added.

Atlanta Medical Center (AMC) has proudly served the community with compassionate healthcare for more than 100 years. It’s a legacy of service and success spanning its years as Tabernacle Baptist Infirmary, Georgia Baptist Hospital and AMC, and at Wellstar, we are honored to have been part of this story.
We understand and share the community’s disappointment that the hospital has closed as of November 1. While the decision may have felt abrupt, it came after an exhaustive search where a national consulting firm identified a number of potential partners. However, after learning more about AMC’s infrastructure and finances, none were willing to move forward. Discussions with state, local and community officials also offered no alternate paths forward.
Throughout the transition, we have remained focused on supporting our AMC patients and team members. Because our top priority is ensuring patient safety, we worked to thoughtfully wind down services in advance of the closure, including safely transferring the few remaining patients to other appropriate Wellstar hospitals and connecting with partners to ensure people receive the care they need.
We are deeply grateful to the hundreds of AMC team members and clinicians who have worked hard to ensure a successful transition and for their many years of service at AMC. We are honored that nearly 75% of our more than 1,780 offers to AMC team members for new positions have been accepted, and we are grateful they will continue in their shared pursuit of Wellstar’s mission and vision. Now that the hospital has been safely closed, Wellstar will continue to secure and maintain the facility and begin a thoughtful process to determine what is next for the site.
The challenges we faced at AMC were multi-faceted and included the age of AMC’s buildings, patients using less than half of the bed capacity, lack of public support while caring for communities most in need of whole-person wellness offerings such as primary and preventive care. Compounding these issues were the intense financial pressures facing hospital systems across the country. Like many of our peers, we felt the pain of the end of government pandemic aid and the skyrocketing costs of supplies and labor. The needed investment to address these challenges was simply too great for Wellstar alone.
As we look ahead, Wellstar will continue to build lasting partnerships that will provide people with increased access to the care they need. As the largest provider of uncompensated care in Georgia, we are proud to serve 1 in 6 Georgians in diverse communities across the region. We will continue to be there for those who need us for primary and specialized care and through our critical role in the statewide collaborative trauma network.
Through our recently announced partnership with Southside Medical Center, Wellstar will invest $5 million in Southside’s East Point clinic to expand their size and capacity and provide greater access to much-needed primary and preventive care, among other services. This is the latest example of our long-standing commitment to partner with others to provide ongoing care to the AMC community.
Our vision for the future requires collaboration with mission-aligned partners and with our friends and neighbors in our communities. That includes partners within and beyond the healthcare industry who can bring unique ideas and perspectives to support the health of the whole person, address the social determinants of health and expand access to world-class care when, where and how people need it. Together, we can transform healthcare to support the people we serve throughout their health and wellness journeys — not just when they are sick or injured. We can build the bold future of care Georgians need and deserve.
Candice L. Saunders, FACHE, is the president and CEO of Wellstar Health System, one of the largest and most integrated health systems in Georgia. A former critical care nurse, she leads nearly 25,000 team members and physicians overseeing the health and well-being of communities throughout the state.
O. Scott Swayze, MD, is the chair of the Board of Trustees for Wellstar Health System. He is an accomplished orthopaedic surgeon, practicing at Pinnacle Orthopaedics and belonging to local, state and national orthopaedic associations.


Building on a rich history of innovation and impact in healthcare delivery, Wellstar Health System has launched Catalyst by WellstarTM, a global digital health and innovation center.
As part of the center’s work, Wellstar has partnered with corporate innovation and venture platform Engage to connect and collaborate with industry-leading corporations, enterprise startups, and universities to fuel innovation. To foster meaningful discussion, action, and philanthropy around healthcare innovation, the Catalyst by Wellstar leadership team will participate in a Wellstar Foundation-hosted Innovation Series virtual event on June 15.
Catalyst by Wellstar designed to drive disruptive innovation
Catalyst by Wellstar is the first-of-its-kind global digital health and innovation center created and operated within a health system to holistically address healthcare disruption by harnessing problems, solutions, investments, and partnerships across industries. The center defines and drives leading-edge, transformative solutions that enhance the health and well-being of people and communities with world-class results and impact.
As technology continues to advance and consumers become more empowered by digital solutions and information access, innovation to solve problems and seize opportunities will evolve and impact how healthcare is delivered and used. Wellstar is committed to transforming healthcare through problem sourcing from patients, community members, physicians and team members, and partners to lead mission-driven innovation. Catalyst by Wellstar is designed to harness, accelerate, optimize, and scale people-centric solutions that:
- Disrupt how Wellstar delivers care to create better patient and provider experiences.
- Maximize quality and safety to improve outcomes while reducing the total cost of care.
- Enhance health and well-being for people through access, engagement, and empowerment.
- Optimize enterprise performance excellence, efficiencies, and productivity.
- Impact communities and the world by designing the future of healthcare.
“Innovation is vital to our mission of enhancing the health and well-being of every person we serve, today and into the future,” said Candice L. Saunders, president and CEO, Wellstar Health System. “Catalyst by Wellstar positions us to lead change across our system, communities, and the healthcare industry.”
Catalyst by Wellstar convenes and activates best-in-class entrepreneurs, philanthropists, innovation ecosystems, research and development experts, corporate partners, academicians and scientists, and thought leaders inside and outside of the healthcare industry. The center will encompass innovation that drives positive impact related to:
- Sustainability
- Aging and children
- Health equity
“There is endless opportunity to transform healthcare in positive and meaningful ways,” said Dr. Hank Capps, executive vice president and chief information and digital officer, Wellstar Health System. “With Catalyst by Wellstar, our system is poised to purposefully drive innovation faster than the speed of change through thought leadership and collaboration. Our global digital health and innovation center will equip Wellstar to transform the way healthcare is delivered for years to come.”
Wellstar invests in Engage corporate venture platform to fuel innovation
The first Catalyst by Wellstar partnership is an investment in Atlanta-based Engage, a first-of-its-kind collaborative innovation and corporate venture platform. Engage brings together industry-leading corporations, enterprise startups, and universities with the shared mission of elevating Atlanta and the Southeast as a leading technology and innovation hub. Wellstar is the only healthcare company to partner with Engage. Saunders has joined Engage’s board of directors and Capps has been named to the Engage Advisory Board.
“As a regional and national healthcare leader, Wellstar brings critical industry perspective to the Engage platform,” said Daley Ervin, managing director of Engage. “Our corporate partners are facing challenges posed by large-scale digital transformation and rapidly evolving customer expectations. Through this partnership, Wellstar will benefit from the expertise of a broad network of industry-leading companies while also leveraging the startup and university research ecosystem on their journey to design the future of healthcare.”
As a result of Wellstar’s investment in Engage, the system will have the opportunity to collaborate with startup technology companies as part of the innovation process, alongside other Engage partners: Chick-fil-A, Cox Enterprises, Delta Air Lines, Georgia-Pacific, Georgia Power Foundation, Georgia Tech, Goldman Sachs, The Home Depot, Inspire Brands, Intercontinental Exchange, Invesco, Invest Georgia, Tech Square Ventures, and UPS. The Engage Fund is managed by Tech Square Ventures. Engage’s exclusive partnership with Georgia Tech, one of the country’s top research and technology commercialization universities, provides unique access to its startup, innovation, and research initiatives.
“Healthcare is one of the strategic areas of focus for UPS and I am thrilled to welcome Wellstar to the Engage partnership," said Matt Guffey, president of Global Strategy and Transformation at UPS and Engage Advisory Board member.
Wellstar Foundation Healthcare Innovation Series to foster discussion about the future of healthcare
The second Wellstar Foundation Healthcare Innovation Series virtual roundtable will take place on June 15, 2021 from noon to 1:30 p.m. The event will focus on “Designing the Future of Healthcare,” with emphasis on the role of technology and innovation. The Series convenes community, philanthropic, and thought leaders to facilitate conversation and collaboration to propel the transformation of healthcare. More than 100 participants attended the inaugural event and engaged in discussion about how to enhance health equity. For more information, contact [email protected].
;

This month Wellstar Health System announced it is extending its partnership with Moth+Flame to further utilize its virtual reality (VR) training technology throughout the enterprise.
Moth+Flame is an award-winning VR communication technology developer and premier enterprise-grade immersive learning provider offering innovative and adaptive learning programs for mastering technical and cognitive skills. Their platform includes content focused on emotional intelligence. When learners put on their headsets, they inhabit and interact with immersive simulated environments. They decide in the moment how to respond and see for themselves the impact their words and decisions have on others — and reflect on how to improve. Trainees receive an empathy rating score at the end of their session.
Last May, Catalyst by Wellstar led Wellstar’s first-ever VR-based leadership development training in collaboration with Moth+Flame. This was Moth+Flame’s first healthcare partnership, and the use of this technology continues to expand within Wellstar’s enterprise.
Following the training, 97% of participants recommended the virtual learning experience to others. They also reported that the training reduced their anxiety around difficult conversations by 57%. As a result of the successful pilot, Wellstar decided to offer VR emotional intelligence training regularly.
“We believe strongly that immersive learning is the future of learning and builds more confidence through practice,” said Kevin Cornish, CEO and founder at Moth+Flame. “Using virtual reality puts you inside of a difficult conversation and gives you a chance to learn in a safe simulated environment.”
The VR emotional intelligence training encourages Wellstar’s employees to build composure and gain practical experience in a highly realistic scenario by navigating difficult conversations and testing resiliency in an emotionally charged environment. This experience helps Wellstar’s workforce develop strategies to build situational awareness and prioritize composure, critical thinking and conscious emotional responses when engaging in triggering conversations.
By gaining conversational expertise and knowledge, Wellstar’s team will know how to respond in real scenarios with the confidence to interact appropriately and strategically.
“The realism within Moth+Flame's VR experiences, from using real-life actors, dramatically increases the emotional connection to the content and helps learners retain the information they learn. We are grateful for Moth+Flame's partnership in helping introduce VR to our leaders,” said Steven LeClercq, executive director of learning and onboarding at Wellstar Health System.
This use of innovation keeps Wellstar on the leading edge of training and team development, and the organization will continue to explore use cases for this technology within a clinical setting.
;
Building on a rich history of innovation and impact in healthcare delivery, Wellstar Health System has launched Catalyst by WellstarTM, a global digital health and innovation center.
As part of the center’s work, Wellstar has partnered with corporate innovation and venture platform Engage to connect and collaborate with industry-leading corporations, enterprise startups, and universities to fuel innovation. To foster meaningful discussion, action, and philanthropy around healthcare innovation, the Catalyst by Wellstar leadership team will participate in a Wellstar Foundation-hosted Innovation Series virtual event on June 15.
Catalyst by Wellstar designed to drive disruptive innovation
Catalyst by Wellstar is the first-of-its-kind global digital health and innovation center created and operated within a health system to holistically address healthcare disruption by harnessing problems, solutions, investments, and partnerships across industries. The center defines and drives leading-edge, transformative solutions that enhance the health and well-being of people and communities with world-class results and impact.
As technology continues to advance and consumers become more empowered by digital solutions and information access, innovation to solve problems and seize opportunities will evolve and impact how healthcare is delivered and used. Wellstar is committed to transforming healthcare through problem sourcing from patients, community members, physicians and team members, and partners to lead mission-driven innovation. Catalyst by Wellstar is designed to harness, accelerate, optimize, and scale people-centric solutions that:
- Disrupt how Wellstar delivers care to create better patient and provider experiences.
- Maximize quality and safety to improve outcomes while reducing the total cost of care.
- Enhance health and well-being for people through access, engagement, and empowerment.
- Optimize enterprise performance excellence, efficiencies, and productivity.
- Impact communities and the world by designing the future of healthcare.
“Innovation is vital to our mission of enhancing the health and well-being of every person we serve, today and into the future,” said Candice L. Saunders, president and CEO, Wellstar Health System. “Catalyst by Wellstar positions us to lead change across our system, communities, and the healthcare industry.”
Catalyst by Wellstar convenes and activates best-in-class entrepreneurs, philanthropists, innovation ecosystems, research and development experts, corporate partners, academicians and scientists, and thought leaders inside and outside of the healthcare industry. The center will encompass innovation that drives positive impact related to:
- Sustainability
- Aging and children
- Health equity
“There is endless opportunity to transform healthcare in positive and meaningful ways,” said Dr. Hank Capps, executive vice president and chief information and digital officer, Wellstar Health System. “With Catalyst by Wellstar, our system is poised to purposefully drive innovation faster than the speed of change through thought leadership and collaboration. Our global digital health and innovation center will equip Wellstar to transform the way healthcare is delivered for years to come.”
Wellstar invests in Engage corporate venture platform to fuel innovation
The first Catalyst by Wellstar partnership is an investment in Atlanta-based Engage, a first-of-its-kind collaborative innovation and corporate venture platform. Engage brings together industry-leading corporations, enterprise startups, and universities with the shared mission of elevating Atlanta and the Southeast as a leading technology and innovation hub. Wellstar is the only healthcare company to partner with Engage. Saunders has joined Engage’s board of directors and Capps has been named to the Engage Advisory Board.
“As a regional and national healthcare leader, Wellstar brings critical industry perspective to the Engage platform,” said Daley Ervin, managing director of Engage. “Our corporate partners are facing challenges posed by large-scale digital transformation and rapidly evolving customer expectations. Through this partnership, Wellstar will benefit from the expertise of a broad network of industry-leading companies while also leveraging the startup and university research ecosystem on their journey to design the future of healthcare.”
As a result of Wellstar’s investment in Engage, the system will have the opportunity to collaborate with startup technology companies as part of the innovation process, alongside other Engage partners: Chick-fil-A, Cox Enterprises, Delta Air Lines, Georgia-Pacific, Georgia Power Foundation, Georgia Tech, Goldman Sachs, The Home Depot, Inspire Brands, Intercontinental Exchange, Invesco, Invest Georgia, Tech Square Ventures, and UPS. The Engage Fund is managed by Tech Square Ventures. Engage’s exclusive partnership with Georgia Tech, one of the country’s top research and technology commercialization universities, provides unique access to its startup, innovation, and research initiatives.
“Healthcare is one of the strategic areas of focus for UPS and I am thrilled to welcome Wellstar to the Engage partnership," said Matt Guffey, president of Global Strategy and Transformation at UPS and Engage Advisory Board member.
Wellstar Foundation Healthcare Innovation Series to foster discussion about the future of healthcare
The second Wellstar Foundation Healthcare Innovation Series virtual roundtable will take place on June 15, 2021 from noon to 1:30 p.m. The event will focus on “Designing the Future of Healthcare,” with emphasis on the role of technology and innovation. The Series convenes community, philanthropic, and thought leaders to facilitate conversation and collaboration to propel the transformation of healthcare. More than 100 participants attended the inaugural event and engaged in discussion about how to enhance health equity. For more information, contact [email protected].
;

For the first time, people in Paulding County and nearby communities have access to leading-edge robotic surgery close to home. Wellstar Health System launched a new robotic surgery program at Wellstar Paulding Medical Center.
“We’re thrilled to offer access to game-changing da Vinci robotic surgery at Wellstar Paulding Medical Center for the first time in history,” said Ralph Turner, Wellstar senior vice president and president of Wellstar Paulding Medical Center.
Robotic technology enables surgeons to make highly precise incisions smaller than the human hand can make — as tiny as a keyhole. As a result, people who have robotic surgery typically experience less blood loss, recovery pain and scarring.
“Robotic surgeries are minimally-invasive, which typically means shorter hospital stays and faster recoveries,” said Dr. Beau Dusseault, a urologist who leads the robotics program at Wellstar Paulding Medical Center.
He performed the first robotic surgery at the hospital, assisted by the $1.8 million da Vinci Xi Surgical System, on August 22. Dr. Dusseault has performed more than 440 robotic surgeries for prostate cancer and urinary tract conditions.
Experienced urologists and general surgeons are the first to offer robotic surgery at Wellstar Paulding Medical Center, primarily treating:
- Cancers such as prostate, kidney and bladder cancers
- Conditions in the kidneys, bladder and urinary tract
- Hernias and other conditions that require general surgery
The surgical team named the robot “Rosie,” a reference to the robotic maid from the 1960s sitcom “The Jetsons.” It is one of 14 robotic systems patients can benefit from at nine Wellstar locations.
“While our robotic surgery program is new to Paulding, we have high-volume robotic experience that we are bringing from the other Wellstar hospitals,” Dr. Dusseault added.

For a child, going to the hospital can be scary. That’s why Wellstar Douglas Hospital’s new $5.7 million Pediatric Emergency Department (ED) offers a kid-friendly and kid-sized experience for Douglas County’s youngest patients. The nautical-themed 7,600 square-foot facility provides specialized care for children from birth to 18 years of age.
The world-class “just-for-kids” facility has a separate entrance and waiting room from the main Emergency Department and is currently open from 11 a.m. to 11 p.m. The ten treatment rooms feature child-sized furniture, equipment and supplies.
“We created an environment that is optimum for healing and that helps our youngest patients feel as comfortable as possible,” said Dr. Avril Beckford, chief pediatric officer, Wellstar Health System. “Children in Douglas deserve to see doctors and nurses who understand them. We also wanted to give parents a state-of-the-art facility staffed by pediatric physicians close to home – there is no need to travel long distances with a sick child now, because this specialized facility is right here, in the Douglas County community.”
A deeper dive into kid-friendly care
Staffed by kid-friendly nurses and skilled providers devoted to children, the new kids’ ED is a result of collaboration between the architect, construction firm and pediatric experts. Wellstar’s pediatric team cares for children at more than 114,000 emergency visits a year across Wellstar’s hospitals.
“From the outside, there are colorful floor-to-ceiling glass windows,” Dr. Beckford said, as she imagined a child’s first impression. “It feels almost like you’re walking into an aquarium.”
Inside the pediatric ED, children and their parents are greeted by warm staff members, soothing murals of ocean life, a large flat screen TV and child-sized furnishings.
To help children be seen and treated more quickly, some rooms will be dedicated to patients with less serious conditions – such as sore throats and sprains. There will also be a trauma bay and a dedicated room for adolescent gynecological concerns.
;
Access to care close to home is something many take for granted until that care is no longer available. Georgia’s rural hospitals provide critical care to residents when and where they need it. However, industry shifts and economic challenges have forced many rural hospitals to close their doors, forcing millions of people to commute — some for hours — to receive the care they need.
Recognizing this strain on rural hospitals and the communities they serve, the Georgia legislature launched the Georgia Rural Hospital Tax Credit program. Through this program, Georgia taxpayers receive a 100% state income tax credit on contributions made to qualifying rural hospitals such as Wellstar Sylvan Grove Hospital.
Dollars making a difference
As in past years, contribution limits will be removed on July 1, 2022. Given recent enhancements and increased interest, the program is anticipated to reach its $60 million cap soon after the contribution limits are removed, making now a pivotal time for Sylvan Grove donors to pre-register for unlimited contributions. By registering your contribution early, you help ensure facilities like Wellstar Sylvan Grove Hospital receive the assistance they need.
Starting May 16, 2022 at 9 a.m., our administrative partner — Georgia HEART— will accept pre-registrations to be loaded on a first-come-first-serve basis once the limits are removed. The Wellstar Foundation is offering to assist Wellstar Sylvan Grove Hospital contributors with this pre-registration process. Contact the Foundation at [email protected] for assistance or click here to pre-register directly with Georgia HEART on May 16, 2022.
Since 2016, Wellstar Sylvan Grove Hospital has received a total of $10 million through this program. As facilitated through the Wellstar Foundation, every dollar has accelerated critical upgrades, including a full renovation of the hospital’s emergency department, radiology department expansion and leading-edge innovation, such as advanced CT scanning technology, that enhances physicians’ abilities to make better-informed medical decisions.
Providing PeopleCare
Advancements in treatments and technology benefit the residents of Butts County — patients like Mary “Lee” Nelson, a retired Butts County teacher who turned to Wellstar Sylvan Grove Hospital’s outpatient rehabilitation center for post-surgical physical therapy. The outpatient center was recently renovated with state-of-the-art equipment made possible through tax credit program contributions.
The former elementary grade teacher spends her retirement days traveling with her husband Bill, tending to her flower gardens and caring for her chickens. With such an active lifestyle, when Lee learned that she needed a knee replacement in 2021, she knew her local hospital would be able to provide the high-quality, compassionate care needed to get her back on her feet safely and quickly. Now, a few months after completing her physical therapy, Lee shares that she “feels normal again” and able to enjoy all the things that once brought her life so much joy.
How you can help
Through corporate and community partnership, the Wellstar Foundation is fueling innovation and action to address the vital needs of diverse communities in Georgia, including urban, suburban and rural communities. Wellstar is committed to delivering world-class healthcare to everyone close to home. Philanthropic support of the Wellstar Foundation is advancing innovation and expanding resources to create a healthier Georgia for all. To learn more, visit wellstar.org/foundation or contact the Wellstar Foundation at (770) 956-GIVE (4483).
;
For the first time, people in Paulding County and nearby communities have access to leading-edge robotic surgery close to home. Wellstar Health System launched a new robotic surgery program at Wellstar Paulding Medical Center.
“We’re thrilled to offer access to game-changing da Vinci robotic surgery at Wellstar Paulding Medical Center for the first time in history,” said Ralph Turner, Wellstar senior vice president and president of Wellstar Paulding Medical Center.
Robotic technology enables surgeons to make highly precise incisions smaller than the human hand can make — as tiny as a keyhole. As a result, people who have robotic surgery typically experience less blood loss, recovery pain and scarring.
“Robotic surgeries are minimally-invasive, which typically means shorter hospital stays and faster recoveries,” said Dr. Beau Dusseault, a urologist who leads the robotics program at Wellstar Paulding Medical Center.
He performed the first robotic surgery at the hospital, assisted by the $1.8 million da Vinci Xi Surgical System, on August 22. Dr. Dusseault has performed more than 440 robotic surgeries for prostate cancer and urinary tract conditions.
Experienced urologists and general surgeons are the first to offer robotic surgery at Wellstar Paulding Medical Center, primarily treating:
- Cancers such as prostate, kidney and bladder cancers
- Conditions in the kidneys, bladder and urinary tract
- Hernias and other conditions that require general surgery
The surgical team named the robot “Rosie,” a reference to the robotic maid from the 1960s sitcom “The Jetsons.” It is one of 14 robotic systems patients can benefit from at nine Wellstar locations.
“While our robotic surgery program is new to Paulding, we have high-volume robotic experience that we are bringing from the other Wellstar hospitals,” Dr. Dusseault added.

The system continues to build on its legacy and commitment to serving communities by actively listening to best understand and respond to what consumers want, need, and expect from their healthcare provider.
“As a leader in healthcare, we must take action to meet the evolving needs of people and communities. Health equity connects to everything we do, and recognizing hardships, disparities, and inequities is just the first step,” said Candice L. Saunders, president and CEO of Wellstar Health System. “Through strategic partnerships and programs, Wellstar is committed to supporting people and communities to make a tangible and lasting difference, enhancing the health and well-being of everyone we serve.”
Wellstar Center for Health Equity addresses community needs at a grassroots level
The Wellstar Center for Health Equity (WCHE) – an extension of Wellstar’s long history of community engagement and allyship to provide people-centric care – was formed to drive lasting change at a grassroots level. The six areas of focus were informed by Wellstar’s triennial Community Health Needs Assessment (CHNA) of 2019: Primary Care, Behavioral Health, Food Insecurity, Suicide, Cancer, Women’s Health.
Each of these strategic domains connects to Wellstar medical service lines to bring to bear the deep expertise and broad bench of resources needed to identify pertinent needs, relevant partnerships, and viable programs.
To create meaningful impact, Wellstar has forged strategic partnerships with government agencies, businesses, philanthropies, non-profit organizations, academia, and citizens. Examples of how WCHE has activated resources in the community include:
Walk-up, pop-up family COVID-19 testing: With the support of community partners, Wellstar conducts free walk-up, pop-up family testing at churches and school lunch pick-up sites and distributes safety kits in English and Spanish. To-date, WCHE has orchestrated 29 pop-up testing sites, administered over 3,000 COVID tests, and distributed more than 51,000 wellness kits with culturally and linguistically appropriate safety information.
Reaching faith-based congregants with vital information and vaccines: WCHE is hosting a series of community town halls to debunk myths about COVID-19 and vaccines in partnership with the Wellstar Congregational Health Network. In April, WCHE hosted a Hispanic town hall to address community questions and launched a series of equity-centric and language-proficient vaccination clinics for congregants at faith-based organizations.
Providing nutritious meals to food-insecure communities: In partnership with Goodr, an organization that provides food resources for people in need, and funded in part by Wellstar Foundation donations, the WCHE “Mobile Market” hosts “pop-up” farmers’ markets in seven communities, feeding over 700 families monthly.
Enabling technology-driven community health transformation: WCHE launched a year-long initiative to enhance access to medical care via technology with leading community partners. Supported by contributions to the Wellstar Foundation, the “Community Health Transformation” program enables the following community organizations to reach, engage, and support at-risk individuals with measurable results: Bethesda Community Clinic; Empowerment Resource Center; Healthy Mothers, Healthy Babies Coalition of Georgia; Good Samaritan Health Center of Cobb; and MUST Ministries.
Anchoring vulnerable patients with vital healthcare resources: When the Centers for Disease Control and Prevention (CDC) reported that 80% of COVID-19 patients in eight Georgia areas were Black people, WCHE developed “Anchoring Vulnerable Patients,” a project in Clayton County to assess and address the medical and social needs of Black patients with co-morbidities that put them at risk for contracting COVID-19.
;
Wellstar Health System, one of Georgia’s largest and most integrated healthcare systems, announced that the Wellstar Cancer Network was recently recognized nationally as a cancer treatment leader. Honored with an Outstanding Achievement Award from the American College of Surgeons Commission on Cancer and designated as a Care Continuum Center of Excellence by the GO2 Foundation for Lung Cancer, the Wellstar Cancer Network continues to pioneer innovative cancer treatments and technologies to improve outcomes and quality of life for patients.
“Wellstar Health System is dedicated to providing patients with the highest quality of compassionate and personalized care,” said Dr. Michael Andrews, Chief Cancer Officer of the Wellstar Cancer Network. “We are extremely proud of the Wellstar Cancer Network and our team of highly skilled physicians, nurses and oncology support services who excel at treating the spectrum of cancer illnesses with the most advanced, patient-centric technologies and treatments. We are focused on enhancing the health and well-being of everyone we serve, with a commitment to delivering world-class cancer care.”
Wellstar earned an Outstanding Achievement Award for the third consecutive cycle from the American College of Surgeons Commission on Cancer (CoC). The highest honor in the United States awarded to a cancer program, the Wellstar Cancer Network was recognized for achieving excellence in providing care to cancer patients. Award recipients must have received commendation ratings in all seven commendation standards and receive a compliance rating for each of the 27 remaining cancer program standards.

UnitedHealthcare and Wellstar Health System have reached a multi-year agreement that restores network access to Wellstar’s clinicians, hospitals, health parks and clinics for people enrolled in UnitedHealthcare employer-sponsored, individual and Medicare Advantage plans, effective July 1, 2022. The agreement also expands access to Wellstar Clinical Partners, skilled nursing facilities, home health and hospice care.
UnitedHealthcare members can begin scheduling appointments with Wellstar today through MyChart or by calling their clinician’s office. For more information, call 770-956-STAR (7827).
“We know how important it is for patients to have local access to high-quality care from the doctors and hospitals they know and trust,” said Candice L. Saunders, President and CEO of Wellstar Health System. “This agreement will offer expanded access and more convenient options for patients with UnitedHealthcare insurance.”
“The care that Wellstar provides to our members is important and personal to them,” said Junior Harewood, CEO of UnitedHealthcare Georgia. “Our top priority throughout this negotiation has been ensuring the people and employers we’re honored to serve in Georgia have access to quality, more affordable health care, and this new agreement helps accomplish that goal.”
Wellstar’s mission is to enhance the health and well-being of every person they serve and provides access to compassionate, high-quality care to 1 in 6 Georgians through 10 hospitals, 300+ medical office locations, 9 cancer centers, 74 rehabilitation centers, 3 hospice facilities, 1 retirement village, 34 imaging centers, 18 urgent care locations and 5 health parks.
In Georgia, UnitedHealthcare serves nearly 1.2 million people through a network of more than 150 hospitals and nearly 35,000 physicians and other care providers.
;
Access to care close to home is something many take for granted until that care is no longer available. Georgia’s rural hospitals provide critical care to residents when and where they need it. However, industry shifts and economic challenges have forced many rural hospitals to close their doors, forcing millions of people to commute — some for hours — to receive the care they need.
Recognizing this strain on rural hospitals and the communities they serve, the Georgia legislature launched the Georgia Rural Hospital Tax Credit program. Through this program, Georgia taxpayers receive a 100% state income tax credit on contributions made to qualifying rural hospitals such as Wellstar Sylvan Grove Hospital.
Dollars making a difference
As in past years, contribution limits will be removed on July 1, 2022. Given recent enhancements and increased interest, the program is anticipated to reach its $60 million cap soon after the contribution limits are removed, making now a pivotal time for Sylvan Grove donors to pre-register for unlimited contributions. By registering your contribution early, you help ensure facilities like Wellstar Sylvan Grove Hospital receive the assistance they need.
Starting May 16, 2022 at 9 a.m., our administrative partner — Georgia HEART— will accept pre-registrations to be loaded on a first-come-first-serve basis once the limits are removed. The Wellstar Foundation is offering to assist Wellstar Sylvan Grove Hospital contributors with this pre-registration process. Contact the Foundation at [email protected] for assistance or click here to pre-register directly with Georgia HEART on May 16, 2022.
Since 2016, Wellstar Sylvan Grove Hospital has received a total of $10 million through this program. As facilitated through the Wellstar Foundation, every dollar has accelerated critical upgrades, including a full renovation of the hospital’s emergency department, radiology department expansion and leading-edge innovation, such as advanced CT scanning technology, that enhances physicians’ abilities to make better-informed medical decisions.
Providing PeopleCare
Advancements in treatments and technology benefit the residents of Butts County — patients like Mary “Lee” Nelson, a retired Butts County teacher who turned to Wellstar Sylvan Grove Hospital’s outpatient rehabilitation center for post-surgical physical therapy. The outpatient center was recently renovated with state-of-the-art equipment made possible through tax credit program contributions.
The former elementary grade teacher spends her retirement days traveling with her husband Bill, tending to her flower gardens and caring for her chickens. With such an active lifestyle, when Lee learned that she needed a knee replacement in 2021, she knew her local hospital would be able to provide the high-quality, compassionate care needed to get her back on her feet safely and quickly. Now, a few months after completing her physical therapy, Lee shares that she “feels normal again” and able to enjoy all the things that once brought her life so much joy.
How you can help
Through corporate and community partnership, the Wellstar Foundation is fueling innovation and action to address the vital needs of diverse communities in Georgia, including urban, suburban and rural communities. Wellstar is committed to delivering world-class healthcare to everyone close to home. Philanthropic support of the Wellstar Foundation is advancing innovation and expanding resources to create a healthier Georgia for all. To learn more, visit wellstar.org/foundation or contact the Wellstar Foundation at (770) 956-GIVE (4483).
;
For a child, going to the hospital can be scary. That’s why Wellstar Douglas Hospital’s new $5.7 million Pediatric Emergency Department (ED) offers a kid-friendly and kid-sized experience for Douglas County’s youngest patients. The nautical-themed 7,600 square-foot facility provides specialized care for children from birth to 18 years of age.
The world-class “just-for-kids” facility has a separate entrance and waiting room from the main Emergency Department and is currently open from 11 a.m. to 11 p.m. The ten treatment rooms feature child-sized furniture, equipment and supplies.
“We created an environment that is optimum for healing and that helps our youngest patients feel as comfortable as possible,” said Dr. Avril Beckford, chief pediatric officer, Wellstar Health System. “Children in Douglas deserve to see doctors and nurses who understand them. We also wanted to give parents a state-of-the-art facility staffed by pediatric physicians close to home – there is no need to travel long distances with a sick child now, because this specialized facility is right here, in the Douglas County community.”
A deeper dive into kid-friendly care
Staffed by kid-friendly nurses and skilled providers devoted to children, the new kids’ ED is a result of collaboration between the architect, construction firm and pediatric experts. Wellstar’s pediatric team cares for children at more than 114,000 emergency visits a year across Wellstar’s hospitals.
“From the outside, there are colorful floor-to-ceiling glass windows,” Dr. Beckford said, as she imagined a child’s first impression. “It feels almost like you’re walking into an aquarium.”
Inside the pediatric ED, children and their parents are greeted by warm staff members, soothing murals of ocean life, a large flat screen TV and child-sized furnishings.
To help children be seen and treated more quickly, some rooms will be dedicated to patients with less serious conditions – such as sore throats and sprains. There will also be a trauma bay and a dedicated room for adolescent gynecological concerns.
;
For a child, going to the hospital can be scary. That’s why Wellstar Douglas Hospital’s new $5.7 million Pediatric Emergency Department (ED) offers a kid-friendly and kid-sized experience for Douglas County’s youngest patients. The nautical-themed 7,600 square-foot facility provides specialized care for children from birth to 18 years of age.
The world-class “just-for-kids” facility has a separate entrance and waiting room from the main Emergency Department and is currently open from 11 a.m. to 11 p.m. The ten treatment rooms feature child-sized furniture, equipment and supplies.
“We created an environment that is optimum for healing and that helps our youngest patients feel as comfortable as possible,” said Dr. Avril Beckford, chief pediatric officer, Wellstar Health System. “Children in Douglas deserve to see doctors and nurses who understand them. We also wanted to give parents a state-of-the-art facility staffed by pediatric physicians close to home – there is no need to travel long distances with a sick child now, because this specialized facility is right here, in the Douglas County community.”
A deeper dive into kid-friendly care
Staffed by kid-friendly nurses and skilled providers devoted to children, the new kids’ ED is a result of collaboration between the architect, construction firm and pediatric experts. Wellstar’s pediatric team cares for children at more than 114,000 emergency visits a year across Wellstar’s hospitals.
“From the outside, there are colorful floor-to-ceiling glass windows,” Dr. Beckford said, as she imagined a child’s first impression. “It feels almost like you’re walking into an aquarium.”
Inside the pediatric ED, children and their parents are greeted by warm staff members, soothing murals of ocean life, a large flat screen TV and child-sized furnishings.
To help children be seen and treated more quickly, some rooms will be dedicated to patients with less serious conditions – such as sore throats and sprains. There will also be a trauma bay and a dedicated room for adolescent gynecological concerns.
;
For the first time, people in Paulding County and nearby communities have access to leading-edge robotic surgery close to home. Wellstar Health System launched a new robotic surgery program at Wellstar Paulding Medical Center.
“We’re thrilled to offer access to game-changing da Vinci robotic surgery at Wellstar Paulding Medical Center for the first time in history,” said Ralph Turner, Wellstar senior vice president and president of Wellstar Paulding Medical Center.
Robotic technology enables surgeons to make highly precise incisions smaller than the human hand can make — as tiny as a keyhole. As a result, people who have robotic surgery typically experience less blood loss, recovery pain and scarring.
“Robotic surgeries are minimally-invasive, which typically means shorter hospital stays and faster recoveries,” said Dr. Beau Dusseault, a urologist who leads the robotics program at Wellstar Paulding Medical Center.
He performed the first robotic surgery at the hospital, assisted by the $1.8 million da Vinci Xi Surgical System, on August 22. Dr. Dusseault has performed more than 440 robotic surgeries for prostate cancer and urinary tract conditions.
Experienced urologists and general surgeons are the first to offer robotic surgery at Wellstar Paulding Medical Center, primarily treating:
- Cancers such as prostate, kidney and bladder cancers
- Conditions in the kidneys, bladder and urinary tract
- Hernias and other conditions that require general surgery
The surgical team named the robot “Rosie,” a reference to the robotic maid from the 1960s sitcom “The Jetsons.” It is one of 14 robotic systems patients can benefit from at nine Wellstar locations.
“While our robotic surgery program is new to Paulding, we have high-volume robotic experience that we are bringing from the other Wellstar hospitals,” Dr. Dusseault added.

This month Wellstar Health System announced it is extending its partnership with Moth+Flame to further utilize its virtual reality (VR) training technology throughout the enterprise.
Moth+Flame is an award-winning VR communication technology developer and premier enterprise-grade immersive learning provider offering innovative and adaptive learning programs for mastering technical and cognitive skills. Their platform includes content focused on emotional intelligence. When learners put on their headsets, they inhabit and interact with immersive simulated environments. They decide in the moment how to respond and see for themselves the impact their words and decisions have on others — and reflect on how to improve. Trainees receive an empathy rating score at the end of their session.
Last May, Catalyst by Wellstar led Wellstar’s first-ever VR-based leadership development training in collaboration with Moth+Flame. This was Moth+Flame’s first healthcare partnership, and the use of this technology continues to expand within Wellstar’s enterprise.
Following the training, 97% of participants recommended the virtual learning experience to others. They also reported that the training reduced their anxiety around difficult conversations by 57%. As a result of the successful pilot, Wellstar decided to offer VR emotional intelligence training regularly.
“We believe strongly that immersive learning is the future of learning and builds more confidence through practice,” said Kevin Cornish, CEO and founder at Moth+Flame. “Using virtual reality puts you inside of a difficult conversation and gives you a chance to learn in a safe simulated environment.”
The VR emotional intelligence training encourages Wellstar’s employees to build composure and gain practical experience in a highly realistic scenario by navigating difficult conversations and testing resiliency in an emotionally charged environment. This experience helps Wellstar’s workforce develop strategies to build situational awareness and prioritize composure, critical thinking and conscious emotional responses when engaging in triggering conversations.
By gaining conversational expertise and knowledge, Wellstar’s team will know how to respond in real scenarios with the confidence to interact appropriately and strategically.
“The realism within Moth+Flame's VR experiences, from using real-life actors, dramatically increases the emotional connection to the content and helps learners retain the information they learn. We are grateful for Moth+Flame's partnership in helping introduce VR to our leaders,” said Steven LeClercq, executive director of learning and onboarding at Wellstar Health System.
This use of innovation keeps Wellstar on the leading edge of training and team development, and the organization will continue to explore use cases for this technology within a clinical setting.
;
The system continues to build on its legacy and commitment to serving communities by actively listening to best understand and respond to what consumers want, need, and expect from their healthcare provider.
“As a leader in healthcare, we must take action to meet the evolving needs of people and communities. Health equity connects to everything we do, and recognizing hardships, disparities, and inequities is just the first step,” said Candice L. Saunders, president and CEO of Wellstar Health System. “Through strategic partnerships and programs, Wellstar is committed to supporting people and communities to make a tangible and lasting difference, enhancing the health and well-being of everyone we serve.”
Wellstar Center for Health Equity addresses community needs at a grassroots level
The Wellstar Center for Health Equity (WCHE) – an extension of Wellstar’s long history of community engagement and allyship to provide people-centric care – was formed to drive lasting change at a grassroots level. The six areas of focus were informed by Wellstar’s triennial Community Health Needs Assessment (CHNA) of 2019: Primary Care, Behavioral Health, Food Insecurity, Suicide, Cancer, Women’s Health.
Each of these strategic domains connects to Wellstar medical service lines to bring to bear the deep expertise and broad bench of resources needed to identify pertinent needs, relevant partnerships, and viable programs.
To create meaningful impact, Wellstar has forged strategic partnerships with government agencies, businesses, philanthropies, non-profit organizations, academia, and citizens. Examples of how WCHE has activated resources in the community include:
Walk-up, pop-up family COVID-19 testing: With the support of community partners, Wellstar conducts free walk-up, pop-up family testing at churches and school lunch pick-up sites and distributes safety kits in English and Spanish. To-date, WCHE has orchestrated 29 pop-up testing sites, administered over 3,000 COVID tests, and distributed more than 51,000 wellness kits with culturally and linguistically appropriate safety information.
Reaching faith-based congregants with vital information and vaccines: WCHE is hosting a series of community town halls to debunk myths about COVID-19 and vaccines in partnership with the Wellstar Congregational Health Network. In April, WCHE hosted a Hispanic town hall to address community questions and launched a series of equity-centric and language-proficient vaccination clinics for congregants at faith-based organizations.
Providing nutritious meals to food-insecure communities: In partnership with Goodr, an organization that provides food resources for people in need, and funded in part by Wellstar Foundation donations, the WCHE “Mobile Market” hosts “pop-up” farmers’ markets in seven communities, feeding over 700 families monthly.
Enabling technology-driven community health transformation: WCHE launched a year-long initiative to enhance access to medical care via technology with leading community partners. Supported by contributions to the Wellstar Foundation, the “Community Health Transformation” program enables the following community organizations to reach, engage, and support at-risk individuals with measurable results: Bethesda Community Clinic; Empowerment Resource Center; Healthy Mothers, Healthy Babies Coalition of Georgia; Good Samaritan Health Center of Cobb; and MUST Ministries.
Anchoring vulnerable patients with vital healthcare resources: When the Centers for Disease Control and Prevention (CDC) reported that 80% of COVID-19 patients in eight Georgia areas were Black people, WCHE developed “Anchoring Vulnerable Patients,” a project in Clayton County to assess and address the medical and social needs of Black patients with co-morbidities that put them at risk for contracting COVID-19.
;
Wellstar Health System, one of Georgia’s largest and most integrated healthcare systems, announced that the Wellstar Cancer Network was recently recognized nationally as a cancer treatment leader. Honored with an Outstanding Achievement Award from the American College of Surgeons Commission on Cancer and designated as a Care Continuum Center of Excellence by the GO2 Foundation for Lung Cancer, the Wellstar Cancer Network continues to pioneer innovative cancer treatments and technologies to improve outcomes and quality of life for patients.
“Wellstar Health System is dedicated to providing patients with the highest quality of compassionate and personalized care,” said Dr. Michael Andrews, Chief Cancer Officer of the Wellstar Cancer Network. “We are extremely proud of the Wellstar Cancer Network and our team of highly skilled physicians, nurses and oncology support services who excel at treating the spectrum of cancer illnesses with the most advanced, patient-centric technologies and treatments. We are focused on enhancing the health and well-being of everyone we serve, with a commitment to delivering world-class cancer care.”
Wellstar earned an Outstanding Achievement Award for the third consecutive cycle from the American College of Surgeons Commission on Cancer (CoC). The highest honor in the United States awarded to a cancer program, the Wellstar Cancer Network was recognized for achieving excellence in providing care to cancer patients. Award recipients must have received commendation ratings in all seven commendation standards and receive a compliance rating for each of the 27 remaining cancer program standards.

Wellstar Health System, one of Georgia’s largest and most integrated healthcare systems, announced that the Wellstar Cancer Network was recently recognized nationally as a cancer treatment leader. Honored with an Outstanding Achievement Award from the American College of Surgeons Commission on Cancer and designated as a Care Continuum Center of Excellence by the GO2 Foundation for Lung Cancer, the Wellstar Cancer Network continues to pioneer innovative cancer treatments and technologies to improve outcomes and quality of life for patients.
“Wellstar Health System is dedicated to providing patients with the highest quality of compassionate and personalized care,” said Dr. Michael Andrews, Chief Cancer Officer of the Wellstar Cancer Network. “We are extremely proud of the Wellstar Cancer Network and our team of highly skilled physicians, nurses and oncology support services who excel at treating the spectrum of cancer illnesses with the most advanced, patient-centric technologies and treatments. We are focused on enhancing the health and well-being of everyone we serve, with a commitment to delivering world-class cancer care.”
Wellstar earned an Outstanding Achievement Award for the third consecutive cycle from the American College of Surgeons Commission on Cancer (CoC). The highest honor in the United States awarded to a cancer program, the Wellstar Cancer Network was recognized for achieving excellence in providing care to cancer patients. Award recipients must have received commendation ratings in all seven commendation standards and receive a compliance rating for each of the 27 remaining cancer program standards.
We use cookies for booking and general analytics. Learn more about or internet privacy policy.